Differential Adherence to Free and Single-Pill Combination of Rosuvastatin/Ezetimibe: Findings from a Real-World Analysis in Italy
- PMID: 38963586
- PMCID: PMC11263226
- DOI: 10.1007/s12325-024-02916-8
Differential Adherence to Free and Single-Pill Combination of Rosuvastatin/Ezetimibe: Findings from a Real-World Analysis in Italy
Abstract
Introduction: Adherence to cardiovascular drug treatment can significantly benefit from a reduced pill burden, but data on this matter derived from real-life settings are currently scanty. This analysis assessed the possible changes in adherence in patients treated with rosuvastatin and ezetimibe (ROS/EZE) as free multi-pill combination who switched to ROS/EZE as single-pill combination in the setting of real clinical practice in Italy.
Methods: A retrospective analysis was conducted on the administrative databases for a catchment area of about seven million health-assisted residents. Adults receiving ROS/EZE as a single-pill combination from January 2010 to June 2020 (followed up to 2021) were identified. The date of the first prescription of single-pill combination of ROS/EZE was considered as the index date. The analysis included the users of ROS/EZE as a free combination during the year before the index date. Baseline demographic and clinical characteristics were collected during the period of data availability prior to the index date. Adherence to therapy was evaluated as proportion of days covered (PDC), namely the percentage of days during which a patient had access to medication, in the 12-month interval preceding or following the index date (PDC < 25% non-adherence; PDC = 25-75% partial adherence; PDC > 75% adherence).
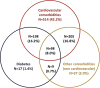
Results: A total of 1219 patients (61.1% male, aged 66.2 ± 10.4 years) were included. Cardiovascular comorbidities were found in 83.3% of them, diabetes in 26.4%, and a combination of both in 16.2%. Single-pill combination of ROS/EZE was associated with a higher proportion of adherent patients compared to free-pill combination (75.2% vs 51.8%, p < 0.001).
Conclusions: This real-world analysis suggested that switching from a regimen based on separate pills to one based on a single-pill combination resulted in improved adherence to ROS/EZE therapy.
Keywords: Adherence; Ezetimibe; Rosuvastatin; Single-pill combination.
Plain language summary
Lipid-lowering therapy to control low-density lipoprotein (LDL) cholesterol levels is essential for cardiovascular risk prevention. Successful therapy depends on the type of lipid-lowering therapy, i.e., low or high statin intensity and combination of statins with ezetimibe or proprotein convertase subtilisin/kexin type 9 (PCSK9) inhibitors, and adherence to therapy, i.e., whether the patient actually takes their pills as prescribed. If there are fewer pills to be taken, this can help patients to follow their treatment. Single-pill combinations of two drugs could facilitate adherence and thus the chances of reaching the recommended lipid targets. Here, we analyzed a sample of Italian patients with dyslipidemia to examine whether the switch from a free combination of two separate pills of rosuvastatin and ezetimibe to a single-pill combination of the same drugs could improve adherence to therapy. We found that the proportion of adherent patients increased from about just over half (51.8%) to about three-fourths (75.1%) when switching from two-pill to single-pill combination of rosuvastatin and ezetimibe. These findings suggest that simplifying therapy can help improve patient adherence, which is essential for reaching lipid targets and ultimately for alleviating atherosclerotic cardiovascular disease.
© 2024. The Author(s).
Conflict of interest statement
Leopoldo Perez de Isla reports research grants, speaker fees and consultant fees from Servier, Sanofi, Amgen, Daiichi-Sankyo and Merk. Evangelos Liberopoulos reports grants from Hellenic Atherosclerosis Society; personal fees and non-financial support from Amgen, personal fees from Sanofi, personal fees from Lilly, personal fees from Bayer, personal fees from Novo Nordisk, grants and personal fees from AstraZeneca, personal fees from Boehringer Ingelheim, personal fees from Novartis, personal fees from Servier, grants and personal fees from Viatris, outside the submitted work. Alberto Zambon reports speaker fees and consultant fees from Amgen, Amarin, Amryt, AlfaSigma, Abbott, Viatris, Novartis, Sanofi, Sobi, Servier, Daiichi Sankyo. Melania Dovizio, Chiara Veronesi, Luca Degli Esposti have no competing interests to disclose.
Figures


Similar articles
-
A real-world analysis of adherence, biochemical outcomes, and healthcare costs in patients treated with rosuvastatin/ezetimibe as single-pill combination vs. free combination in Italy.Eur Heart J Open. 2024 Aug 28;4(5):oeae074. doi: 10.1093/ehjopen/oeae074. eCollection 2024 Sep. Eur Heart J Open. 2024. PMID: 39310723 Free PMC article.
-
Adherence to Lipid-Lowering Treatment by Single-Pill Combination of Statin and Ezetimibe.Adv Ther. 2021 Oct;38(10):5270-5285. doi: 10.1007/s12325-021-01892-7. Epub 2021 Sep 3. Adv Ther. 2021. PMID: 34480293 Free PMC article.
-
Comparison of rosuvastatin 10 mg plus ezetimibe versus rosuvastatin 20 mg in atherosclerotic cardiovascular disease and type 2 diabetes.Sci Rep. 2025 May 8;15(1):16012. doi: 10.1038/s41598-025-00298-7. Sci Rep. 2025. PMID: 40341101 Free PMC article. Clinical Trial.
-
Fixed-dose combination of rosuvastatin and ezetimibe: treating hypercholesteremia according to cardiovascular risk.Expert Rev Clin Pharmacol. 2021 Jul;14(7):793-806. doi: 10.1080/17512433.2021.1925539. Epub 2021 May 24. Expert Rev Clin Pharmacol. 2021. PMID: 33970743
-
An overview of rosuvastatin/ezetimibe association for the treatment of hypercholesterolemia and mixed dyslipidemia.Expert Opin Pharmacother. 2020 Apr;21(5):531-539. doi: 10.1080/14656566.2020.1714028. Epub 2020 Feb 8. Expert Opin Pharmacother. 2020. PMID: 32036729 Review.
Cited by
-
A real-world analysis of adherence, biochemical outcomes, and healthcare costs in patients treated with rosuvastatin/ezetimibe as single-pill combination vs. free combination in Italy.Eur Heart J Open. 2024 Aug 28;4(5):oeae074. doi: 10.1093/ehjopen/oeae074. eCollection 2024 Sep. Eur Heart J Open. 2024. PMID: 39310723 Free PMC article.
-
Real-World Effectiveness of Rosuvastatin-Ezetimibe Single Pill (Rovazet®) in Korean Dyslipidemia Patients.J Clin Med. 2025 Aug 4;14(15):5480. doi: 10.3390/jcm14155480. J Clin Med. 2025. PMID: 40807110 Free PMC article.
-
Learnings from Implementation Strategies to Improve Lipid Management.Curr Cardiol Rep. 2025 Jan 8;27(1):9. doi: 10.1007/s11886-024-02174-8. Curr Cardiol Rep. 2025. PMID: 39775142 Free PMC article. Review.
References
-
- Borén J, Chapman MJ, Krauss RM, et al. Low-density lipoproteins cause atherosclerotic cardiovascular disease: pathophysiological, genetic, and therapeutic insights: a consensus statement from the European Atherosclerosis Society Consensus Panel. Eur Heart J. 2020;41(24):2313–30. 10.1093/eurheartj/ehz962 - DOI - PMC - PubMed
-
- Ference BA, Ginsberg HN, Graham I, et al. Low-density lipoproteins cause atherosclerotic cardiovascular disease. 1. Evidence from genetic, epidemiologic, and clinical studies. A consensus statement from the European Atherosclerosis Society Consensus Panel. Eur Heart J. 2017;38:2459–72. 10.1093/eurheartj/ehx144 - DOI - PMC - PubMed
-
- Grundy SM, Feingold KR. Guidelines for the management of high blood cholesterol. [Updated 2022 May 28]. In: Feingold KR, Anawalt B, Blackman MR, et al., editors. Endotext [Internet]. South Dartmouth (MA): MDText.com; 2000. https://www.ncbi.nlm.nih.gov/books/NBK305897/. Accessed 15 Apr 2024. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

