Rest-Activity Rhythm Differences in Acute Rehabilitation Between Poststroke Patients and Non-Brain Disease Controls: Comparative Study
- PMID: 38963936
- PMCID: PMC11258522
- DOI: 10.2196/49530
Rest-Activity Rhythm Differences in Acute Rehabilitation Between Poststroke Patients and Non-Brain Disease Controls: Comparative Study
Abstract
Background: Circadian rhythm disruptions are a common concern for poststroke patients undergoing rehabilitation and might negatively impact their functional outcomes.
Objective: Our research aimed to uncover unique patterns and disruptions specific to poststroke rehabilitation patients and identify potential differences in specific rest-activity rhythm indicators when compared to inpatient controls with non-brain-related lesions, such as patients with spinal cord injuries.
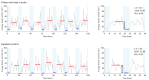
Methods: We obtained a 7-day recording with a wearable actigraphy device from 25 poststroke patients (n=9, 36% women; median age 56, IQR 46-71) and 25 age- and gender-matched inpatient control participants (n=15, 60% women; median age 57, IQR 46.5-68.5). To assess circadian rhythm, we used a nonparametric method to calculate key rest-activity rhythm indicators-relative amplitude, interdaily stability, and intradaily variability. Relative amplitude, quantifying rest-activity rhythm amplitude while considering daily variations and unbalanced amplitudes, was calculated as the ratio of the difference between the most active 10 continuous hours and the least active 5 continuous hours to the sum of these 10 and 5 continuous hours. We also examined the clinical correlations between rest-activity rhythm indicators and delirium screening tools, such as the 4 A's Test and the Barthel Index, which assess delirium and activities of daily living.
Results: Patients who had a stroke had higher least active 5-hour values compared to the control group (median 4.29, IQR 2.88-6.49 vs median 1.84, IQR 0.67-4.34; P=.008). The most active 10-hour values showed no significant differences between the groups (stroke group: median 38.92, IQR 14.60-40.87; control group: median 31.18, IQR 18.02-46.84; P=.93). The stroke group presented a lower relative amplitude compared to the control group (median 0.74, IQR 0.57-0.85 vs median 0.88, IQR 0.71-0.96; P=.009). Further analysis revealed no significant differences in other rest-activity rhythm metrics between the two groups. Among the patients who had a stroke, a negative correlation was observed between the 4 A's Test scores and relative amplitude (ρ=-0.41; P=.045). Across all participants, positive correlations emerged between the Barthel Index scores and both interdaily stability (ρ=0.34; P=.02) and the most active 10-hour value (ρ=0.42; P=.002).
Conclusions: This study highlights the relevance of circadian rhythm disruptions in poststroke rehabilitation and provides insights into potential diagnostic and prognostic implications for rest-activity rhythm indicators as digital biomarkers.
Keywords: circadian rhythms; stroke rehabilitation, rest-activity rhythms, relative amplitude, delirium screening, interdaily stability.
©Huey-Wen Liang, Chueh-Hung Wu, Chen Lin, Hsiang-Chih Chang, Yu-Hsuan Lin, Shao-Yu Chen, Wei-Chen Hsu. Originally published in the Journal of Medical Internet Research (https://www.jmir.org), 04.07.2024.
Conflict of interest statement
Conflicts of Interest: YHL is an associate editor of JMIR at the time of this publication
Figures

Similar articles
-
Associations of Rest-Activity Rhythm Disturbances With Stroke Risk and Poststroke Adverse Outcomes.J Am Heart Assoc. 2024 Sep 17;13(18):e032086. doi: 10.1161/JAHA.123.032086. Epub 2024 Sep 5. J Am Heart Assoc. 2024. PMID: 39234806 Free PMC article.
-
Circadian disturbances in Alzheimer's disease progression: a prospective observational cohort study of community-based older adults.Lancet Healthy Longev. 2020 Dec;1(3):e96-e105. doi: 10.1016/s2666-7568(20)30015-5. Epub 2020 Nov 12. Lancet Healthy Longev. 2020. PMID: 34179863 Free PMC article.
-
Comparing Human-Smartphone Interactions and Actigraphy Measurements for Circadian Rhythm Stability and Adiposity: Algorithm Development and Validation Study.J Med Internet Res. 2024 Jun 5;26:e50149. doi: 10.2196/50149. J Med Internet Res. 2024. PMID: 38838328 Free PMC article.
-
Non-pharmacological interventions for sleep promotion in hospitalized children.Cochrane Database Syst Rev. 2022 Jun 15;6(6):CD012908. doi: 10.1002/14651858.CD012908.pub2. Cochrane Database Syst Rev. 2022. PMID: 35703367 Free PMC article.
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2021 Apr 19;4(4):CD011535. doi: 10.1002/14651858.CD011535.pub4. Cochrane Database Syst Rev. 2021. Update in: Cochrane Database Syst Rev. 2022 May 23;5:CD011535. doi: 10.1002/14651858.CD011535.pub5. PMID: 33871055 Free PMC article. Updated.
References
-
- Sterr A, Kuhn M, Nissen C, Ettine D, Funk S, Feige B, Umarova R, Urbach H, Weiller C, Riemann D. Post-stroke insomnia in community-dwelling patients with chronic motor stroke: physiological evidence and implications for stroke care. Sci Rep. 2018 May 30;8(1):8409. doi: 10.1038/s41598-018-26630-y. https://boris.unibe.ch/id/eprint/125042 10.1038/s41598-018-26630-y - DOI - PMC - PubMed
-
- Duss SB, Seiler A, Schmidt MH, Pace M, Adamantidis A, Müri René M, Bassetti CL. The role of sleep in recovery following ischemic stroke: A review of human and animal data. Neurobiol Sleep Circadian Rhythms. 2017 Jan;2:94–105. doi: 10.1016/j.nbscr.2016.11.003. https://boris.unibe.ch/id/eprint/145198 S2451-9944(16)30014-1 - DOI - PMC - PubMed
-
- Siengsukon C, Al-Dughmi M, Al-Sharman A, Stevens S. Sleep parameters, functional status, and time post-stroke are associated with offline motor skill learning in people with chronic stroke. Front Neurol. 2015 Oct 30;6:225. doi: 10.3389/fneur.2015.00225. https://europepmc.org/abstract/MED/26579068 - DOI - PMC - PubMed
-
- Kim J, Kim Y, Yang KI, Kim D, Kim SA. The relationship between sleep disturbance and functional status in mild stroke patients. Ann Rehabil Med. 2015 Aug;39(4):545–52. doi: 10.5535/arm.2015.39.4.545. https://europepmc.org/abstract/MED/26361590 - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

