Virtual simulation training for postpartum hemorrhage in low-to-moderate-volume hospitals in the US
- PMID: 38975047
- PMCID: PMC11227018
- DOI: 10.1016/j.xagr.2024.100357
Virtual simulation training for postpartum hemorrhage in low-to-moderate-volume hospitals in the US
Abstract
Background: Maternal mortality in the United States is rising and many deaths are preventable. Emergencies, such as postpartum hemorrhage, occur less frequently in non-teaching, rural, and urban low-birth volume hospitals. There is an urgent need for accessible, evidence-based, and sustainable inter-professional education that creates the opportunity for clinical teams to practice their response to rare, but potentially devastating events.
Objective: To assess the feasibility of virtual simulation training for the management of postpartum hemorrhage in low-to-moderate-volume delivery hospitals.
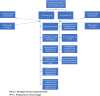
Study design: The study occurred between December 2021 and March 2022 within 8 non-academic hospitals in the United States with low-to-moderate-delivery volumes, randomized to one of two models: direct simulation training and train-the-trainer. In the direct simulation training model, simulation faculty conducted a virtual simulation training program with participants. In the train-the-trainer model, simulation faculty conducted virtual lessons with new simulation instructors on how to prepare and conduct a simulation course. Following this training, the instructors led their own simulation training program at their respective hospitals. The direct simulation training participants and students trained by new instructors from the train-the-trainer program were evaluated with a multiple-choice questionnaire on postpartum hemorrhage knowledge and a confidence and attitude survey at 3 timepoints: prior to, immediately after, and at 3 months post-training. Paired t-tests were performed to assess for changes in knowledge and confidence within teaching models across time points. ANOVA was performed to test cross-sectionally for differences in knowledge and confidence between teaching models at each time point.
Results: Direct simulation training participants (n=22) and students of the train-the-trainer instructors (n=18) included nurses, certified nurse midwives and attending physicians in obstetrics, family practice or anesthesiology. Mean pre-course knowledge and confidence scores were not statistically different between direct simulation participants and the students of the instructors from the train-the-trainer course (79%+/-13 versus 75%+/-14, respectively, P-value=.45). Within the direct simulation group, knowledge and confidence scores significantly improved from pre- to immediately post-training (knowledge score mean difference 9.81 [95% CI 3.23-16.40], P-value<.01; confidence score mean difference 13.64 [95% CI 6.79-20.48], P-value<.01), which were maintained 3-months post-training. Within the train-the-trainer group, knowledge and confidence scores immediate post-intervention were not significantly different compared with pre-course or 3-month post-course scores. Mean knowledge scores were significantly greater for the direct simulation group compared to the train-the-trainer group immediately post-training (89%+/-7 versus 74%+/-8, P-value<.01) and at 3-months (88%+/-7 versus 76%+/-12, P-value<.01). Comparisons between groups showed no difference in confidence and attitude scores at these timepoints. Both direct simulation participants and train-the-trainer instructors preferred virtual education, or a hybrid structure, over in-person education.
Conclusion: Virtual education for obstetric simulation training is feasible, acceptable, and effective. Utilizing a direct simulation model for postpartum hemorrhage management resulted in enhanced knowledge acquisition and retention compared to a train-the-trainer model.
Keywords: education; emergency; innovation; low-volume; moderate-volume; multidisciplinary; non-academic; postpartum hemorrhage; rural; technology; train-the-trainer.
© 2024 The Authors.
Conflict of interest statement
The authors have no conflicts of interest.
Figures
References
-
- Provisional Maternal Death Counts. National Center for Health Statistics. 2023. Accessed Nov. 22, 2023. Available at:https://www.cdc.gov/nchs/nvss/vsrr/provisional-maternal-deaths.htm
-
- Alkema L, Chou D, Hogan D, et al. Global, regional, and national levels and trends in maternal mortality between 1990 and 2015, with scenario-based projections to 2030: a systematic analysis by the UN Maternal Mortality Estimation Inter-Agency Group. Lancet. 2016;387(10017):462–474. doi: 10.1016/S0140-6736(15)00838-7. - DOI - PMC - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources