Decoding immune-related gene-signatures in colorectal neoplasia
- PMID: 38979413
- PMCID: PMC11229009
- DOI: 10.3389/fimmu.2024.1407995
Decoding immune-related gene-signatures in colorectal neoplasia
Abstract
Background: Colorectal cancer (CRC) is a significant health issue, with notable incidence rates in Norway. The immune response plays a dual role in CRC, offering both protective effects and promoting tumor growth. This research aims to provide a detailed screening of immune-related genes and identify specific genes in CRC and adenomatous polyps within the Norwegian population, potentially serving as detection biomarkers.
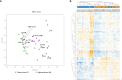
Methods: The study involved 69 patients (228 biopsies) undergoing colonoscopy, divided into CRC, adenomatous polyps, and control groups. We examined the expression of 579 immune genes through nCounter analysis emphasizing differential expression in tumor versus adjacent non-tumorous tissue and performed quantitative reverse transcription polymerase chain reaction (RT-qPCR) across patient categories.
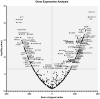
Results: Key findings include the elevated expression of CXCL1, CXCL2, IL1B, IL6, CXCL8 (IL8), PTGS2, and SPP1 in CRC tissues. Additionally, CXCL1, CXCL2, IL6, CXCL8, and PTGS2 showed significant expression changes in adenomatous polyps, suggesting their early involvement in carcinogenesis.
Conclusions: This study uncovers a distinctive immunological signature in colorectal neoplasia among Norwegians, highlighting CXCL1, CXCL2, IL1B, IL6, CXCL8, PTGS2, and SPP1 as potential CRC biomarkers. These findings warrant further research to confirm their role and explore their utility in non-invasive screening strategies.
Keywords: Norway; adenomatous polyps; biomarker potential; colorectal cancer (CRC); gene expression; immunology.
Copyright © 2024 Omran, Tunsjø, Jahanlu, Brackmann, Bemanian and Sæther.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures



Similar articles
-
Selection of optimal extraction and RT-PCR protocols for stool RNA detection of colorectal cancer associated immune genes.Sci Rep. 2024 Nov 10;14(1):27468. doi: 10.1038/s41598-024-78680-0. Sci Rep. 2024. PMID: 39523395 Free PMC article.
-
A novel gene expression signature in peripheral blood mononuclear cells for early detection of colorectal cancer.Aliment Pharmacol Ther. 2014 Mar;39(5):507-17. doi: 10.1111/apt.12618. Epub 2014 Jan 16. Aliment Pharmacol Ther. 2014. PMID: 24428642
-
LINE-1 is preferentially hypomethylated within adenomatous polyps in the presence of synchronous colorectal cancer.Clin Epigenetics. 2017 Mar 9;9:25. doi: 10.1186/s13148-017-0325-7. eCollection 2017. Clin Epigenetics. 2017. PMID: 28293326 Free PMC article.
-
Transcriptomic Signatures in Colorectal Cancer Progression.Curr Mol Med. 2023;23(3):239-249. doi: 10.2174/1566524022666220427102048. Curr Mol Med. 2023. PMID: 35490318 Review.
-
Contribution of bi-allelic germline MUTYH mutations to early-onset and familial colorectal cancer and to low number of adenomatous polyps: case-series and literature review.Fam Cancer. 2013 Mar;12(1):43-50. doi: 10.1007/s10689-012-9570-2. Fam Cancer. 2013. PMID: 23007840 Review.
Cited by
-
The Immune Environment in Colorectal Adenoma: A Systematic Review.Biomedicines. 2025 Mar 12;13(3):699. doi: 10.3390/biomedicines13030699. Biomedicines. 2025. PMID: 40149674 Free PMC article. Review.
-
CXCL2: a key player in the tumor microenvironment and inflammatory diseases.Cancer Cell Int. 2025 Apr 7;25(1):133. doi: 10.1186/s12935-025-03765-3. Cancer Cell Int. 2025. PMID: 40197328 Free PMC article. Review.
-
Selection of optimal extraction and RT-PCR protocols for stool RNA detection of colorectal cancer associated immune genes.Sci Rep. 2024 Nov 10;14(1):27468. doi: 10.1038/s41598-024-78680-0. Sci Rep. 2024. PMID: 39523395 Free PMC article.
References
-
- Norway CRo . Cancer incidence, mortality, survival and prevalence in Norway. Oslo: Cancer in Norway; (2022).
-
- Xu W, He Y, Wang Y, Li X, Young J, Ioannidis JPA, et al. . Risk factors and risk prediction models for colorectal cancer metastasis and recurrence: an umbrella review of systematic reviews and meta-analyses of observational studies. BMC Med. (2020) 18:172. doi: 10.1186/s12916-020-01618-6 - DOI - PMC - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

