Lower urinary tract dysfunction in the central nervous system neurogenic bladder and the real-life treatment outcome of botulinum toxin A
- PMID: 38993829
- PMCID: PMC11236072
- DOI: 10.4103/tcmj.tcmj_29_24
Lower urinary tract dysfunction in the central nervous system neurogenic bladder and the real-life treatment outcome of botulinum toxin A
Abstract
Neurogenic lower urinary tract dysfunction (NLUTD) is common in patients with central nervous system (CNS) lesions. Cases of cerebrovascular accidents (CVA), Parkinson's disease, dementia, and other intracranial lesions develop poor bladder control with or without urinary difficulty due to loss of cortical perception of bladder filling sensation and poor coordination of urethral sphincter relaxation during reflex micturition. Patients with CNS lesions usually have overactive bladder (OAB) symptoms, including urgency, frequency, incontinence, voiding symptoms of dysuria, large postvoid residual volume, and retention. In elderly patients with severe CNS disease the OAB symptoms are usually difficult to adequately relieve by medical treatment, and thus, their quality of life is greatly. Botulinum toxin A (BoNT-A) is currently licensed and has been applied in patients with idiopathic and neurogenic OAB due to spinal cord injury or multiple sclerosis. However, the application of BoNT-A in the treatment of urinary incontinence due to NLUTD in chronic CNS lesions has not been well-documented. Although cohort studies and case series support BoNT-A treatment for neurogenic OAB, chronic urine retention after intravesical BoNT-A injection for OAB and exacerbated urinary incontinence after urethral BoNT-A injection for voiding dysfunction have greatly limited its application among patients with NLUTD due to CNS lesions. This article reviews the pathophysiology and clinical characteristics of NLUTD in patients with CNS lesions and the clinical effects and adverse events of BoNT-A injection for patients with NLUTD. A flowchart was created to outline the patient selection and treatment strategy for neurogenic OAB.
Keywords: Botulinum toxin A; Dysfunctional voiding; Lower urinary tract dysfunction; Neurogenic bladder; Overactive bladder.
Copyright: © 2024 Tzu Chi Medical Journal.
Conflict of interest statement
Dr. Hann-Chorng Kuo, an editorial board member at Tzu Chi Medical Journal, had no role in the peer review process or the decision to publish this article.
Figures
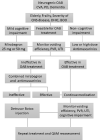
References
-
- Griffiths D, Derbyshire S, Stenger A, Resnick N. Brain control of normal and overactive bladder. J Urol. 2005;174:1862–7. - PubMed
-
- Tudor KI, Sakakibara R, Panicker JN. Neurogenic lower urinary tract dysfunction: Evaluation and management. J Neurol. 2016;263:2555–64. - PubMed
-
- Chang TL, Chen SF, Kuo HC. Surgical outcome of male patients with chronic central nervous system disorders and voiding dysfunction due to bladder outlet obstruction. Int Urol Nephrol. 2022;54:2511–9. - PubMed
-
- Malone-Lee J, Wahedna I. Characterisation of detrusor contractile function in relation to old age. Br J Urol. 1993;72:873–80. - PubMed
-
- Resnick NM, Yalla SV. Detrusor hyperactivity with impaired contractile function. An unrecognized but common cause of incontinence in elderly patients. JAMA. 1987;257:3076–81. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
