The profile of patients with postpartum hemorrhage admitted to the obstetric intensive care: a cross-sectional study
- PMID: 38994461
- PMCID: PMC11239208
- DOI: 10.61622/rbgo/2024rbgo47
The profile of patients with postpartum hemorrhage admitted to the obstetric intensive care: a cross-sectional study
Abstract
Objective: In Brazil, postpartum hemorrhage (PPH) is a major cause of maternal morbidity and mortality. Data on the profile of women and risk factors associated with PPH are sparse. This study aimed to describe the profile and management of patients with PPH, and the association of risk factors for PPH with severe maternal outcomes (SMO).
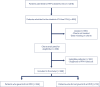
Methods: A cross-sectional study was conducted in Instituto de Medicina Integral Prof. Fernando Figueira (IMIP) obstetric intensive care unit (ICU) between January 2012 and March 2020, including patients who gave birth at the hospital and that were admitted with PPH to the ICU.
Results: The study included 358 patients, of whom 245 (68.4%) delivered in the IMIP maternity, and 113 (31.6%) in other maternity. The mean age of the patients was 26.7 years, with up to eight years of education (46.1%) and a mean of six prenatal care. Uterine atony (72.9%) was the most common cause, 1.6% estimated blood loss, 2% calculated shock index (SI), 63.9% of patients received hemotransfusion, and 27% underwent hysterectomy. 136 cases of SMO were identified, 35.5% were classified as maternal near miss and 3.0% maternal deaths. Multiparity was associated with SMO as an antepartum risk factor (RR=1.83, 95% CI1.42-2.36). Regarding intrapartum risk factors, abruptio placentae abruption was associated with SMO (RR=2.2 95% CI1.75-2.81). Among those who had hypertension (49.6%) there was a lower risk of developing SMO.
Conclusion: The principal factors associated with poor maternal outcome were being multiparous and placental abruption.
Keywords: Intensive care units; Maternal mortality; Postpartum hemorrhage; Pregnancy.
Conflict of interest statement
Conflicts to interest: none to declare.
References
-
- World Health Organization . WHO recommendations on the assessment of postpartum blood loss and use of a treatment bundles for postpartum haemorrhage. Geneva: WHO; 2023. - PubMed
-
- Ministério da Saúde. Secretaria de Vigilância em Saúde Maternal mortality in Brazil. Bol Epidemiol. 51(20):21–27. Portuguese.
-
- Freitas RA., Júnior Avoidable maternal mortality as social injustice. Rev Bras Saúde Matern Infant. 2020;20(2):607–614. doi: 10.1590/1806-93042020000200016. - DOI
MeSH terms
LinkOut - more resources
Full Text Sources
Miscellaneous