Predictive value of MRI-based deep learning model for lymphovascular invasion status in node-negative invasive breast cancer
- PMID: 39003325
- PMCID: PMC11246470
- DOI: 10.1038/s41598-024-67217-0
Predictive value of MRI-based deep learning model for lymphovascular invasion status in node-negative invasive breast cancer
Abstract
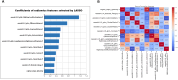
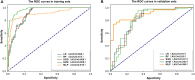
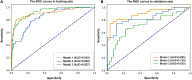
To retrospectively assess the effectiveness of deep learning (DL) model, based on breast magnetic resonance imaging (MRI), in predicting preoperative lymphovascular invasion (LVI) status in patients diagnosed with invasive breast cancer who have negative axillary lymph nodes (LNs). Data was gathered from 280 patients, including 148 with LVI-positive and 141 with LVI-negative lesions. These patients had undergone preoperative breast MRI and were histopathologically confirmed to have invasive breast cancer without axillary LN metastasis. The cohort was randomly split into training and validation groups in a 7:3 ratio. Radiomics features for each lesion were extracted from the first post-contrast dynamic contrast-enhanced (DCE)-MRI. The Least Absolute Shrinkage and Selection Operator (LASSO) regression method and logistic regression analyses were employed to identify significant radiomic features and clinicoradiological variables. These models were established using four machine learning (ML) algorithms and one DL algorithm. The predictive performance of the models (radiomics, clinicoradiological, and combination) was assessed through discrimination and compared using the DeLong test. Four clinicoradiological parameters and 10 radiomic features were selected by LASSO for model development. The Multilayer Perceptron (MLP) model, constructed using both radiomic and clinicoradiological features, demonstrated excellent performance in predicting LVI, achieving a high area under the curve (AUC) of 0.835 for validation. The DL model (MLP-radiomic) achieved the highest accuracy (AUC = 0.896), followed by DL model (MLP-combination) with an AUC of 0.835. Both DL models were significantly superior to the ML model (RF-clinical) with an AUC of 0.720. The DL model (MLP), which integrates radiomic features with clinicoradiological information, effectively aids in the preoperative determination of LVI status in patients with invasive breast cancer and negative axillary LNs. This is beneficial for making informed clinical decisions.
Keywords: Breast cancer; Deep learning; Lymphovascular invasion; Magnetic resonance imaging.
© 2024. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures



Similar articles
-
Preoperative prediction of lymphovascular invasion in invasive breast cancer with dynamic contrast-enhanced-MRI-based radiomics.J Magn Reson Imaging. 2019 Sep;50(3):847-857. doi: 10.1002/jmri.26688. Epub 2019 Feb 17. J Magn Reson Imaging. 2019. PMID: 30773770
-
Assessment of Lymphovascular Invasion in Breast Cancer Using a Combined MRI Morphological Features, Radiomics, and Deep Learning Approach Based on Dynamic Contrast-Enhanced MRI.J Magn Reson Imaging. 2024 Jun;59(6):2238-2249. doi: 10.1002/jmri.29060. Epub 2023 Oct 19. J Magn Reson Imaging. 2024. PMID: 37855421
-
Multiphases DCE-MRI Radiomics Nomogram for Preoperative Prediction of Lymphovascular Invasion in Invasive Breast Cancer.Acad Radiol. 2024 Dec;31(12):4743-4758. doi: 10.1016/j.acra.2024.06.007. Epub 2024 Aug 5. Acad Radiol. 2024. PMID: 39107190
-
Deep learning-based breast MRI for predicting axillary lymph node metastasis: a systematic review and meta-analysis.Cancer Imaging. 2025 Mar 31;25(1):44. doi: 10.1186/s40644-025-00863-3. Cancer Imaging. 2025. PMID: 40165212 Free PMC article.
-
The use of radiomics in magnetic resonance imaging for the pre-treatment characterisation of breast cancers: A scoping review.J Med Radiat Sci. 2023 Dec;70(4):462-478. doi: 10.1002/jmrs.709. Epub 2023 Aug 3. J Med Radiat Sci. 2023. PMID: 37534540 Free PMC article.
References
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

