Childhood Opportunity and Acute Interstage Outcomes: A National Pediatric Cardiology Quality Improvement Collaborative Analysis
- PMID: 39008557
- PMCID: PMC11251506
- DOI: 10.1161/CIRCULATIONAHA.124.069127
Childhood Opportunity and Acute Interstage Outcomes: A National Pediatric Cardiology Quality Improvement Collaborative Analysis
Abstract
Background: The interstage period after discharge from stage 1 palliation carries high morbidity and mortality. The impact of social determinants of health on interstage outcomes is not well characterized. We assessed the relationship between childhood opportunity and acute interstage outcomes.
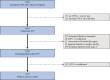
Methods: Infants discharged home after stage 1 palliation in the National Pediatric Quality Improvement Collaborative Phase II registry (2016-2022) were retrospectively reviewed. Zip code-level Childhood Opportunity Index (COI), a composite metric of 29 indicators across education, health and environment, and socioeconomic domains, was used to classify patients into 5 COI levels. Acute interstage outcomes included death or transplant listing, unplanned readmission, intensive care unit admission, unplanned catheterization, and reoperation. The association between COI level and acute interstage outcomes was assessed using logistic regression with sequential adjustment for potential confounders.
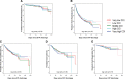
Results: The analysis cohort included 1837 patients from 69 centers. Birth weight (P<0.001) and proximity to a surgical center at birth (P=0.02) increased with COI level. Stage 1 length of stay decreased (P=0.001), and exclusive oral feeding rate at discharge increased (P<0.001), with higher COI level. More than 98% of patients in all COI levels were enrolled in home monitoring. Death or transplant listing occurred in 101 (5%) patients with unplanned readmission in 987 (53%), intensive care unit admission in 448 (24%), catheterization in 345 (19%), and reoperation in 83 (5%). There was no difference in the incidence or time to occurrence of any acute interstage outcome among COI levels in unadjusted or adjusted analysis. There was no interaction between race and ethnicity and childhood opportunity in acute interstage outcomes.
Conclusions: Zip code COI level is associated with differences in preoperative risk factors and stage 1 palliation hospitalization characteristics. Acute interstage outcomes, although common across the spectrum of childhood opportunity, are not associated with COI level in an era of highly prevalent home monitoring programs. The role of home monitoring in mitigating disparities during the interstage period merits further investigation.
Keywords: childhood opportunity; hypoplastic left heart syndrome; single ventricle; social disparities; socioeconomic status.
Conflict of interest statement
None.
Figures
Similar articles
-
Variability of antithrombotics use in patients with hypoplastic left heart syndrome and its variants following first- and second-stage palliation surgery: a national report using the National Pediatric Cardiology Quality Improvement Collaborative registry.Cardiol Young. 2017 May;27(4):731-738. doi: 10.1017/S1047951116001189. Epub 2016 Aug 30. Cardiol Young. 2017. PMID: 27981915
-
Risk Factors for Unanticipated Readmissions During the Interstage: A Report From the National Pediatric Cardiology Quality Improvement Collaborative.Semin Thorac Cardiovasc Surg. 2016 Winter;28(4):803-814. doi: 10.1053/j.semtcvs.2016.08.011. Epub 2016 Sep 5. Semin Thorac Cardiovasc Surg. 2016. PMID: 28417868
-
Predictors of Prolonged Hospital Length of Stay Following Stage II Palliation of Hypoplastic Left Heart Syndrome (and Variants): Analysis of the National Pediatric Cardiology Quality Improvement Collaborative (NPC-QIC) Database.Pediatr Cardiol. 2015 Dec;36(8):1630-41. doi: 10.1007/s00246-015-1208-3. Epub 2015 Jun 3. Pediatr Cardiol. 2015. PMID: 26036350
-
Parental mobile health adherence to symptom home monitoring for infants with congenital heart disease during the single ventricle interstage period: A concept analysis.J Spec Pediatr Nurs. 2020 Oct;25(4):e12303. doi: 10.1111/jspn.12303. Epub 2020 Jul 14. J Spec Pediatr Nurs. 2020. PMID: 32662243 Review.
-
Postoperative Morbidity and Interstage Hemodynamics Following Stage I Palliation in Patients with Turner Syndrome and Hypoplastic Left Heart Syndrome.Pediatr Cardiol. 2024 Feb;45(2):221-227. doi: 10.1007/s00246-023-03395-4. Epub 2023 Dec 28. Pediatr Cardiol. 2024. PMID: 38153546 Review.
Cited by
-
Unplanned Readmissions in Pediatric Cardiac Disease: Impacts of Social Determinants of Health.Pediatr Cardiol. 2025 May 17. doi: 10.1007/s00246-025-03883-9. Online ahead of print. Pediatr Cardiol. 2025. PMID: 40381042
-
Hypoplastic left heart syndrome-a scoping review.Transl Pediatr. 2025 Apr 30;14(4):700-717. doi: 10.21037/tp-24-367. Epub 2025 Apr 27. Transl Pediatr. 2025. PMID: 40386366 Free PMC article. Review.
References
-
- Ghanayem NS, Allen KR, Tabbutt S, Atz AM, Clabby ML, Cooper DS, Eghtesady P, Frommelt PC, Gruber PJ, Hill KD, et al. ; Pediatric Heart Network Investigators. Interstage mortality after the Norwood procedure: results of the multicenter Single Ventricle Reconstruction trial. J Thorac Cardiovasc Surg. 2012;144:896–906. doi: 10.1016/j.jtcvs.2012.05.020 - PMC - PubMed
-
- Rudd NA, Ghanayem NS, Hill GD, Lambert LM, Mussatto KA, Nieves JA, Robinson S, Shirali G, Steltzer MM, Uzark K, et al. ; American Heart Association Council on Cardiovascular and Stroke Nursing; Council on Lifelong Congenital Heart Disease and Heart Health in the Young; Council on Arteriosclerosis, Thrombosis and Vascular Biology; Council on Clinical Cardiology; and Council on Lifestyle and Cardiometabolic HealthCardiometabolic H. Interstage home monitoring for infants with single ventricle heart disease: education and management: a scientific statement from the American Heart Association. J Am Heart Assoc. 2020;9:e014548. doi: 10.1161/JAHA.119.014548 - PMC - PubMed
-
- Liu MY, Zielonka B, Snarr BS, Zhang X, Gaynor JW, Rychik J. Longitudinal assessment of outcome from prenatal diagnosis through Fontan operation for over 500 fetuses with single ventricle-type congenital heart disease: the Philadelphia Fetus-to-Fontan Cohort Study. J Am Heart Assoc. 2018;7:e009145. doi: 10.1161/JAHA.118.009145 - PMC - PubMed
-
- Brown DW, Mangeot C, Anderson JB, Peterson LE, King EC, Lihn SL, Neish SR, Fleishman C, Phelps C, Hanke S, et al. ; National Pediatric Cardiology Quality Improvement Collaborative. Digoxin use is associated with reduced interstage mortality in patients with no history of arrhythmia after stage I palliation for single ventricle heart disease. J Am Heart Assoc. 2016;5:e002376. doi: 10.1161/JAHA.115.002376 - PMC - PubMed
-
- Hornik CP, He X, Jacobs JP, Li JS, Jaquiss RD, Jacobs ML, O’Brien SM, Peterson ED, Pasquali SK. Complications after the Norwood operation: an analysis of the Society of Thoracic Surgeons Congenital Heart Surgery Database. Ann Thorac Surg. 2011;92:1734–1740. doi: 10.1016/j.athoracsur.2011.05.100 - PMC - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

