A paradigm shift in diagnosis and treatment innovation for mucinous cystic neoplasms of the liver
- PMID: 39019969
- PMCID: PMC11255220
- DOI: 10.1038/s41598-024-67320-2
A paradigm shift in diagnosis and treatment innovation for mucinous cystic neoplasms of the liver
Abstract
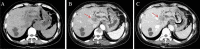
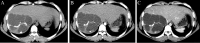
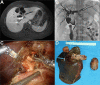
This study comprehensively explores the clinical characteristics, diagnostic approaches, and treatment methods for liver mucinous cystic neoplasms (MCN). A retrospective analysis was conducted on seven individuals diagnosed with MCN, admitted to the Fifth Medical Center of the PLA General Hospital between October 2016 and May 2023. Preoperative AFP was negative, while CA19-9 was elevated in two cases. Surgical resection was performed for all patients. The patients showed favorable postoperative recovery. Follow-up revealed an excellent overall survival rate, except for one case of invasive carcinoma resulting in tumor recurrence and metastasis 6 months after surgery. MCN poses a diagnostic challenge due to the absence of distinct clinical and radiological features, leading to potential misdiagnosis and inappropriate treatment. Patients with suspected liver cystic diseases should consider the possibility of MCN. Surgical resection has proven to be a practical approach with satisfactory therapeutic outcomes.
Keywords: Diagnosis; Invasive carcinoma; Liver; Mucinous cystic neoplasms; Surgical resection; Treatment.
© 2024. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures

References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

