A Study of Predictors of Failure of Nonoperative Management of Ileocolic Intussusception in Children
- PMID: 39022205
- PMCID: PMC11249906
- DOI: 10.5005/jp-journals-10018-1432
A Study of Predictors of Failure of Nonoperative Management of Ileocolic Intussusception in Children
Abstract
Background: Surgery remains the mainstay in treating intussusception in developing nations. A correspondingly high bowel resection rate exists despite a shift to nonoperative reduction in high-income countries. We aimed to study the clinical profile of the patients with intussusception presenting to our hospital and to assess the clinical and radiological predictors of success or failure of nonoperative management of intussusception.
Materials and methods: This prospective study was conducted in the Department of Pediatric Surgery over a period of 3 years and included a total of 118 patients who presenting to our emergency division with features suggestive of intussusception and were managed accordingly either with hydrostatic reduction or by surgical intervention.
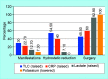
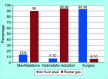
Results: We observed that the majority of the patients were males (65.5%). The mean age was 13.54 months. Intermittent pain was the most common symptom. Both pain and vomiting did not affect the outcome. Lab parameters like raised total leukocyte counts (TLC), C-reactive protein (CRP) and lactate levels were significantly associated with failure of hydrostatic reduction. Patients with air fluid levels on X-ray were more likely to end up in surgery. Ultrasound findings of bowel wall edema, aperistaltic gut loops and a pathological lead point was associated with failure of hydrostatic reduction as well. The overall success rate of hydrostatic reduction was 85.5%.
Conclusion: Hydrostatic reduction of intussusception is a safe and effective method of management of intussusception whenever indicated. Factors that might reduce the chance of its success include continuous pain, irritability, tenderness, deranged lab parameters like TLC, CRP and lactate levels, air fluid levels on X-ray, bowel wall edema, aperistalsis and the presence of a lead point.
How to cite this article: Shah JY, Banday I, Hamdani HZ, et al. A Study of Predictors of Failure of Nonoperative Management of Ileocolic Intussusception in Children. Euroasian J Hepato-Gastroenterol 2024;14(1):81-85.
Keywords: Acute abdomen; Hydrostatic reduction; Intussusception; Outcomes; Pediatric emergency; Pediatric surgery.
Copyright © 2024; The Author(s).
Conflict of interest statement
Source of support: Nil Conflict of interest: None
Figures

References
-
- Jain S, Haydel MJ. Treasure Island (FL): StatPearls Publishing; 2022. Child Intussusception. In: StatPearls [Internet]. Available at: https://www.ncbi.nlm.nih.gov/books/NBK431078. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous
