White Matter Hyperintensities Are Associated with Slower Gait Speed in Older Adults without Dementia
- PMID: 39025052
- PMCID: PMC11747921
- DOI: 10.1159/000538944
White Matter Hyperintensities Are Associated with Slower Gait Speed in Older Adults without Dementia
Abstract
Introduction: Slow gait speed is associated with poor health outcomes in aging, but the relationship between cerebral small vessel disease (CSVD) pathologies and gait speed in aging is not well understood. We investigated the relationships between CSVD imaging markers and gait speed during simple (normal pace walking [NPW]) and complex (walking while talking [WWT]) as both measures are associated with shared health outcomes such as falls, frailty, disability, mortality, and dementia.
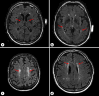
Methods: A total of 113 Ashkenazi Jewish adults over 65 (M age = 78.6 ± 6.3 years, 45.8% women) and without dementia were examined. Established rating systems were used to quantify white matter hyperintensities (WMHs) and lacunes of presumed vascular origin from fluid-attenuated inversion recovery (FLAIR) images. Linear regression models adjusted for age, sex, global health, and total intracranial volume were used to examine associations between CSVD markers and gait speed during NPW and WWT. Student t tests were used to contrast gait speed in those with "confluent-diffuse" WMH and those with "mild or no" WMH.
Results: The number of WMH in the basal ganglia (β = -3.274 cm/s p = 0.047) and temporal lobes (β = -3.113 cm/s p = 0.048) were associated with slower NPW speed in adjusted models. Participants with higher CSVD burden (confluent-diffuse pattern) in the frontal lobe (94.65 cm/s vs. 105.21 cm/s, p = 0.018) and globally (98.98 cm/s vs. 107.24 cm/s, p = 0.028) also had lower NPW speed. WMHs were not associated with WWT speeds. Lacunes were not associated with NPW or WWT speed.
Conclusion: Adjusted models found higher CSVD burden as measured by the presence of WMH in the basal ganglia and temporal lobes were associated with slower normal pace gait speed in older adults, but not with complex walking speeds. Participants with confluent-diffuse WMHs in the frontal lobes were found to have slower average normal gait speed. Further studies are needed to establish the temporality of WMH and gait speed decline as well as mechanistic links between the two.
Introduction: Slow gait speed is associated with poor health outcomes in aging, but the relationship between cerebral small vessel disease (CSVD) pathologies and gait speed in aging is not well understood. We investigated the relationships between CSVD imaging markers and gait speed during simple (normal pace walking [NPW]) and complex (walking while talking [WWT]) as both measures are associated with shared health outcomes such as falls, frailty, disability, mortality, and dementia.
Methods: A total of 113 Ashkenazi Jewish adults over 65 (M age = 78.6 ± 6.3 years, 45.8% women) and without dementia were examined. Established rating systems were used to quantify white matter hyperintensities (WMHs) and lacunes of presumed vascular origin from fluid-attenuated inversion recovery (FLAIR) images. Linear regression models adjusted for age, sex, global health, and total intracranial volume were used to examine associations between CSVD markers and gait speed during NPW and WWT. Student t tests were used to contrast gait speed in those with "confluent-diffuse" WMH and those with "mild or no" WMH.
Results: The number of WMH in the basal ganglia (β = -3.274 cm/s p = 0.047) and temporal lobes (β = -3.113 cm/s p = 0.048) were associated with slower NPW speed in adjusted models. Participants with higher CSVD burden (confluent-diffuse pattern) in the frontal lobe (94.65 cm/s vs. 105.21 cm/s, p = 0.018) and globally (98.98 cm/s vs. 107.24 cm/s, p = 0.028) also had lower NPW speed. WMHs were not associated with WWT speeds. Lacunes were not associated with NPW or WWT speed.
Conclusion: Adjusted models found higher CSVD burden as measured by the presence of WMH in the basal ganglia and temporal lobes were associated with slower normal pace gait speed in older adults, but not with complex walking speeds. Participants with confluent-diffuse WMHs in the frontal lobes were found to have slower average normal gait speed. Further studies are needed to establish the temporality of WMH and gait speed decline as well as mechanistic links between the two.
Keywords: Aging; Cerebral small vessel disease; Gait speed; Neuroimaging.
© 2024 S. Karger AG, Basel.
Conflict of interest statement
The authors have no conflicts of interest to declare.
Figures
Similar articles
-
Cerebral small vessel disease, cardiovascular risk factors, and future walking speed in old age: a population-based cohort study.BMC Neurol. 2021 Dec 24;21(1):496. doi: 10.1186/s12883-021-02529-6. BMC Neurol. 2021. PMID: 34949170 Free PMC article.
-
Pathways linking regional hyperintensities in the brain and slower gait.Neuroimage. 2014 Oct 1;99:7-13. doi: 10.1016/j.neuroimage.2014.05.017. Epub 2014 May 17. Neuroimage. 2014. PMID: 24841418 Free PMC article.
-
Impact of enlarged perivascular spaces in the basal ganglia on gait in cerebral small vessel disease.Aging Clin Exp Res. 2025 Apr 30;37(1):138. doi: 10.1007/s40520-025-03045-0. Aging Clin Exp Res. 2025. PMID: 40304928 Free PMC article.
-
Gait and falls in cerebral small vessel disease: a systematic review and meta-analysis.Age Ageing. 2023 Mar 1;52(3):afad011. doi: 10.1093/ageing/afad011. Age Ageing. 2023. PMID: 37000039 Free PMC article.
-
White matter hyperintensities and risks of cognitive impairment and dementia: A systematic review and meta-analysis of 36 prospective studies.Neurosci Biobehav Rev. 2021 Jan;120:16-27. doi: 10.1016/j.neubiorev.2020.11.007. Epub 2020 Nov 11. Neurosci Biobehav Rev. 2021. PMID: 33188821
Cited by
-
Cognitive cerebellum dominates motor cerebellum in functional decline of older adults with mild cognitive impairment.PLoS One. 2025 Apr 3;20(4):e0321304. doi: 10.1371/journal.pone.0321304. eCollection 2025. PLoS One. 2025. PMID: 40179117 Free PMC article.
References
-
- Paulson S, Gray M. Parameters of gait among community-dwelling older adults. J Geriatr Phys Ther. 2015;38(1):28–32. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources