Validation of a commercially available CAD-system for lung nodule detection and characterization using CT-scans
- PMID: 39042303
- PMCID: PMC11782423
- DOI: 10.1007/s00330-024-10969-0
Validation of a commercially available CAD-system for lung nodule detection and characterization using CT-scans
Abstract
Objectives: This study aims to externally validate a commercially available Computer-Aided Detection (CAD)-system for the automatic detection and characterization of solid, part-solid, and ground-glass lung nodules (LN) on CT scans.
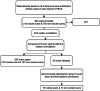
Methods: This retrospective study encompasses 263 chest CT scans performed between January 2020 and December 2021 at a Dutch university hospital. All scans were read by a radiologist (R1) and compared with the initial radiology report. Conflicting scans were assessed by an adjudicating radiologist (R2). All scans were also processed by CAD. The standalone performance of CAD in terms of sensitivity and false-positive (FP)-rate for detection was calculated together with the sensitivity for characterization, including texture, calcification, speculation, and location. The R1's detection sensitivity was also assessed.
Results: A total of 183 true nodules were identified in 121 nodule-containing scans (142 non-nodule-containing scans), of which R1 identified 165/183 (90.2%). CAD detected 149 nodules, of which 12 were not identified by R1, achieving a sensitivity of 149/183 (81.4%) with an FP-rate of 49/121 (0.405). CAD's detection sensitivity for solid, part-solid, and ground-glass LNs was 82/94 (87.2%), 42/47 (89.4%), and 25/42 (59.5%), respectively. The classification accuracy for solid, part-solid, and ground-glass LNs was 81/82 (98.8%), 16/42 (38.1%), and 18/25 (72.0%), respectively. Additionally, CAD demonstrated overall classification accuracies of 137/149 (91.9%), 123/149 (82.6%), and 141/149 (94.6%) for calcification, spiculation, and location, respectively.
Conclusions: Although the overall detection rate of this system slightly lags behind that of a radiologist, CAD is capable of detecting different LNs and thereby has the potential to enhance a reader's detection rate. While promising characterization performances are obtained, the tool's performance in terms of texture classification remains a subject of concern.
Clinical relevance statement: Numerous lung nodule computer-aided detection-systems are commercially available, with some of them solely being externally validated based on their detection performance on solid nodules. We encourage researchers to assess performances by incorporating all relevant characteristics, including part-solid and ground-glass nodules.
Key points: Few computer-aided detection (CAD) systems are externally validated for automatic detection and characterization of lung nodules. A detection sensitivity of 81.4% and an overall texture classification sensitivity of 77.2% were measured utilizing CAD. CAD has the potential to increase single reader detection rate, however, improvement in texture classification is required.
Keywords: Computer-assisted detection; Early detection of cancer; Lung; Lung cancer; Validation study.
© 2024. The Author(s).
Conflict of interest statement
Compliance with ethical standards. Guarantor: The scientific guarantor of this publication is Jacob J. Visser, MD, PhD. Conflict of interest: The authors of this manuscript declare relationships with the following companies: Souvik Mandal, Prakash Vanapalli, Vikash Challa, Saigopal Sathyamurthy, Ranjana Devi, and Ritvik Jain are full-time paid employees of Qure.ai. Jacob J. Visser, MD, PhD: Grant to institution from Qure.ai; consulting fees from Tegus; payment to institution for lectures from Roche; travel grant from Qure.ai; participation on a data safety monitoring board or advisory board from Quibim, Contextflow, Noaber Foundation, and NLC Ventures; leadership or fiduciary role on the steering committee of the PINPOINT Project (payment to institution from AstraZeneca) and RSNA Common Data Elements Steering Committee (unpaid); phantom shares in Contextflow and Quibim. The remaining authors declare no conflicts of interest. Statistics and biometry: Daniel Bos, MD, PhD and Saigopal Sathyamurthy kindly provided statistical advice for this manuscript. Informed consent: Written informed consent was waived by the Institutional Review Board because of the retrospective nature of the study and the analysis only used anonymous data. Ethical approval: The study protocol was reviewed and approved by the Medical Ethics Review Committee Erasmus Medical Centre Rotterdam (2022-0465). Study subjects or cohorts overlap: No overlaps. Methodology: Retrospective Diagnostic or prognostic study Performed at one institution
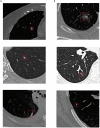
Figures

Similar articles
-
Validation of a deep learning computer aided system for CT based lung nodule detection, classification, and growth rate estimation in a routine clinical population.PLoS One. 2022 May 5;17(5):e0266799. doi: 10.1371/journal.pone.0266799. eCollection 2022. PLoS One. 2022. PMID: 35511758 Free PMC article.
-
Computer-aided diagnosis (CAD) of subsolid nodules: Evaluation of a commercial CAD system.Eur J Radiol. 2016 Oct;85(10):1728-1734. doi: 10.1016/j.ejrad.2016.07.011. Epub 2016 Jul 18. Eur J Radiol. 2016. PMID: 27666609
-
Commercially available computer-aided detection system for pulmonary nodules on thin-section images using 64 detectors-row CT: preliminary study of 48 cases.Acad Radiol. 2009 Aug;16(8):924-33. doi: 10.1016/j.acra.2009.01.030. Epub 2009 Apr 25. Acad Radiol. 2009. PMID: 19394873
-
Is there an advantage to using computer aided detection for the early detection of pulmonary nodules within chest X-Ray imaging?Radiography (Lond). 2020 Aug;26(3):e170-e178. doi: 10.1016/j.radi.2020.01.002. Epub 2020 Jan 29. Radiography (Lond). 2020. PMID: 32052750 Review.
-
Research progress of computer aided diagnosis system for pulmonary nodules in CT images.J Xray Sci Technol. 2020;28(1):1-16. doi: 10.3233/XST-190581. J Xray Sci Technol. 2020. PMID: 31815727 Review.
Cited by
-
Computer-aided Nodule Detection in the Lung Apices in Head and Neck Computed Tomography Angiography: An Unexpected Opportunity.J Thorac Imaging. 2025 Sep 1;40(5):e0836. doi: 10.1097/RTI.0000000000000836. J Thorac Imaging. 2025. PMID: 40485126 Free PMC article.
-
Cross-validation of an artificial intelligence tool for fracture classification and localization on conventional radiography in Dutch population.Insights Imaging. 2025 Jul 3;16(1):150. doi: 10.1186/s13244-025-02034-1. Insights Imaging. 2025. PMID: 40610833 Free PMC article.
-
China Protocol for early screening, precise diagnosis, and individualized treatment of lung cancer.Signal Transduct Target Ther. 2025 May 27;10(1):175. doi: 10.1038/s41392-025-02256-1. Signal Transduct Target Ther. 2025. PMID: 40425545 Free PMC article. Review.
References
-
- All Cancer Fact Sheet, World Health Organization International Agency for Research on Cancer (2020) Available via https://gco.iarc.fr/today/data/factsheets/cancers/39-All-cancers-fact-sh.... Accessed 18 Apr 2023
-
- Gould MK, Tang T, Liu ILA et al (2015) Recent trends in the identification of incidental pulmonary nodules. Am J Respir Crit Care Med 192:1208–1214. 10.1164/rccm.201505-0990OC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

