The Impact of Race/Ethnicity on Disparities in Utilization and Outcomes of Neuraxial Anesthesia for Hip and Femoral Shaft Fractures
- PMID: 39064039
- PMCID: PMC11277043
- DOI: 10.3390/jcm13143999
The Impact of Race/Ethnicity on Disparities in Utilization and Outcomes of Neuraxial Anesthesia for Hip and Femoral Shaft Fractures
Abstract
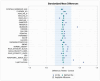
Background/Objectives: The use of neuraxial anesthesia versus general anesthesia for hip fracture surgery remains an active area of research, with recent studies demonstrating mixed findings supporting neuraxial over general anesthesia. The benefits of neuraxial anesthesia have been documented in associated surgeries, including total joint arthroplasty. However, racial disparities in the administration of neuraxial anesthesia have been identified in numerous procedures. We aimed to examine the association of race/ethnicity with neuraxial anesthesia use and the effect of neuraxial anesthesia on length of stay, non-home discharge, 30-day severe adverse events, and rates of readmission among patients undergoing isolated hip and femoral shaft fracture operations. Methods: The American College of Surgeons National Quality Improvement Program database was queried for isolated hip or femoral shaft fractures from 2015 to 2019. Stepwise logistic regression was performed to assess the relationship between race/ethnicity and neuraxial anesthesia use. Within each sex-race stratum, neuraxial anesthesia recipients were propensity-matched to general anesthesia recipients in a 1:2 ratio. Logistic regression and negative binomial regression were performed on the propensity-matched cohort. Results: A total of 12,004 neuraxial and 64,250 general anesthesia hip and femoral shaft fracture patients were identified. Compared to White patients, Black and Hispanic patients were between 0.64 and 0.61 times less likely to receive neuraxial anesthesia over general anesthesia, respectively (p < 0.05). 11,993 patients who received neuraxial anesthesia were propensity matched to 23,946 patients who received general anesthesia. Propensity-matched logistic regressions found that neuraxial anesthesia was associated with decreased length of stay, 30-day severe adverse events, and acute rehab/skilled nursing facility discharge for White patients (p < 0.05 for all), but only decreased length of stay in Black and Hispanic patients (p = 0.01 and p = 0.02, respectively). Conclusions: Notable disparities exist in the administration of neuraxial anesthesia for isolated hip and femoral shaft fracture patients. Hispanic and Black race/ethnicity in particular influences provision of neuraxial anesthesia. Further research is required to understand the degree of effect modification and root causes of regional anesthesia access and benefits for this high-volume patient population.
Keywords: femoral shaft fracture; health disparities; hip fracture; neuraxial anesthesia; regional anesthesia; trauma.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Similar articles
-
Association of race and receipt of regional anesthesia for hip fracture surgery.Reg Anesth Pain Med. 2023 Aug;48(8):392-398. doi: 10.1136/rapm-2022-104055. Epub 2023 Feb 3. Reg Anesth Pain Med. 2023. PMID: 36737100
-
The Frank Stinchfield Award : Total Hip Arthroplasty for Femoral Neck Fracture Is Not a Typical DRG 470: A Propensity-matched Cohort Study.Clin Orthop Relat Res. 2017 Feb;475(2):353-360. doi: 10.1007/s11999-016-4868-2. Clin Orthop Relat Res. 2017. PMID: 27154530 Free PMC article.
-
Racial Disparity in the Perioperative Care for Patients Undergoing Total Knee and Hip Arthroplasty: A Retrospective Propensity-Matched Cohort Study.J Racial Ethn Health Disparities. 2018 Jun;5(3):632-637. doi: 10.1007/s40615-017-0409-2. Epub 2017 Aug 4. J Racial Ethn Health Disparities. 2018. PMID: 28779477
-
General versus Neuraxial Anesthesia on Clinical Outcomes in Patients Receiving Hip Fracture Surgery: An Analysis of the ACS NSQIP Database.J Clin Med. 2023 Jun 2;12(11):3827. doi: 10.3390/jcm12113827. J Clin Med. 2023. PMID: 37298022 Free PMC article.
-
Neuraxial versus general anesthesia in elderly patients undergoing hip fracture surgery and the incidence of postoperative delirium: a systematic review and stratified meta-analysis.BMC Anesthesiol. 2023 Jul 22;23(1):250. doi: 10.1186/s12871-023-02196-9. BMC Anesthesiol. 2023. PMID: 37481517 Free PMC article.
References
-
- Holy C.E., Vanderkarr M., Chitnis A.S., Sparks C. Femoral Shaft Fractures: Treatment Costs and Complication Risks—A Claims Database Analysis. Value Health. 2018;21:S177. doi: 10.1016/j.jval.2018.04.1178. - DOI
Grants and funding
LinkOut - more resources
Full Text Sources