Analysis of Survival Modification by Furosemide Use in a Cohort of Hospitalized COVID-19 Patients with Severe or Critical Disease in Mexico: Due to Its Chemical Structure, Furosemide Is More than Just a Diuretic
- PMID: 39065617
- PMCID: PMC11280466
- DOI: 10.3390/pharmaceutics16070920
Analysis of Survival Modification by Furosemide Use in a Cohort of Hospitalized COVID-19 Patients with Severe or Critical Disease in Mexico: Due to Its Chemical Structure, Furosemide Is More than Just a Diuretic
Abstract
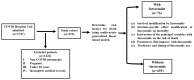
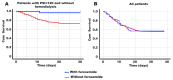
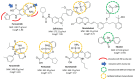
In the ongoing fight against Coronavirus Disease 2019 (COVID-19), researchers are exploring potential treatments to improve outcomes, especially in severe cases. This includes investigating the repurposing of existing medications, such as furosemide, which is widely available. This study aimed to evaluate the impact of furosemide on mortality rates among COVID-19 patients with severe or critical illness. We assessed a cohort of 515 hospitalized adults who experienced a high mortality rate of 43.9%. Using a multivariate analysis with adjusted risk ratios (AdRRs), factors like smoking (AdRR 2.48, 95% CI 1.53-4.01, p < 0.001), a high Pneumonia Severity Index (PSI) score (AdRR 7.89, 95% CI 5.82-10.70, p < 0.001), mechanical ventilation (AdRR 23.12, 95% CI 17.28-30.92, p < 0.001), neutrophilia (AdRR 2.12, 95% CI 1.52-2.95, p < 0.001), and an elevated neutrophil-to-lymphocyte ratio (NLR) (AdRR 2.39, 95% CI 1.72-3.32, p < 0.001) were found to increase mortality risk. In contrast, vaccination and furosemide use were associated with reduced mortality risk (AdRR 0.58, p = 0.001 and 0.60, p = 0.008; respectively). Furosemide showed a pronounced survival benefit in patients with less severe disease (PSI < 120) and those not on hemodialysis, with mortality rates significantly lower in furosemide users (3.7% vs. 25.7%). A Kaplan-Meier analysis confirmed longer survival and better oxygenation levels in patients treated with furosemide. Furthermore, a Structure-Activity Relationship analysis revealed that furosemide's sulfonamide groups may interact with cytokine sites such as tumor necrosis factor-alpha (TNF-α) and interleukin-6 (IL-6), potentially explaining its beneficial effects in COVID-19 management. These findings suggest that furosemide could be a beneficial treatment option in certain COVID-19 patient groups, enhancing survival and improving oxygenation.
Keywords: COVID-19; cohort; furosemide; hospital mortality; structure–activity relation; survival.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
References
-
- World Health Organization (WHO) World Health Organization 2023 Data. Who.Int, WHO Coronavirus (COVID-19) Dashboard > about [Dashboard] [(accessed on 28 April 2024)]. Available online: https://data.who.int/dashboards/covid19/about.
-
- CONACYT (Consejo Nacional de Ciencia y Tecnología) CentroGeo (Centro de Investigación en Ciencias de Información Geoespacial) GeoInt (Laboratorio Nacional de GeoInteligencia) DataLab COVID-19 Tablero México. [(accessed on 19 March 2023)]. Available online: https://datos.covid-19.conacyt.mx/
Grants and funding
LinkOut - more resources
Full Text Sources

