Nalbuphine Potentiates Reversal of Fentanyl Overdose by Naloxone
- PMID: 39065717
- PMCID: PMC11279547
- DOI: 10.3390/ph17070866
Nalbuphine Potentiates Reversal of Fentanyl Overdose by Naloxone
Abstract
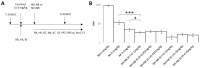
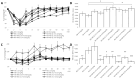
Developing an effective antidote for fentanyl-induced overdose to achieve timely reversal is an unmet public health need. Previously, we found that naloxone derivative NX90 with mild κ-opioid agonistic properties was three-fold more effective than the parent naloxone in reversing a fentanyl overdose in rats. To investigate whether κ-agonistic properties could indeed augment the robustness of overdose reversal, we evaluated a κ-agonist/µ-antagonist nalbuphine (NB) as well as its combinations with naloxone (NX) in a fentanyl overdose model in rodents. An administration of either NB or NX as single agents at 0.1 mg/kg doses produced a full recovery in 90 ± 9.9 min and 11.4 ± 2.7 min, respectively. A higher dose of NX at 0.2 mg/kg reversed an overdose within 4.8 ± 1.0 min. In contrast to that, the coadministration of NB and NX at 0.1 mg/kg each produced a synergistic effect, with overdose reversal in 3.4 ± 0.2 min. The coadministration of NX and NB at sub-therapeutic doses of 0.05 mg/kg each was also 1.2-fold more effective than NX at 0.2 mg/kg. We further found that co-administration of NB at different doses (0.025, 0.05, 0.1 mg/kg) and ratios (1:4 and 1:1) with NX had differential effects on overdose reversal, cardiorespiratory liabilities, and analgesia.
Keywords: fentanyl; nalbuphine; naloxone; overdose reversal; withdrawal.
Conflict of interest statement
Authors Georgiy Nikonov and Michael Voronkov are employed by the company Κappa Pharmaceuticals LLC. Author John Abernethy is employed by the company Serodopa Therapeutics. The remaining authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest. The authors declare that this study received funding from Κappa Pharmaceuticals, LLC, and Serodopa Therapeutics, Inc. The funder was not involved in the study design, collection, analysis, interpretation of data, the writing of this article or the decision to submit it for publication.
Figures
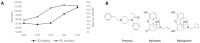

Similar articles
-
Modifying naloxone to reverse fentanyl-induced overdose.Int J Pharm. 2022 Jan 5;611:121326. doi: 10.1016/j.ijpharm.2021.121326. Epub 2021 Nov 27. Int J Pharm. 2022. PMID: 34848365
-
Narcotic reversal in hypercapnic dogs: comparison of naloxone and nalbuphine.Can J Anaesth. 1990 Mar;37(2):238-44. doi: 10.1007/BF03005476. Can J Anaesth. 1990. PMID: 2311152
-
Systemic opioids enhance the spread of sensory analgesia produced by intrathecal lidocaine.Anesth Analg. 1994 Jul;79(1):94-7. doi: 10.1213/00000539-199407000-00018. Anesth Analg. 1994. PMID: 8010462 Clinical Trial.
-
Treatment of opioid overdose: current approaches and recent advances.Psychopharmacology (Berl). 2022 Jul;239(7):2063-2081. doi: 10.1007/s00213-022-06125-5. Epub 2022 Apr 7. Psychopharmacology (Berl). 2022. PMID: 35385972 Free PMC article. Review.
-
The need for multiple naloxone administrations for opioid overdose reversals: A review of the literature.Subst Abus. 2022;43(1):774-784. doi: 10.1080/08897077.2021.2010252. Subst Abus. 2022. PMID: 35112993 Review.
References
-
- Ahmad F.B., Cisewski J.A., Rossen L.M., Sutton P. Provisional Drug Overdose Death Counts. Department of Health and Human Services, National Center for Health Statistics; Atlanta, GA USA: 2023.
-
- Somerville N.J., O’Donnell J., Gladden R.M., Zibbell J.E., Green T.C., Younkin M., Ruiz S., Babakhanlou-Chase H., Chan M., Callis B.P., et al. Characteristics of Fentanyl Overdose-Massachusetts, 2014–2016. MMWR Morb. Mortal. Wkly. Rep. 2017;66:382–386. doi: 10.15585/mmwr.mm6614a2. - DOI - PMC - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

