Occlusio Pupillae: A Duet of Darkness Where the Patient Sees Naught, and the Doctor Discerns Not
- PMID: 39070462
- PMCID: PMC11283770
- DOI: 10.7759/cureus.63370
Occlusio Pupillae: A Duet of Darkness Where the Patient Sees Naught, and the Doctor Discerns Not
Abstract
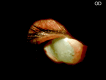
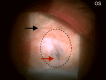
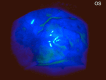
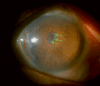
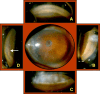
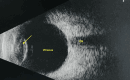
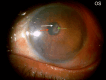
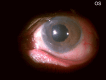
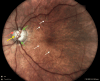
A 71-year-old, one-eyed female patient presented with a loss of vision in the right eye due to trauma 20 years ago and a progressive diminution of vision in the left eye over the past six years. An ambiguous history of some surgery performed on the left eye was elicited, with no available records, adding an element of uncertainty to this case. Visual acuity (VA) was noted as no light perception (No PL) in the right eye and light perception with accurate projection of rays (PL+, PR accurate) in the left eye. Anterior segment slit-lamp evaluation of the right eye showed a shrunken globe with low intraocular pressure (IOP). The left eye exhibited signs of chronic uveitis with occlusio pupillae, non-visualization of the lens, and a doubtful conjunctival bleb with scleral thinning superior to the limbus. B-scan evaluation was suggestive of phthisis in the right eye and an equivocal lens shadow in the left eye. A yttrium aluminum garnet (YAG) pupillary membranotomy was planned for the left eye under steroid cover and was cautiously attempted, successfully detaching the occlusio membrane and revealing an underlying complicated cataract beneath it. Post-laser, medical management included topical anti-glaucoma and steroid medications, along with systemic steroids. The VA improved from PL+, PR accurate to 3/60 (improving to 6/60 with a Retinal Acuity Meter). After stabilization of the uveitis over the next few weeks and under a steroid cover, a temporal clear-corneal phacoemulsification was cautiously performed with intra-operative management of the small pupil, and a hydrophobic lens was implanted. At one month post-surgery, the patient's best-corrected visual acuity had improved to 6/12 for distance and N6 for near. This report highlights a compelling instance wherein the neodymium:Yttrium-aluminum-garnet (Nd:YAG) laser was efficaciously employed for a lesser-known application in resolving a diagnostic dilemma and for instituting an interim treatment strategy in a challenging case involving a one-eyed patient prior to planning a definitive surgery. This case emphasizes the importance of thinking out of the box, ensuring comprehensive preoperative and careful intra-operative precautions in the management of patients diagnosed with complex ocular inflammatory conditions, so as to optimize visual outcomes, eventually resulting in achieving a gratifying reduction of visual disability and improvement of quality of life.
Keywords: complicated cataract; glaucoma; neodymium:yttrium-aluminum-garnet (nd:yag) laser applications; occlusio pupillae; one-eyed patient; phacoemulsification; phthisical eye; pseudo-bleb; uveitis; yag pupillary membranotomy.
Copyright © 2024, Hingorani-Bang et al.
Conflict of interest statement
Human subjects: Consent was obtained or waived by all participants in this study. Conflicts of interest: In compliance with the ICMJE uniform disclosure form, all authors declare the following: Payment/services info: All authors have declared that no financial support was received from any organization for the submitted work. Financial relationships: All authors have declared that they have no financial relationships at present or within the previous three years with any organizations that might have an interest in the submitted work. Other relationships: All authors have declared that there are no other relationships or activities that could appear to have influenced the submitted work.
Figures




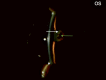


Similar articles
-
A randomized controlled trial of peeling and aspiration of Elschnig pearls and neodymium: yttrium-aluminium-garnet laser capsulotomy.Int J Ophthalmol. 2015 Jun 18;8(3):590-6. doi: 10.3980/j.issn.2222-3959.2015.03.28. eCollection 2015. Int J Ophthalmol. 2015. PMID: 26086014 Free PMC article.
-
Evaluation of posterior capsular opacification and neodymium-doped yttrium aluminum garnet capsulotomy rates in patients with hydrophilic intraocular lens implantation with and without ocular viscoelastic device.Indian J Ophthalmol. 2022 Oct;70(10):3529-3533. doi: 10.4103/ijo.IJO_678_22. Indian J Ophthalmol. 2022. PMID: 36190041 Free PMC article. Clinical Trial.
-
Recurrent late-onset fibrotic capsular block syndrome after neodymium-yttrium-aluminum-garnet laser anterior capsulotomy: a case report.BMC Ophthalmol. 2016 Jun 11;16:86. doi: 10.1186/s12886-016-0261-x. BMC Ophthalmol. 2016. PMID: 27287252 Free PMC article.
-
Cyclodestructive procedures for refractory glaucoma.Cochrane Database Syst Rev. 2019 Mar 10;3(3):CD012223. doi: 10.1002/14651858.CD012223.pub2. Cochrane Database Syst Rev. 2019. PMID: 30852841 Free PMC article.
-
Why not Y naught.Heredity (Edinb). 2022 Aug;129(2):75-78. doi: 10.1038/s41437-022-00543-z. Epub 2022 May 17. Heredity (Edinb). 2022. PMID: 35581478 Free PMC article. Review. No abstract available.
Cited by
-
A Case of Intraocular Pressure Elevation Secondary to Pupillary Occlusion.Cureus. 2025 May 27;17(5):e84917. doi: 10.7759/cureus.84917. eCollection 2025 May. Cureus. 2025. PMID: 40575243 Free PMC article.
References
-
- Neodymium: YAG laser iridolenticular synechiolysis in uveitis. Kumar H, Ahuja S, Garg SP. https://europepmc.org/article/MED/8058259. Ophthalmic Surg. 1994;25:288–291. - PubMed
-
- Role of neodymium: Yttrium-aluminum-garnet laser in occlusio pupillae and iridolenticular ring synechiae. Khurana G, Prakash O, Jain R. MAMC J Med Sci. 2016;2:102.
-
- Vitreoretinal changes associated with rise in intraocular pressure after Nd:YAG capsulotomy. Schubert HD. https://doi.org/10.3928/1542-8877-19870101-07 Ophthalmic Surg. 1987;25:19–22. - PubMed
-
- Uveitis in developing countries. Rao NA. https://pubmed.ncbi.nlm.nih.gov/23803475/ Indian J Ophthalmol. 2013;61:253–254. - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous
