Projected Changes in Statin and Antihypertensive Therapy Eligibility With the AHA PREVENT Cardiovascular Risk Equations
- PMID: 39073797
- PMCID: PMC11287447
- DOI: 10.1001/jama.2024.12537
Projected Changes in Statin and Antihypertensive Therapy Eligibility With the AHA PREVENT Cardiovascular Risk Equations
Abstract
Importance: Since 2013, the American College of Cardiology (ACC) and American Heart Association (AHA) have recommended the pooled cohort equations (PCEs) for estimating the 10-year risk of atherosclerotic cardiovascular disease (ASCVD). An AHA scientific advisory group recently developed the Predicting Risk of cardiovascular disease EVENTs (PREVENT) equations, which incorporated kidney measures, removed race as an input, and improved calibration in contemporary populations. PREVENT is known to produce ASCVD risk predictions that are lower than those produced by the PCEs, but the potential clinical implications have not been quantified.
Objective: To estimate the number of US adults who would experience changes in risk categorization, treatment eligibility, or clinical outcomes when applying PREVENT equations to existing ACC and AHA guidelines.
Design, setting, and participants: Nationally representative cross-sectional sample of 7765 US adults aged 30 to 79 years who participated in the National Health and Nutrition Examination Surveys of 2011 to March 2020, which had response rates ranging from 47% to 70%.
Main outcomes and measures: Differences in predicted 10-year ASCVD risk, ACC and AHA risk categorization, eligibility for statin or antihypertensive therapy, and projected occurrences of myocardial infarction or stroke.
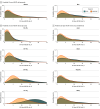
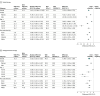
Results: In a nationally representative sample of 7765 US adults aged 30 to 79 years (median age, 53 years; 51.3% women), it was estimated that using PREVENT equations would reclassify approximately half of US adults to lower ACC and AHA risk categories (53.0% [95% CI, 51.2%-54.8%]) and very few US adults to higher risk categories (0.41% [95% CI, 0.25%-0.62%]). The number of US adults receiving or recommended for preventive treatment would decrease by an estimated 14.3 million (95% CI, 12.6 million-15.9 million) for statin therapy and 2.62 million (95% CI, 2.02 million-3.21 million) for antihypertensive therapy. The study estimated that, over 10 years, these decreases in treatment eligibility could result in 107 000 additional occurrences of myocardial infarction or stroke. Eligibility changes would affect twice as many men as women and a greater proportion of Black adults than White adults.
Conclusion and relevance: By assigning lower ASCVD risk predictions, application of the PREVENT equations to existing treatment thresholds could reduce eligibility for statin and antihypertensive therapy among 15.8 million US adults.
Conflict of interest statement
Figures


Comment in
-
The Evolving Landscape of Cardiovascular Risk Assessment.JAMA. 2024 Sep 24;332(12):967-969. doi: 10.1001/jama.2024.13247. JAMA. 2024. PMID: 39073798 No abstract available.
References
-
- Goff DC Jr, Lloyd-Jones DM, Bennett G, et al. 2013 ACC/AHA guideline on the assessment of cardiovascular risk: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 2014;63(25 pt B):2935-2959. doi: 10.1016/j.jacc.2013.11.005 - DOI - PMC - PubMed
-
- Grundy SM, Stone NJ, Bailey AL, et al. 2018 AHA/ACC/AACVPR/AAPA/ABC/ACPM/ADA/AGS/APhA/ASPC/NLA/PCNA guideline on the management of blood cholesterol: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation. 2019;139(25):e1082-e1143. doi: 10.1161/CIR.0000000000000625 - DOI - PMC - PubMed
-
- Whelton PK, Carey RM, Aronow WS, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation. 2018;138(17):e426-e483.doi: 10.1161/CIR.0000000000000597 - DOI - PubMed
-
- Arnett DK, Blumenthal RS, Albert MA, et al. 2019 ACC/AHA guideline on the primary prevention of cardiovascular disease: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation. 2019;140(11):e596-e646. doi: 10.1161/CIR.0000000000000678 - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

