Kidney Blood Flow and Renin-Angiotensin-Aldosterone System Measurements Associated With Kidney and Cardiovascular Dysfunction in Pediatric Shock
- PMID: 39110074
- PMCID: PMC11309640
- DOI: 10.1097/CCE.0000000000001134
Kidney Blood Flow and Renin-Angiotensin-Aldosterone System Measurements Associated With Kidney and Cardiovascular Dysfunction in Pediatric Shock
Abstract
Importance: Pediatric acute kidney injury (AKI) is a prevalent and morbid complication of shock. Its pathogenesis and early identification remain elusive.
Objectives: We aim to determine whether renal blood flow (RBF) measurements by point-of-care ultrasound (POCUS) and renin-angiotensin-aldosterone system (RAAS) hormones in pediatric shock associate with vasoactive requirements and AKI.
Design, setting, and participants: This is a single-center prospective, noninterventional observational cohort study in one tertiary PICU in North American from 2020 to 2022 that enrolled children younger than 18 years with shock without preexisting end-stage renal disease.
Main outcomes and measures: RBF was measured by POCUS on hospital days 1 and 3 and plasma RAAS hormone levels were measured on day 1. The primary outcome was the presence of AKI by Kidney Disease Improving Global Outcomes criteria at first ultrasound with key secondary outcomes of creatinine, blood urea nitrogen (BUN), Vasoactive-Inotrope Score (VIS), and norepinephrine equivalent dosing (NED) 48 hours after first ultrasound.
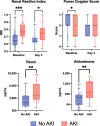
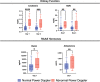
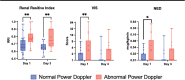
Results: Fifty patients were recruited (20 with AKI, mean age 10.5 yr, 48% female). POCUS RBF showed lower qualitative blood flow (power Doppler ultrasound [PDU] score) and higher regional vascular resistance (renal resistive index [RRI]) in children with AKI (p = 0.017 and p = 0.0007). Renin and aldosterone levels were higher in the AKI cohort (p = 0.003 and p = 0.007). Admission RRI and PDU associated with higher day 3 VIS and NED after adjusting for age, day 1 VIS, and RAAS hormones. Admission renin associated with higher day 3 creatinine and BUN after adjusting for age, day 1 VIS, and the ultrasound parameters.
Conclusions and relevance: In pediatric shock, kidney blood flow was abnormal and renin and aldosterone were elevated in those with AKI. Kidney blood flow abnormalities are independently associated with future cardiovascular dysfunction; renin elevations are independently associated with future kidney dysfunction. Kidney blood flow by POCUS may identify children who will have persistent as opposed to resolving AKI. RAAS perturbations may drive AKI in pediatric shock.
Copyright © 2024 The Authors. Published by Wolters Kluwer Health, Inc. on behalf of the Society of Critical Care Medicine.
Conflict of interest statement
Dr. Taylor received a grant through the National Institute of General Medicine, K08 National Institutes of Health GM132794. Drs. Taylor and Deutschman received Angiotensin II (Giapreza) for murine research in the cecal ligation and puncture model of sepsis from La Jolla Pharmaceutical Company/InnoViva Specialty Therapeutics. The remaining authors have disclosed that they do not have any potential conflicts of interest.
Figures
References
-
- Schneider J, Khemani R, Grushkin C, et al. : Serum creatinine as stratified in the RIFLE score for acute kidney injury is associated with mortality and length of stay for children in the pediatric intensive care unit. Crit Care Med 2010; 38:933–939 - PubMed
-
- Fitzgerald JC, Basu RK, Akcan-Arikan A, et al. ; Sepsis PRevalence, OUtcomes, and Therapies Study Investigators and Pediatric Acute Lung Injury and Sepsis Investigators Network: Acute kidney injury in pediatric severe sepsis: An independent risk factor for death and new disability. Crit Care Med 2016; 44:2241–2250 - PMC - PubMed
-
- Anastasio P, Cirillo M, Spitali L, et al. : Level of hydration and renal function in healthy humans. Kidney Int 2001; 60:748–756 - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

