Drug resistance in drug-resistant tuberculosis patients with and without diabetes mellitus: a comparative analysis
- PMID: 39123148
- PMCID: PMC11316371
- DOI: 10.1186/s12879-024-09712-3
Drug resistance in drug-resistant tuberculosis patients with and without diabetes mellitus: a comparative analysis
Abstract
Background: This dual burden of tuberculosis (TB) and diabetes mellitus (DM) has become a global public health concern. This study aims to compare drug resistance in drug-resistant tuberculosis (DR-TB) patients with and without DM and analyse the risk factors of multidrug-resistant tuberculosis (MDR-TB).
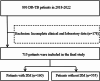
Methods: A total of 893 DR-TB patients were admitted to Wenzhou Central Hospital between January 2018 and December 2022. After excluding 178 cases with incomplete clinical and laboratory data, 715 patients were included in the study. These patients were then categorized into two groups based on the presence of type 2 DM: the DM group (160 cases) and the non-DM group (555 cases). Demographic information, baseline clinical characteristics, laboratory and imaging test results, clinical diagnoses, and other relevant data were collected for analysis. Statistical analysis was conducted on demographic information, clinical parameters, drug resistance spectrum, and risk factors for multidrug resistance.
Results: In both the DM and non-DM groups, the order of resistance to first-line anti-tuberculosis drugs is isoniazid, streptomycin, rifampicin, and ethambutol. There is no significant difference in the proportion of mono-resistant tuberculosis, polydrug-resistant tuberculosis, and multidrug-resistant tuberculosis between the two groups (P > 0.05). The prevalence of MDR-TB in both groups shows a downward trend between 2018 and 2022, but the trend is not statistically significant (P > 0.05). Among patients without DM, residence in rural areas, retreatment of tuberculosis, pulmonary cavity, and uric acid ≥ 346 µmol/L are identified as independent risk factors for MDR-TB. Among patients with DM, residence in rural areas, retreatment of tuberculosis, pulmonary cavity, and HbA1c ≥ 9.8% were identified as independent risk factors for MDR-TB.
Conclusion: Isoniazid is the most resistant drug among DR-TB patients with and without DM. There is no statistically significant difference in drug resistance patterns between the two groups. Some progress has been made in the prevention and control of DR-TB in this area, but the effect is not very significant. There are differences in the risk factors of MDR-TB between patients with and without DM.
Keywords: Diabetes mellitus; Drug resistance profile; Drug-resistant tuberculosis; Multidrug-resistant tuberculosis; Risk factors.
© 2024. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures


Similar articles
-
The differences in drug resistance between drug-resistant tuberculosis patients with and without diabetes mellitus in northeast China: a retrospective study.BMC Infect Dis. 2023 Mar 15;23(1):162. doi: 10.1186/s12879-023-08130-1. BMC Infect Dis. 2023. PMID: 36922787 Free PMC article.
-
Prevalence and drug resistance profile of Mycobacterium tuberculosis isolated from pulmonary tuberculosis patients attending two public hospitals in East Gojjam zone, northwest Ethiopia.BMC Public Health. 2015 Jun 20;15:572. doi: 10.1186/s12889-015-1933-9. BMC Public Health. 2015. PMID: 26092570 Free PMC article.
-
First-line tuberculosis drug resistance patterns and associated risk factors in Germany, 2008-2017.PLoS One. 2019 Jun 12;14(6):e0217597. doi: 10.1371/journal.pone.0217597. eCollection 2019. PLoS One. 2019. PMID: 31188848 Free PMC article.
-
Prevalence and patterns of drug-resistant Mycobacterium tuberculosis in newly diagnosed patients in China: A systematic review and meta-analysis.J Glob Antimicrob Resist. 2024 Sep;38:292-301. doi: 10.1016/j.jgar.2024.05.018. Epub 2024 May 31. J Glob Antimicrob Resist. 2024. PMID: 38825149
-
A novel risk factor for predicting anti-tuberculosis drug resistance in patients with tuberculosis complicated with type 2 diabetes mellitus.Int J Infect Dis. 2020 Aug;97:69-77. doi: 10.1016/j.ijid.2020.05.080. Epub 2020 May 29. Int J Infect Dis. 2020. PMID: 32474202
Cited by
-
Trends in Drug Resistance and Epidemiological Patterns of Tuberculosis in Elderly Patients in Wenzhou, China (2014-2023).Infect Drug Resist. 2025 Jul 12;18:3459-3470. doi: 10.2147/IDR.S530067. eCollection 2025. Infect Drug Resist. 2025. PMID: 40671759 Free PMC article.
References
-
- WHO. Global tuberculosis report 2023. In Geneva. World Health Organization; 2023.
-
- Saeedi P, Petersohn I, Salpea P, Malanda B, Karuranga S, Unwin N, et al. Global and regional diabetes prevalence estimates for 2019 and projections for 2030 and 2045: results from the International Diabetes Federation Diabetes Atlas, 9(th) edition. Diabetes Res Clin Pract. 2019;157:107843. 10.1016/j.diabres.2019.107843 - DOI - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

