Myocardial Fibrosis in Young and Veteran Athletes: Evidence from a Systematic Review of the Current Literature
- PMID: 39124802
- PMCID: PMC11313657
- DOI: 10.3390/jcm13154536
Myocardial Fibrosis in Young and Veteran Athletes: Evidence from a Systematic Review of the Current Literature
Abstract
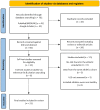
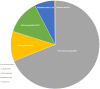
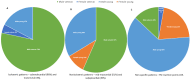
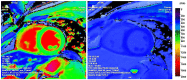
Background: Exercise is associated with several cardiac adaptations that can enhance one's cardiac output and allow one to sustain a higher level of oxygen demand for prolonged periods. However, adverse cardiac remodelling, such as myocardial fibrosis, has been identified in athletes engaging in long-term endurance exercise. Cardiac magnetic resonance (CMR) imaging is considered the noninvasive gold standard for its detection and quantification. This review seeks to highlight factors that contribute to the development of myocardial fibrosis in athletes and provide insights into the assessment and interpretation of myocardial fibrosis in athletes. Methods: A literature search was performed using the PubMed/Medline database and Google Scholar for publications that assessed myocardial fibrosis in athletes using CMR. Results: A total of 21 studies involving 1642 endurance athletes were included in the analysis, and myocardial fibrosis was found in 378 of 1595 athletes. A higher prevalence was seen in athletes with cardiac remodelling compared to control subjects (23.7 vs. 3.3%, p < 0.001). Similarly, we found that young endurance athletes had a significantly higher prevalence than veteran athletes (27.7 vs. 19.9%, p < 0.001), while male and female athletes were similar (19.7 vs. 16.4%, p = 0.207). Major myocardial fibrosis (nonischaemic and ischaemic patterns) was predominately observed in veteran athletes, particularly in males and infrequently in young athletes. The right ventricular insertion point was the most common fibrosis location, occurring in the majority of female (96%) and young athletes (84%). Myocardial native T1 values were significantly lower in athletes at 1.5 T (p < 0.001) and 3 T (p = 0.004), although they had similar extracellular volume values to those of control groups. Conclusions: The development of myocardial fibrosis in athletes appears to be a multifactorial process, with genetics, hormones, the exercise dose, and an adverse cardiovascular risk profile playing key roles. Major myocardial fibrosis is not a benign finding and warrants a comprehensive evaluation and follow-up regarding potential cardiac disease.
Keywords: T1 mapping; cardiac magnetic resonance imaging; endurance athlete; late gadolinium enhancement; myocardial fibrosis.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
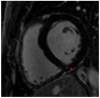
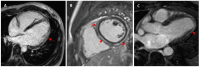
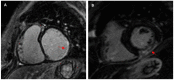
References
-
- Androulakis E., Mouselimis D., Tsarouchas A., Antonopoulos A., Bakogiannis C., Papagkikas P., Vlachopoulos C. The Role of Cardiovascular Magnetic Resonance Imaging in the Assessment of Myocardial Fibrosis in Young and Veteran Athletes: Insights from a Meta-Analysis. Front. Cardiovasc. Med. 2021;8:784474. doi: 10.3389/fcvm.2021.784474. - DOI - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources

