Reducing Blood Culture Contamination Rates: Introduction of a Combined Education and Skin Antisepsis Intervention
- PMID: 39130732
- PMCID: PMC11316574
- DOI: 10.1099/acmi.0.000806.v3
Reducing Blood Culture Contamination Rates: Introduction of a Combined Education and Skin Antisepsis Intervention
Abstract
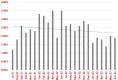
Background. Blood culture contamination (BCC) is an important quality concern in clinical microbiology as it can lead to unnecessary antimicrobial therapy in patients and increased workload for laboratory scientists. The Clinical Laboratory and Standards Institute recommend BCC rates to be <3 % and recently updated guidelines have set a new goal of 1 %. The aim of this project was to design and implement interventions to reduce BCC rates at our institution. Methods. We introduced a combined education and skin antisepsis intervention in a large Model 4 academic teaching hospital in the South of Ireland. BD ChloraPrep skin antisepsis applicators (2 % chlorhexidine gluconate/70 % isopropyl alcohol), licensed for use for blood culture specimen collection, were introduced, replacing Clinell (2 % chlorhexidine gluconate/70 % isopropyl alcohol) wipes. In addition, a multimodal education programme was designed and delivered. This consisted of a video demonstrating the recommended blood culture specimen collection technique using the new applicators as well as simulation training for all interns. The video was uploaded to the intranet as an educational resource available to all staff. Results. The interventions were implemented in July 2022 and BCC rates pre- and post-intervention were calculated. The average BCC rate for the 12 months preceding the intervention (July 2021 to July 2022) was 2.56 % with highest rates in the Emergency Department. This compared to an average rate of 2.2 % in the 12 months post-intervention (July 2022 to July 2023). In comparing the two rates the reduction in BCC rates between the two periods was not statistically significant (P=0.30). Conclusion. Overall BCC rates reduced but the difference between the two periods did not reach statistical significance. The resource-intensive nature of providing regular and timely feedback of contamination rates and the larger impact of in-person education and training over virtual modalities may explain the modest reduction. Further investments in these areas, particularly in the Emergency Department, will be necessary to further reduce rates in line with new recommendations.
Keywords: blood culture contamination; education; intervention; simulation training; skin antisepsis.
Copyright © 2024 The Authors.
Conflict of interest statement
The authors declare that there are no conflicts of interest.
Figures
References
-
- World Health Organization Global action plan on antimicrobial resistance. 2016. [10-October-2023]. https://www.who.int/publications accessed.
LinkOut - more resources
Full Text Sources