The Prognostic Value of Troponin-T in Out-of-Hospital Cardiac Arrest Without ST-Segment Elevation: A COACT Substudy
- PMID: 39132217
- PMCID: PMC11308418
- DOI: 10.1016/j.jscai.2023.101191
The Prognostic Value of Troponin-T in Out-of-Hospital Cardiac Arrest Without ST-Segment Elevation: A COACT Substudy
Abstract
Background: In out-of-hospital cardiac arrest (OHCA) without ST-elevation, predictive markers that can identify those with a high risk of acute coronary syndrome are lacking.
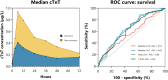
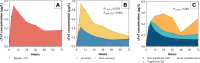
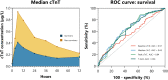
Methods: In this post hoc analysis of the Coronary Angiography after Cardiac Arrest (COACT) trial, the baseline, median, peak, and time-concentration curves of troponin-T (cTnT) (T-AUC) in OHCA patients without ST-elevation were studied. cTnT values were obtained at predefined time points at 0, 3, 6, 12, 24, 36, 28, and 72 hours after admission. All patients who died within the measurement period were not included. The primary outcome was the association between cTnT and 90-day survival. Secondary outcomes included the association of cTnT and acute thrombotic occlusions, acute unstable lesions, and left ventricular function.
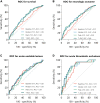
Results: In total, 352 patients were included in the analysis. The mean age was 64 ± 13 years (80.4% men). All cTnT measures were independent prognostic factors for mortality after adjustment for potential confounders age, sex, history of coronary artery disease, witnessed arrest, time to BLS, and time to return of spontaneous circulation (eg, for T-AUC: hazard ratio, 1.44; 95% CI, 1.06-1.94; P = .02; P value for all variables ≤.02). Median cTnT (odds ratio [OR], 1.58; 95% CI, 1.18-2.12; P = .002) and T-AUC (OR, 2.03; 95% CI, 1.25-3.29; P = .004) were independent predictors for acute unstable lesions. Median cTnT (OR, 1.62; 95% CI, 1.17-2.23; P = .003) and T-AUC (OR, 2.16; 95% CI, 1.27-3.68; P = .004) were independent predictors for acute thrombotic occlusions. CTnT values were not associated with the left ventricular function (eg, for T-AUC: OR, 2.01; 95% CI, 0.65-6.19; P = .22; P value for all variables ≥.14).
Conclusion: In OHCA patients without ST-segment elevation, cTnT release during the first 72 hours after return of spontaneous circulation was associated with clinical outcomes.
Keywords: acute coronary syndrome; coronary angiography; out-of-hospital cardiac arrest.
© 2023 The Author(s).
Figures
References
LinkOut - more resources
Full Text Sources
Research Materials

