Association of weight-adjusted waist index with cardiovascular disease and mortality among metabolic syndrome population
- PMID: 39134613
- PMCID: PMC11319818
- DOI: 10.1038/s41598-024-69486-1
Association of weight-adjusted waist index with cardiovascular disease and mortality among metabolic syndrome population
Abstract
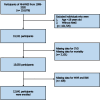
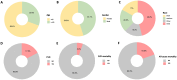
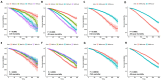
Metabolic syndrome (MetS) is prevalent and significantly impacts global public health, with obesity being a major risk factor for cardiovascular diseases (CVD) and mortality. Traditional metrics like body mass index (BMI) have limitations in assessing obesity-related risks. The weight-adjusted waist circumference index (WWI) has emerged as a novel obesity metric, this study aimed to evaluate the association of WWI with CVD and mortality in MetS patients. This study used data from 12,641 participants with MetS, derived from the National Health and Nutrition Examination Survey (NHANES) conducted from 1999 to 2020. The WWI was calculated, and its association with CVD and mortality was assessed using multivariate logistic and Cox regression models. The study controlled for potential confounders and performed subgroup and sensitivity analyses to validate the robustness of the findings. The predictive performance of WWI was evaluated using the area under the receiver operating characteristic curve (ROC). Kaplan-Meier (KM) curves further were used to evaluate the associations between WWI and mortality of the MetS population. As WWI values escalated, there was a proportional rise in the risk of CVD and mortality in MetS. The fully adjusted continuous model revealed a 32.0% elevated likelihood of CVD development, a 69.5% increased probability of heart failure (HF), a 51.1% heightened risk for CVD mortality, and a 22.8% augmented risk for all-cause mortality with each one-unit increment in WWI. Comparing the highest to the lowest quartile of WWI, the top quartile exhibited a significantly increased risk of CVD (odds ratio [OR] = 1.883; 95% confidence interval [CI]: 1.276-2.633, p-value = 0.001), HF (OR = 2.909; 95% CI: 1.490-5.677, p-value = 0.002), CVD mortality (hazard ratio [HR] = 2.088; 95% CI: 1.279-3.409, p-value = 0.003), and all-cause mortality (HR = 1.394; 95% CI: 1.070-1.816, p-value = 0.014) among individuals with MetS. Sensitivity and subgroup analyses substantiated the consistency and stability of these associations across various demographic groups. The ROC analysis demonstrated that WWI outperforms BMI in predicting adverse outcomes in MetS. The KM curves validated that higher WWI values was correlated with diminished survival rates in MetS population. The WWI served as a significant indicator for assessing the risk of CVD and mortality in the MetS population. This study recommended the regular assessment of WWI in MetS individuals for evaluating their risk of CVD and mortality, potentially enhancing preventive and treatment strategies for this patient population.
Keywords: MetS; Metabolic syndrome; NHANES; WWI; Weight-adjusted waist circumference index.
© 2024. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures


Similar articles
-
The association between weight-adjusted waist circumference index and cardiovascular disease and mortality in patients with diabetes.Sci Rep. 2024 Aug 16;14(1):18973. doi: 10.1038/s41598-024-69712-w. Sci Rep. 2024. PMID: 39152145 Free PMC article.
-
Association of weight-adjusted waist index with all-cause and cardiovascular disease mortality among rheumatoid arthritis population: a cohort study from the NHANES 1999-2018.Lipids Health Dis. 2025 Jul 1;24(1):223. doi: 10.1186/s12944-025-02594-7. Lipids Health Dis. 2025. PMID: 40597197 Free PMC article.
-
Weight-adjusted waist index is positively and linearly associated with all-cause and cardiovascular mortality in metabolic dysfunction-associated steatotic liver disease: findings from NHANES 1999-2018.Front Endocrinol (Lausanne). 2024 Sep 30;15:1457869. doi: 10.3389/fendo.2024.1457869. eCollection 2024. Front Endocrinol (Lausanne). 2024. PMID: 39403588 Free PMC article.
-
Association of body roundness index with cardiovascular disease in patients with cardiometabolic syndrome: a cross-sectional study based on NHANES 2009-2018.Front Endocrinol (Lausanne). 2025 Feb 3;16:1524352. doi: 10.3389/fendo.2025.1524352. eCollection 2025. Front Endocrinol (Lausanne). 2025. PMID: 39963283 Free PMC article. Review.
-
Association between Weight-Adjusted Waist Index and depressive symptoms: A nationally representative cross-sectional study from NHANES 2005 to 2018.J Affect Disord. 2024 Apr 1;350:49-57. doi: 10.1016/j.jad.2024.01.104. Epub 2024 Jan 12. J Affect Disord. 2024. PMID: 38220117 Review.
Cited by
-
The interplay of factors in metabolic syndrome: understanding its roots and complexity.Mol Med. 2024 Dec 27;30(1):279. doi: 10.1186/s10020-024-01019-y. Mol Med. 2024. PMID: 39731011 Free PMC article. Review.
-
Weight-Adjusted Waist Index, Psoriasis, and All-Cause Mortality: Findings from the NHANES 2003-2006 and 2009-2014.Clin Cosmet Investig Dermatol. 2025 Jan 4;18:7-18. doi: 10.2147/CCID.S497128. eCollection 2025. Clin Cosmet Investig Dermatol. 2025. PMID: 39781099 Free PMC article.
-
Weight-Adjusted Waist Index: an anthropometric measure for frailty in older adults.Eur Geriatr Med. 2024 Dec;15(6):1731-1738. doi: 10.1007/s41999-024-01047-1. Epub 2024 Sep 5. Eur Geriatr Med. 2024. PMID: 39237732
-
The Impact of Kefir Consumption on Inflammation, Oxidative Stress Status, and Metabolic-Syndrome-Related Parameters in Animal Models: A Systematic Review and Meta-Analysis.Foods. 2025 Jun 12;14(12):2077. doi: 10.3390/foods14122077. Foods. 2025. PMID: 40565686 Free PMC article. Review.
-
Triglyceride glucose-weight-adjusted waist index (TyG-WWI): the best predictor of diabetes mellitus and mortality risks among TyG and TyG-derived indices.BMC Endocr Disord. 2025 Jul 4;25(1):166. doi: 10.1186/s12902-025-01989-y. BMC Endocr Disord. 2025. PMID: 40616082 Free PMC article.
References
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

