Patterns and unique features of infantile cholestasis among Arabs
- PMID: 39139600
- PMCID: PMC11319143
- DOI: 10.3389/fped.2024.1423657
Patterns and unique features of infantile cholestasis among Arabs
Abstract
Background: Most of the literature on infantile cholestasis (IC) originated from Caucasian and Asian populations. The differential diagnosis of IC is very broad, and identification of etiology is challenging to clinicians because the list includes many entities with overlapping clinical, biochemical, and histological features. Thus, a structured, stepwise diagnostic approach is required to help early recognition and prompt evaluation and management of treatable causes of cholestasis.
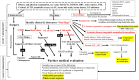
Objective: (1) To determine the differential diagnosis of IC among Saudi population and (2) to evaluate the usefulness of a diagnostic algorithm that has been tailored by the authors to the local practice.
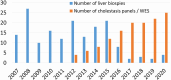
Methods: All infants with onset of cholestasis before 12 months of age (2007 and 2020) were identified and included if they underwent extensive work up to exclude infectious, structural, metabolic, endocrine, infiltrative, and familial causes.
Results: Our diagnostic pathway allowed a definite diagnosis in 373 of the included 533 cases; 160 (30%) were labelled as "idiopathic neonatal hepatitis" (INH) [i.e., overall 70% detection rate]. However, when considering the cases that underwent extensive investigations including advanced gene testing (415 of the 533), the yield of the diagnostic algorithm was 90% (373/415). Familial cholestasis group was the most common in 20% (107/533), and biliary atresia and neonatal-onset Dubin Johnson syndrome contributed to 6% each. The genetic/hereditary causes of cholestasis contributed to 58% of the diagnosed cases (217/373). No single case of alpha-1 antitrypsin deficiency was diagnosed. Forty-nine infants with cholestasis presented with liver failure (9%).
Conclusion: Our study highlights several unique features and causes of IC among Arabs which could have a great impact on the differential diagnosis process and the choice of laboratory tests used in the clinical setting.
Keywords: Saudi Arabia; idiopathic neonatal hepatitis; liver disease; next-generation sequence; whole exome sequence.
© 2024 Al-Hussaini, Alrashidi, Hafez, Alkhalifah, Otayn, Alrasheed, Al Mufarreh and AlKasim.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Diagnostic Yield of an Algorithm for Neonatal and Infantile Cholestasis Integrating Next-Generation Sequencing.J Pediatr. 2019 Aug;211:54-62.e4. doi: 10.1016/j.jpeds.2019.04.016. Epub 2019 May 31. J Pediatr. 2019. PMID: 31160058
-
Role of percutaneous liver biopsy in infantile cholestasis: cohort from Arabs.BMC Gastroenterol. 2021 Mar 12;21(1):118. doi: 10.1186/s12876-021-01699-4. BMC Gastroenterol. 2021. PMID: 33711954 Free PMC article.
-
A new diagnostic approach to biliary atresia with emphasis on the ultrasonographic triangular cord sign: comparison of ultrasonography, hepatobiliary scintigraphy, and liver needle biopsy in the evaluation of infantile cholestasis.J Pediatr Surg. 1997 Nov;32(11):1555-9. doi: 10.1016/s0022-3468(97)90451-6. J Pediatr Surg. 1997. PMID: 9396524
-
Urinary coproporphyrins as a diagnostic biomarker of Dubin-Johnson syndrome in neonates: A diagnostic pathway is proposed.Saudi J Gastroenterol. 2023 May-Jun;29(3):183-190. doi: 10.4103/sjg.sjg_480_22. Saudi J Gastroenterol. 2023. PMID: 37313948 Free PMC article. Review.
-
Recent developments in diagnostics and treatment of neonatal cholestasis.Semin Pediatr Surg. 2020 Aug;29(4):150945. doi: 10.1016/j.sempedsurg.2020.150945. Epub 2020 Jul 23. Semin Pediatr Surg. 2020. PMID: 32861449 Free PMC article. Review.
References
LinkOut - more resources
Full Text Sources

