Should Prophylactic Endotracheal Intubation Be Performed in Upper Gastrointestinal Bleeding?
- PMID: 39144893
- PMCID: PMC11323713
- DOI: 10.7759/cureus.64567
Should Prophylactic Endotracheal Intubation Be Performed in Upper Gastrointestinal Bleeding?
Abstract
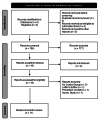
No consensus exists on the standard of intraoperative airway management approach to prevent endoscopy complications in acute gastrointestinal (GI) bleeding. Eight years after our initial meta-analysis, we reassessed the effect of prophylactic endotracheal intubation in acute GI bleeding in hospitalized patients. Multiple databases were reviewed in 2024, identifying 10 studies that compared prophylactic endotracheal intubation (PEI) versus no intubation in acute upper GI bleeding in hospitalized patients. Outcomes of interest included pneumonia, length of hospital stay, aspiration, and mortality. The odds ratio (OR) or mean difference (MD) using the random effects model was calculated for each outcome. In total, 11 studies (10 retrospective, one prospective) were included in the meta-analysis (n = 7,332). PEI demonstrated statistically significant higher odds of pneumonia (OR = 5.83; 95% confidence interval (CI) = 3.15-10.79; p < 0.01) and longer length of stays (MD = 0.84; 95% CI = 0.12-1.56; p = 0.02). However, mortality (OR = 1.68; 95% CI = 0.78-3.64; p = 0.19) and aspiration (OR = 2.79; 95% CI = 0.89-8.7; p = 0.08) were not statistically significant. PEI before esophagogastroduodenoscopy for hospitalized upper GI bleeding patients is associated with an increased incidence of pneumonia within 48 hours and prolonged hospitalization but no statistically significant increased risk of mortality or aspiration.
Keywords: bleeding; length of stay; meta-analysis; pneumonia; prophylactic intubation.
Copyright © 2024, Pasha et al.
Conflict of interest statement
Conflicts of interest: In compliance with the ICMJE uniform disclosure form, all authors declare the following: Payment/services info: All authors have declared that no financial support was received from any organization for the submitted work. Financial relationships: Matthew Bechtold MD declare(s) personal fees from Medtrition. Advisory Board. Matthew Bechtold MD declare(s) personal fees from Nestle Nutrition Institute. Nutrition lectures. Other relationships: All authors have declared that there are no other relationships or activities that could appear to have influenced the submitted work.
Figures




Similar articles
-
Prophylactic Endotracheal Intubation in Patients with Upper Gastrointestinal Bleeding Undergoing Endoscopy: A Systematic Review and Meta-analysis.Saudi J Med Med Sci. 2017 Sep-Dec;5(3):201-209. doi: 10.4103/sjmms.sjmms_95_17. Epub 2017 Aug 21. Saudi J Med Med Sci. 2017. PMID: 30787790 Free PMC article. Review.
-
Endotracheal intubation for airway protection during endoscopy for severe upper GI hemorrhage.Gastrointest Endosc. 2003 Jan;57(1):58-61. doi: 10.1067/mge.2003.46. Gastrointest Endosc. 2003. PMID: 12518132
-
Prophylactic endotracheal intubation in critically ill patients with upper gastrointestinal bleed: A systematic review and meta-analysis.JGH Open. 2019 May 24;4(1):22-28. doi: 10.1002/jgh3.12195. eCollection 2020 Feb. JGH Open. 2019. PMID: 32055693 Free PMC article.
-
Prophylactic tracheal intubation for upper GI bleeding: A meta-analysis.World J Metaanal. 2015 Feb 26;3(1):4-10. doi: 10.13105/wjma.v3.i1.4. World J Metaanal. 2015. PMID: 25741509 Free PMC article.
-
Effectiveness of prophylactic antibacterial drugs for patients with liver cirrhosis and upper gastrointestinal bleeding: a systematic review and meta-analysis.Front Pharmacol. 2024 Mar 14;15:1324848. doi: 10.3389/fphar.2024.1324848. eCollection 2024. Front Pharmacol. 2024. PMID: 38549674 Free PMC article.
References
-
- Upper gastrointestinal bleeding: etiologies and management. Kamboj AK, Hoversten P, Leggett CL. Mayo Clin Proc. 2019;94:697–703. - PubMed
-
- Association of prophylactic endotracheal intubation in critically ill patients with upper GI bleeding and cardiopulmonary unplanned events. Hayat U, Lee PJ, Ullah H, Sarvepalli S, Lopez R, Vargo JJ. Gastrointest Endosc. 2017;86:500–509. - PubMed
-
- Anaesthesia care with and without tracheal intubation during emergency endoscopy for peptic ulcer bleeding: a population-based cohort study. Lohse N, Lundstrøm LH, Vestergaard TR, Risom M, Rosenstock SJ, Foss NB, Møller MH. Br J Anaesth. 2015;114:901–908. - PubMed
-
- Risk of aspiration pneumonia in suspected variceal hemorrhage: the value of prophylactic endotracheal intubation prior to endoscopy. Koch DG, Arguedas MR, Fallon MB. Dig Dis Sci. 2007;52:2225–2228. - PubMed
-
- Prophylactic endotracheal intubation prior to urgent endoscopy in patients with suspected variceal hemorrhage: an evaluation of outcomes and complications. Tang YM, Wang W. http://www.ghrnet.org/index.php/joghr/article/view/1968/2365 J Gastroenterol Hepatol Res. 2017;6:2324–2328.
Publication types
LinkOut - more resources
Full Text Sources
