Sex-based disparities in dopamine agonist response in patients with restless legs syndrome
- PMID: 39160111
- PMCID: PMC11911044
- DOI: 10.1111/jsr.14311
Sex-based disparities in dopamine agonist response in patients with restless legs syndrome
Abstract
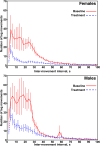
This study aimed to investigate sex-related differences in the response to ropinirole and pramipexole in patients with restless legs syndrome (RLS). By analysing clinical parameters and polysomnographic (PSG) findings, we sought to elucidate the potential factors related to sex disparities modulating treatment responses and sleep quality in RLS. A total of 41 drug-free patients with RLS, aged ≥18 years, underwent two consecutive nocturnal PSG recordings, without medication at baseline; before the second night, 26 patients received an oral dose of 0.25 mg pramipexole whereas 15 received 0.5 mg ropinirole. After each PSG recording, patients self-evaluated the severity of their previous night symptoms by means of an ad hoc visual analogue scale (VAS). At baseline, sleep efficiency and percentage of Stage N2 tended to be higher in females while wakefulness after sleep onset was significantly higher in males. After treatment, total leg movements during sleep (LMS), periodic LMS (PLMS), and periodicity indexes were significantly lower in females than in males. The VAS score was lower after treatment in all patients, without differences between the two sexes. This study demonstrates a higher acute responsiveness of PLMS to dopamine agonists (pramipexole and ropinirole) in females than in males with RLS. These findings might be explained by differential sex-related expression of dopamine receptors, especially D3, within the central nervous system. In addition, our findings provide translational hints toward a better tailored and sex-specific approach to the treatment of RLS associated with PLMS, with dopamine agonist possibly associated with a better outcome in females than in males.
Keywords: dopamine agonists; isolated leg movements during sleep; periodic leg movements during sleep; restless legs syndrome; sex.
© 2024 The Author(s). Journal of Sleep Research published by John Wiley & Sons Ltd on behalf of European Sleep Research Society.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
References
-
- Allen, R. P. , Picchietti, D. L. , Garcia‐Borreguero, D. , Ondo, W. G. , Walters, A. S. , Winkelman, J. W. , Zucconi, M. , Ferri, R. , Trenkwalder, C. , Lee, H. B. , & International Restless Legs Syndrome Study, Group . (2014). Restless legs syndrome/Willis–Ekbom disease diagnostic criteria: Updated international restless legs syndrome study group (IRLSSG) consensus criteria – history, rationale, description, and significance. Sleep Medicine, 15(8), 860–873. 10.1016/j.sleep.2014.03.025 - DOI - PubMed
-
- Bao, A.‐M. , & Swaab, D. F. (2010). Sex differences in the brain, behavior, and neuropsychiatric disorders. The Neuroscientist, 16(5), 550–565. - PubMed
-
- Bassetti, C. L. A. , Randerath, W. , Vignatelli, L. , Ferini‐Strambi, L. , Brill, A. K. , Bonsignore, M. R. , Grote, L. , Jennum, P. , Leys, D. , Minnerup, J. , Nobili, L. , Tonia, T. , Morgan, R. , Kerry, J. , Riha, R. , McNicholas, W. T. , & Papavasileiou, V. (2020). EAN/ERS/ESO/ESRS statement on the impact of sleep disorders on risk and outcome of stroke. The European Respiratory Journal, 55(4), 1901104. 10.1183/13993003.01104-2019 - DOI - PubMed