Changes in payer mix of new and established trauma centers: the new trauma center money grab?
- PMID: 39161373
- PMCID: PMC11331905
- DOI: 10.1136/tsaco-2024-001417
Changes in payer mix of new and established trauma centers: the new trauma center money grab?
Abstract
Background: Although timely access to trauma center (TC) care for injured patients is essential, the proliferation of new TCs does not always improve outcomes. Hospitals may seek TC accreditation for financial reasons, rather than to address community or geographic need. Introducing new TCs risks degrading case and payer mix at established TCs. We hypothesized that newly accredited TCs would see a disproportionate share of commercially insured patients.
Study design: We collected data from all accredited adult TCs in Pennsylvania using the state trauma registry from 1999 to 2018. As state policy regarding supplemental reimbursement for underinsured patients changed in 2004, we compared patient characteristics and payer mix between TCs established before and after 2004. We used multivariable logistic regression to assess the relationship between payer and presentation to a new versus established TC in recent years.
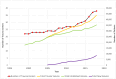
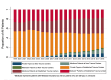
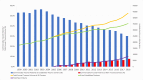
Results: Over time, there was a 40% increase in the number of TCs from 23 to 38. Of 326 204 patients from 2010 to 2018, a total of 43 621 (13.4%) were treated at 15 new TCs. New TCs treated more blunt trauma and less severely injured patients (p<0.001). In multivariable analysis, patients presenting to new TCs were more likely to have Medicare (OR 2.0, 95% CI 1.9 to 2.1) and commercial insurance (OR 1.6, 95% CI 1.5 to 1.6) compared with Medicaid. Over time, fewer patients at established TCs and more patients at new TCs had private insurance.
Conclusions: With the opening of new centers, payer mix changed unfavorably at established TCs. Trauma system development should consider community and regional needs, as well as impact on existing centers to ensure financial sustainability of TCs caring for vulnerable patients.
Level of evidence: Level III, prognostic/epidemiological.
Keywords: Health Care Economics And Organizations; Health Care Quality, Access, And Evaluation; health policy; insurance.
Copyright © Author(s) (or their employer(s)) 2024. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
None declared.
Figures
Comment in
-
Population need versus trauma center financial sustainability: striking the right balance.Trauma Surg Acute Care Open. 2024 Sep 5;9(1):e001540. doi: 10.1136/tsaco-2024-001540. eCollection 2024. Trauma Surg Acute Care Open. 2024. PMID: 39252755 Free PMC article. No abstract available.
References
-
- American College of Surgeons Committee on Trauma Putting the Pieces Together: A National Effort to Complete the U.S Trauma System. 2017. https://www.facs.org/quality-programs/trauma/systems/trauma-series/ Available.
-
- Hancock J. In alleged health care money grab, nation’s largest hospital chain cashes in on trauma centers. Kaiser health news 2021
LinkOut - more resources
Full Text Sources
Research Materials
