Assessing actigraphy performance for daytime sleep detection following stroke: insights from inpatient monitoring in a rehabilitation hospital
- PMID: 39161745
- PMCID: PMC11331150
- DOI: 10.1093/sleepadvances/zpae057
Assessing actigraphy performance for daytime sleep detection following stroke: insights from inpatient monitoring in a rehabilitation hospital
Abstract
Study objectives: Stroke can result in or exacerbate various sleep disorders. The presence of behaviors such as daytime sleepiness poststroke can indicate underlying sleep disorders which can significantly impact functional recovery and thus require prompt detection and monitoring for improved care. Actigraphy, a quantitative measurement technology, has been primarily validated for nighttime sleep in healthy adults; however, its validity for daytime sleep monitoring is currently unknown. Therefore this study aims to identify the best-performing actigraphy sensor and algorithm for detecting daytime sleep in poststroke individuals.
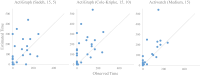
Methods: Participants wore Actiwatch Spectrum and ActiGraph wGT3X-BT on their less-affected wrist, while trained observers recorded daytime sleep occurrences and activity levels (active, sedentary, and asleep) during non-therapy times. Algorithms, Actiwatch (Autoscore AMRI) and ActiGraph (Cole-Kripke, Sadeh), were compared with on-site observations and assessed using F2 scores, emphasizing sensitivity to detect daytime sleep.
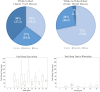
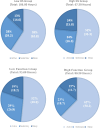
Results: Twenty-seven participants from an inpatient stroke rehabilitation unit contributed 173.5 hours of data. The ActiGraph Cole-Kripke algorithm (minute sleep time = 15 minutes, bedtime = 10 minutes, and wake time = 10 minutes) achieved the highest F2 score (0.59). Notably, when participants were in bed, the ActiGraph Cole-Kripke algorithm continued to outperform Sadeh and Actiwatch AMRI, with an F2 score of 0.69.
Conclusions: The study demonstrates both Actiwatch and ActiGraph's ability to detect daytime sleep, particularly during bed rest. ActiGraph (Cole-Kripke) algorithm exhibited a more balanced sleep detection profile and higher F2 scores compared to Actiwatch, offering valuable insights for optimizing daytime sleep monitoring with actigraphy in stroke patients.
Keywords: Inpatient Rehabilitation Hospital; actigraphy; napping; stroke.
© The Author(s) 2024. Published by Oxford University Press on behalf of Sleep Research Society.
Figures
Similar articles
-
Actigraphy-based sleep estimation in adolescents and adults: a comparison with polysomnography using two scoring algorithms.Nat Sci Sleep. 2018 Jan 18;10:13-20. doi: 10.2147/NSS.S151085. eCollection 2018. Nat Sci Sleep. 2018. PMID: 29403321 Free PMC article.
-
Performance comparison of different interpretative algorithms utilized to derive sleep parameters from wrist actigraphy data.Chronobiol Int. 2019 Dec;36(12):1752-1760. doi: 10.1080/07420528.2019.1679826. Epub 2019 Oct 28. Chronobiol Int. 2019. PMID: 31658822
-
The convergent validity of Actiwatch 2 and ActiGraph Link accelerometers in measuring total sleeping period, wake after sleep onset, and sleep efficiency in free-living condition.Sleep Breath. 2017 Mar;21(1):209-215. doi: 10.1007/s11325-016-1406-0. Epub 2016 Sep 10. Sleep Breath. 2017. PMID: 27614441
-
Comparison of sleep parameters from wrist-worn ActiGraph and Actiwatch devices.Sleep. 2024 Feb 8;47(2):zsad155. doi: 10.1093/sleep/zsad155. Sleep. 2024. PMID: 37257489 Free PMC article.
-
Actigraphy-Based Sleep Detection: Validation with Polysomnography and Comparison of Performance for Nighttime and Daytime Sleep During Simulated Shift Work.Nat Sci Sleep. 2022 Oct 14;14:1801-1816. doi: 10.2147/NSS.S373107. eCollection 2022. Nat Sci Sleep. 2022. PMID: 36275180 Free PMC article.
References
-
- Bogan RK. Effects of restless legs syndrome (RLS) on sleep. Neuropsychiatr Dis Treat. 2006;2(4):513–519. doi: 10.2147/nedt.2006.2.4.513. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2671944/. Accessed June 12, 2024. - DOI - PMC - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

