Respiratory Viral Infections From 2015 to 2022 in the HIVE Cohort of American Households: Incidence, Illness Characteristics, and Seasonality
- PMID: 39179953
- PMCID: PMC11847950
- DOI: 10.1093/infdis/jiae423
Respiratory Viral Infections From 2015 to 2022 in the HIVE Cohort of American Households: Incidence, Illness Characteristics, and Seasonality
Abstract
Background: Viral respiratory illnesses are the most common acute illnesses experienced and generally follow a predicted pattern over time. The severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) pandemic interrupted that pattern.
Methods: The HIVE (Household Influenza Vaccine Evaluation) study was established in 2010 to follow a cohort of Southeast Michigan households over time. Initially focused on influenza, surveillance was expanded to include other major respiratory pathogens, and, starting in 2015, the population was followed year round. Symptoms of acute illness were reported, and respiratory specimens were collected and tested to identify viral infections. Based on the known population being followed, virus-specific incidence was calculated.
Results: From 2015 to 2022, 1755 participants were followed in HIVE for 7785 person-years with 7833 illnesses documented. Before the pandemic, rhinovirus (RV) and common cold human coronaviruses (HCoVs) were the viruses most frequently identified, and incidence decreased with increasing age. Type A influenza was next but with comparable incidence by age. Parainfluenza and respiratory syncytial viruses were less frequent overall, followed by human metapneumoviruses. Incidence was highest in young children, but infections were frequently documented in all age groups. Seasonality followed patterns established decades ago. The SARS-CoV-2 pandemic disrupted these patterns, except for RV and, to a lesser extent, HCoVs. In the first 2 years of the pandemic, RV incidence far exceeded that of SARS-CoV-2.
Conclusions: Longitudinal cohort studies are important in comparing the incidence, seasonality, and characteristics of different respiratory viral infections. Studies documented the differential effect of the pandemic on the incidence of respiratory viruses in addition to SARS-CoV-2.
Keywords: SARS-CoV-2; cohort studies; coronaviruses; influenza; respiratory infections.
Published by Oxford University Press on behalf of Infectious Diseases Society of America 2024.
Conflict of interest statement
Potential conflicts of interest. All authors: No reported conflicts of interest. All authors have submitted the ICMJE Form for Disclosure of Potential Conflicts of Interest. Conflicts that the editors consider relevant to the content of the manuscript have been disclosed.
Figures
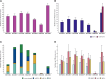

References
-
- Dingle JH, Badger GF, Feller AE, Hodges RG, Jordan WS, Rammelkamp CH. A study of illness in a group of Cleveland families. I. Plan of study and certain general observations. Am J Hyg 1953; 58:16–30. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

