Multivariate analysis of factors associated with the successful prediction of initial blind placement of a nasointestinal tube in the stomach based on X-ray imaging: a retrospective, single-center study
- PMID: 39179985
- PMCID: PMC11342475
- DOI: 10.1186/s12876-024-03363-z
Multivariate analysis of factors associated with the successful prediction of initial blind placement of a nasointestinal tube in the stomach based on X-ray imaging: a retrospective, single-center study
Abstract
Background: Patients in the intensive care unit (ICU) are highly susceptible to malnutrition, and while enteral nutrition via nasogastric tube is the preferred method, there is a risk of inadvertent reflux and aspiration. Therefore, clinicians have turned to nasointestinal tubes (NET) for enteral nutrition as an alternative option. But the precise localization of NET presents an ongoing challenge. We proposed an innovative approach to provide a valuable reference for clinicians involved in NET placement.
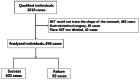
Method: Data were obtained retrospectively from the medical records of adult patients with a high risk of aspiration or gastric feeding intolerance who had a NET placed in the ICU of Zhejiang Provincial People's Hospital between October 1, 2017, and October 1, 2023. The collected data were subjected to statistical analysis using SPSS and R software.
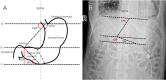
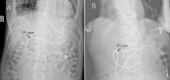
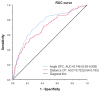
Result: There were 494 patients who met the inclusion and exclusion criteria. The first-pass success rate was 81.4% (n = 402). The success of a patient's initial NET placement was found to be associated with Angle SPC and Distance CP, as determined by univariate analysis (25.6 ± 16.7° vs. 41.9 ± 18.0°, P < 0.001; 40.0 ± 26.2 mm vs. 62.0 ± 31.8 mm, P < 0.001, respectively). By conducting a multivariate regression analysis, we identified a significant association between pyloric types and the success rate of placing NET (OR 29.559, 95%CI 14.084-62.038, P < 0.001).
Conclusion: Angle SPC, Distance CP, and the type of pylorus are independently associated with successful initial placement of NET. Besides, patients with the outside type of pylorus (OP-type) exhibit a higher rate of initial placement success.
Keywords: Blind placement; Intensive care unit; Nasointestinal tube; Post-pyloric feeding.
© 2024. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures

References
-
- Mundi MS, Patel JJ, Martindale R. Body composition technology: implications for the ICU. NUTR CLIN PRACT. 2019;34(1):48–58. - PubMed
-
- Vavruk AM, Martins C, Mazza DNM. Validation of Malnutrition clinical characteristics in critically ill patients. NUTR CLIN PRACT. 2021;36(5):993–1002. - PubMed
-
- Gramlich L, Kichian K, Pinilla J, Rodych NJ, Dhaliwal R, Heyland DK. Does enteral nutrition compared to parenteral nutrition result in better outcomes in critically ill adult patients? A systematic review of the literature. NUTRITION. 2004;20(10):843–8. - PubMed
-
- Peter JV, Moran JL, Phillips-Hughes J. A metaanalysis of treatment outcomes of early enteral versus early parenteral nutrition in hospitalized patients. CRIT CARE MED. 2005;33(1):213–20. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

