Impact of a 'Catheter Bundle' on Infection Rates and Economic Costs in the Intensive Care Unit: A Retrospective Cohort Study
- PMID: 39189275
- PMCID: PMC11348204
- DOI: 10.3390/nursrep14030145
Impact of a 'Catheter Bundle' on Infection Rates and Economic Costs in the Intensive Care Unit: A Retrospective Cohort Study
Abstract
Introduction: Catheter-related infections (CBRSIs) are a widespread problem that increase morbidity and mortality in intensive care unit (ICU) patients and management costs.
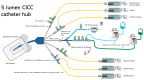
Objective: The main aim of this study was to assess the prevalence of CBRSIs in an intensive care unit following international literature guidelines for managing vascular lines in critically ill patients. These guidelines include changing vascular lines every 7 days, using needle-free devices and port protectors, standardising closed infusion lines, employing chlorhexidine-impregnated dressings, and utilising sutureless devices for catheter securement.
Materials and methods: This single-centre retrospective observational study was conducted in a general Italian ICU. This study included all eligible patients aged > 1 year who were admitted between January 2018 and December 2022.
Results: During the study period, 1240 patients were enrolled, of whom 9 were diagnosed with a CRBSI. The infection rate per 1000 catheters/day was as follows: femorally inserted central catheter, 1.04; centrally inserted central catheter, 0.77; pulmonary arterial catheter 0.71, arterial catheter, 0.1; and peripherally inserted central catheter and continuous veno-venous haemodialysis dialysis catheters equal to 0. No difference in CRBSI was observed between the years included in the study (p = 0.874). The multivariate analysis showed an association between the diagnosis of CBRSI and Nursing Activities Score (per single point increase β = 0.04-95%CI: -0.01-0.09, p = 0.048), reason for ICU admission-trauma (β = 0.77-95%CI: -0.03-1.49, p = 0.039), and use of therapeutic hypothermia (β = 2.06, 95%CI: 0.51-3.20, p < 0.001). Implementing the study protocol revealed a cost of EUR 130.00/patient, equivalent to a daily cost of EUR 15.20 per patient.
Conclusions: This study highlights the importance of implementing a catheter care bundle to minimise the risk of CRBSI and the associated costs in the ICU setting. A policy change for infusion set replacement every 7 days has helped to maintain the CRBSI rate below the recommended rate, resulting in significant cost reduction and reduced production of ICU waste.
Keywords: CLABSI; CRBSI; bundle; infection prevention; needle-free; port protector.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
References
-
- Buetti N., Marschall J., Drees M., Fakih M.G., Hadaway L., Maragakis L.L., Monsees E., Novosad S., O’Grady N.P., Rupp M.E., et al. Strategies to Prevent Central Line-Associated Bloodstream Infections in Acute-Care Hospitals: 2022 Update. Infect. Control Hosp. Epidemiol. 2022;43:553–569. doi: 10.1017/ice.2022.87. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources