Beyond Clinical Examination: Utilizing MRI Surveillance to Detect Recurrence of Soft Tissue Sarcomas and Differentiate from Posttherapeutic Changes
- PMID: 39200105
- PMCID: PMC11351765
- DOI: 10.3390/biomedicines12081640
Beyond Clinical Examination: Utilizing MRI Surveillance to Detect Recurrence of Soft Tissue Sarcomas and Differentiate from Posttherapeutic Changes
Abstract
Background: Early detection of soft tissue sarcoma (STS) recurrence is essential; however, the role and timeline of Magnetic resonance imaging (MRI) surveillance are still under debate. The aim of this study was to determine whether local recurrence (LR) could be identified via clinical examination alone and to assess the MRI morphology of primary STS and LR.
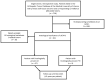
Methods: This retrospective study included all patients with STS recurrence after surveillance for at least five years from the tumor database of the Medical University of Vienna from 2000 until December 2023. The characteristics of primary STS and LR and the time interval to recurrence and clinical detectability were assessed. The MRIs of LR and posttherapeutic changes (PTC) were compared with the initial MRIs.
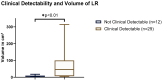
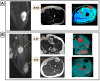
Results: A total of 57 patients (60% male; mean age 58.5 ± 18.0 years) with STS and histologically confirmed LR were included. The mean time interval to LR was 2.3 ± 1.8 years (range 108 to 3037 days). The clinically detectable recurrences were significantly larger than the inapparent ones (71.9 cm3 vs. 7.0 cm3; p < 0.01). The MRI morphology of all LRs (26/26) closely resembled the initial STS. For comparison, nine patients were included with clinically suspected LRs, which were histologically proven to be PTC. None of these resembled the primary STS.
Conclusion: Based on clinical symptoms alone, especially small and early recurrences can be missed, which supports the importance of MRI surveillance.
Keywords: locoregional neoplasm recurrence; magnetic resonance imaging; sarcoma; soft tissue neoplasms; surveillance.
Conflict of interest statement
The Department of Biomedical Imaging and Image-guided Therapy of Medical University of Vienna has grants/grants pending and contracts with more than 100 partners (organizational, academic, industry), independent of this study and all through official contracts with the Medical University of Vienna. However, this study has not received any funding. Felix R. M. Koenig—nothing to disclose. Alfred H. Kielburg—nothing to disclose. Snehansh Roy Chaudhary—nothing to disclose. Akash Ganguly—nothing to disclose. Christian Wassipaul—nothing to disclose. Raoul Varga—nothing to disclose. Martin L. Watzenboeck—nothing to disclose. Iris-M. Noebauer-Huhmann—nothing to disclose.
Figures

Similar articles
-
Can we use MRI to detect clinically silent recurrent soft-tissue sarcoma?Eur Radiol. 2020 Sep;30(9):4724-4733. doi: 10.1007/s00330-020-06810-z. Epub 2020 Apr 20. Eur Radiol. 2020. PMID: 32314057
-
MRI surveillance for local recurrence in extremity soft tissue sarcoma.Eur J Surg Oncol. 2019 Feb;45(2):268-274. doi: 10.1016/j.ejso.2018.08.032. Epub 2018 Oct 16. Eur J Surg Oncol. 2019. PMID: 30352764
-
Linear mixed-effects models for predicting sarcoma local recurrence growth rates: Implications for optimal surveillance imaging frequency.Eur J Radiol. 2020 Nov;132:109308. doi: 10.1016/j.ejrad.2020.109308. Epub 2020 Sep 28. Eur J Radiol. 2020. PMID: 33010684 Free PMC article.
-
Imaging update on soft tissue sarcoma.J Clin Orthop Trauma. 2021 Aug 20;22:101568. doi: 10.1016/j.jcot.2021.101568. eCollection 2021 Nov. J Clin Orthop Trauma. 2021. PMID: 34567971 Free PMC article. Review.
-
Treating soft tissue sarcomas with adjuvant chemotherapy.Curr Treat Options Oncol. 2011 Mar;12(1):21-31. doi: 10.1007/s11864-011-0145-5. Curr Treat Options Oncol. 2011. PMID: 21384115 Review.
Cited by
-
Soft tissue tumor imaging in adults: European Society of Musculoskeletal Radiology-Guidelines 2024: imaging immediately after neoadjuvant therapy in soft tissue sarcoma, soft tissue tumor surveillance, and the role of interventional radiology.Eur Radiol. 2025 Jun;35(6):3324-3335. doi: 10.1007/s00330-024-11242-0. Epub 2024 Dec 18. Eur Radiol. 2025. PMID: 39694887 Free PMC article.
References
LinkOut - more resources
Full Text Sources

