Moving beyond Symptom Criteria to Diagnose and Treat Functional Disorders: Patient-Reported Symptoms of Functional Lower Gastrointestinal Disorders Correlate Poorly with Objective Assessment of Luminal Contents Seen on Intestinal Ultrasound
- PMID: 39200901
- PMCID: PMC11355646
- DOI: 10.3390/jcm13164759
Moving beyond Symptom Criteria to Diagnose and Treat Functional Disorders: Patient-Reported Symptoms of Functional Lower Gastrointestinal Disorders Correlate Poorly with Objective Assessment of Luminal Contents Seen on Intestinal Ultrasound
Abstract
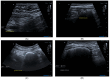
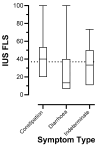
Background/Objectives: The diagnosis of lower functional gastrointestinal disorders (FGIDs) is currently based on subjective and unreliable patient-reported symptoms, with significant clinical overlap between diagnosed phenotypes. Objective biomarkers are urgently sought. Gastrointestinal ultrasound (GIUS) can objectively and non-invasively assess luminal contents. This study aimed to assess the utility of GIUS in phenotyping patients with lower FGIDs. Methods: Patients with lower FGIDs underwent a GIUS and completed the Rome IV Diagnostic Questionnaire, SAGIS questionnaire, and 100 mm VAS score for overall symptom severity. The faecal loading score (FLS) was obtained using a modified Leech score, where an FLS of >37 was consistent with clinically significant constipation. Results: Eighty-eight patients fulfilled the study requirements. In total, 56 met the Rome IV criteria for irritable bowel syndrome (IBS) subtypes, while 23 met the criteria for functional constipation (FC), 4 for functional diarrhoea (FD), and 5 for other diagnoses. Patients reporting constipation-predominant symptoms had a significantly higher median FLS than those describing diarrhoea-predominant symptoms (FLS = 40 [IQR 20.0-53.3] vs. 13.3 [IQR 6.7-40.0], respectively). However, 27% of patients describing diarrhoea had significant faecal loading on GIUS, and of those who described constipation, 34% did not have significant faecal loading. Sensitivity and specificity for the detection of FLS-indicated constipation by the Rome IV criteria were low at 59% and 66%, respectively. Conclusions: The symptom-based diagnosis of FGID subtypes based on the Rome IV criteria is a poor predictor of faecal loading. These findings should prompt further exploration of the limitations of symptom-based assessment and a shift towards physiological assessment of patients with FGIDs such as gastrointestinal ultrasound to develop more targeted therapy. Future research is underway to determine if targeting objective physiological endpoints results in improved clinical outcomes.
Keywords: disorder of brain–gut interaction; functional gastrointestinal disorder; intestinal ultrasound; irritable bowel syndrome.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures

References
LinkOut - more resources
Full Text Sources
Miscellaneous

