Eosinophilic Bronchiectasis: Prevalence, Severity, and Associated Features-A Cohort Study
- PMID: 39201075
- PMCID: PMC11355134
- DOI: 10.3390/jcm13164932
Eosinophilic Bronchiectasis: Prevalence, Severity, and Associated Features-A Cohort Study
Abstract
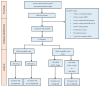
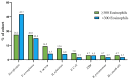
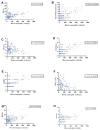
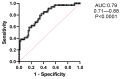
Background: Bronchiectasis (BE) has been traditionally associated with neutrophilic inflammation, but eosinophilic bronchiectasis (EB) has recently emerged. Data about prevalence, clinical features, and disease severity are lacking. This study aimed to assess the EB prevalence, compare EB with non-EB, evaluate the Type-2 (T2) high endotype in BE (T2-high EB) versus non-T2-high EB, and identify EB predictors. Methods: We conducted a prospective study involving 153 BE patients. The data collected included clinical, radiological, and microbiological findings. BE severity was assessed using the bronchiectasis severity index (BSI), FACED and E-FACED scores, and the bronchiectasis etiology and comorbidity index (BACI). EB was defined as a blood eosinophil count (BEC) ≥ 300 cells/μL, and T2-high EB as BEC ≥ 300 cells/μL with fractional exhaled nitric oxide (FeNO) ≥ 25 ppb. Results: Prevalence was 27% for EB and 20% for T2-high EB. EB patients exhibited poorer lung function and more severe radiologic features, with significantly higher severity scores [BSI, FACED, E-FACED, BACI (p < 0.05)], and a higher median exacerbation rate [4 (2-5) in EB vs. 2 (1-4) in non-EB, p = 0.0002], compared with non-EB patients. T2-high EB patients showed higher severity scores [BSI, FACED, E-FACED (p < 0.05)], as well as worse lung function parameters [FEV1%, FVC%, FEF 25-75% (p < 0.05)] compared with non-T2-high EB patients. In our study, patients with EB exhibited notably worsened lung function and higher BE severity scores compared with their non-EB counterparts, with exacerbations playing a major role in these differences. We found statistically significant positive correlations between BEC and disease severity scores, such as BSI, FACED, and mMRC, as well as an inverse relationship with pulmonary function. The likelihood of EB being present was significantly higher in association with mMRC ≥ 1 (OR = 2.53; 95% CI, 1.26-5.64), exacerbations/year ≥ 1 (OR = 1.27; 95% CI, 1.0-1.63), and chronic PA colonization (OR = 3.9; 95% CI, 1.08-15.8). Conclusions: EB is a distinct endotype. Dyspnea, exacerbations, and PA colonization may be predictive of EB, emphasizing the importance of early detection for improved outcomes. BEC could serve as a useful biomarker of disease severity to consider when diagnosing EB.
Keywords: Type 2 (T2) inflammation; bronchiectasis; eosinophil; exacerbations.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Similar articles
-
Simultaneous evaluation of the fractional exhaled nitric oxide and blood eosinophil count of T2-high endotype in patients with non-cystic fibrosis bronchiectasis.Chron Respir Dis. 2023 Jan-Dec;20:14799731231210559. doi: 10.1177/14799731231210559. Chron Respir Dis. 2023. PMID: 37889184 Free PMC article.
-
Type 2 Biomarkers and Their Clinical Implications in Bronchiectasis: A Prospective Cohort Study.Lung. 2024 Oct;202(5):695-709. doi: 10.1007/s00408-024-00707-0. Epub 2024 Jun 17. Lung. 2024. PMID: 38884647 Free PMC article.
-
Elevated Eosinophil Counts in Acute Exacerbations of Bronchiectasis: Unveiling a Distinct Clinical Phenotype.Lung. 2024 Feb;202(1):53-61. doi: 10.1007/s00408-023-00668-w. Epub 2024 Jan 16. Lung. 2024. PMID: 38228883 Free PMC article.
-
Prognostic performance of the FACED score and bronchiectasis severity index in bronchiectasis: a systematic review and meta-analysis.Biosci Rep. 2020 Oct 30;40(10):BSR20194514. doi: 10.1042/BSR20194514. Biosci Rep. 2020. PMID: 33057706 Free PMC article.
-
Assessing effects of inhaled antibiotics in adults with non-cystic fibrosis bronchiectasis--experiences from recent clinical trials.Expert Rev Respir Med. 2018 Sep;12(9):769-782. doi: 10.1080/17476348.2018.1503540. Epub 2018 Aug 3. Expert Rev Respir Med. 2018. PMID: 30025482 Review.
Cited by
-
Hypereosinophilic Syndrome in a Patient With Cystic Fibrosis: A Rare Case of Cardiac Involvement and Response to Mepolizumab.Cureus. 2025 Jul 4;17(7):e87264. doi: 10.7759/cureus.87264. eCollection 2025 Jul. Cureus. 2025. PMID: 40755600 Free PMC article.
-
Innovating Respiratory Diagnostics: The Game-Changing Role of Biomarkers.J Clin Med. 2024 Sep 30;13(19):5850. doi: 10.3390/jcm13195850. J Clin Med. 2024. PMID: 39407909 Free PMC article.
-
The role of T-helper and T regulatory cells in driving neutrophilic and eosinophilic inflammation in bronchiectasis.Front Immunol. 2025 Jun 16;16:1598257. doi: 10.3389/fimmu.2025.1598257. eCollection 2025. Front Immunol. 2025. PMID: 40589741 Free PMC article. Review.
References
-
- Polverino E., Goeminne P.C., McDonnell M.J., Aliberti S., Marshall S.E., Loebinger M.R., Murris M., Cantón R., Torres A., Dimakou K., et al. European Respiratory Society guidelines for the management of adult bronchiectasis. Eur. Respir. J. 2017;50:1700629. doi: 10.1183/13993003.00629-2017. - DOI - PubMed
-
- Tsikrika S., Dimakou K., Papaioannou A.I., Hillas G., Thanos L., Kostikas K., Loukides S., Papiris S., Koulouris N., Bakakos P. The role of non-invasive modalities for assessing inflammation in patients with non-cystic fibrosis bronchiectasis. Cytokine. 2017;99:281–286. doi: 10.1016/j.cyto.2017.08.005. - DOI - PubMed
LinkOut - more resources
Full Text Sources

