A Comparison of Norepinephrine versus Phenylephrine to Prevent Hypotension after Spinal Anesthesia for Cesarean Section: Systematic Review and Meta-Analysis
- PMID: 39201995
- PMCID: PMC11355940
- DOI: 10.3390/jpm14080803
A Comparison of Norepinephrine versus Phenylephrine to Prevent Hypotension after Spinal Anesthesia for Cesarean Section: Systematic Review and Meta-Analysis
Abstract
Background: This systematic review and meta-analysis aimed to compare the effects of using phenylephrine or norepinephrine on the pH and base excess (BE) of the umbilical artery and vein in parturients undergoing cesarean section.
Methods: The study protocol was registered in INPLASY. Independent researchers searched Ovid-Medline, Ovid-EMBASE, and Cochrane Central Register of Controlled Trials (CENTRAL) databases and Google Scholar for relevant randomized controlled trials (RCTs). The primary outcome of this study was the umbilical artery (UA) or umbilical vein (UV) pH as neonatal condition at birth, and the secondary outcome was the UA or UV BE as an additional prognostic value over the measurement of umbilical pH.
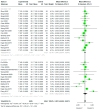
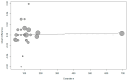
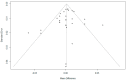
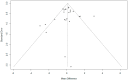
Results: There was no evidence of a difference between phenylephrine and norepinephrine for overall, UA, and UV pH (mean difference (MD) -0.001, 95% confidence interval (CI) -0.004 to 0.007; MD 0.000, 95%CI -0.004 to 0.004; and MD 0.002, 95%CI -0.013 to 0.017). There was also no evidence of a difference between phenylephrine and norepinephrine for overall, UA, and UV BE (MD 0.096, 95% CI -0.258 to 0.451; MD 0.076, 95%CI -0.141 to 0.294; and MD 0.121, 95%CI; -0.569 to 0.811). A meta-regression showed that factors such as umbilical artery or vein, infusion method, single or twin, and the number of parturients per study had no effect on the UA pH, UV pH, UA BE, or UV BE. No evidence of publication bias was detected.
Conclusions: There was no evidence of a difference between phenylephrine and norepinephrine for umbilical pH and BE. A subgroup analysis and meta-regression also did not show evidence of differences.
Keywords: anesthesia; cesarean section; hypotension; meta-analysis; norepinephrine; phenylephrine; spinal; vasoconstrictor agents.
Conflict of interest statement
No potential conflicts of interest relevant to this article were reported.
Figures



References
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources

