Mild Phenotypes of Gyrate Atrophy in a Heterozygous Carrier with One Variant Allele of OAT
- PMID: 39202380
- PMCID: PMC11353755
- DOI: 10.3390/genes15081020
Mild Phenotypes of Gyrate Atrophy in a Heterozygous Carrier with One Variant Allele of OAT
Abstract
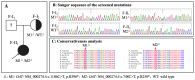
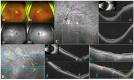
This study aimed to identify whether gyrate atrophy of the choroid and retina (GACR) heterozygous individuals have possible clinical manifestations and to explore the potential pathogenic mechanism. In this retrospective study, we surveyed a two-generation pedigree of an individual diagnosed with GACR. Two family members underwent ophthalmological, hematologic, and genetic tests. An arginine-restricted diet with vitamin B6 supplementation was implemented; clinical assessments were repeated every 3 months during follow-up. The relative OAT mRNA expression was determined using a real-time quantitative polymerase chain reaction. The 19-year-old compound heterozygous daughter (OAT: c.1186C>T; c.748C>T) had bilateral pathologic myopia, posterior staphyloma, chorioretinal atrophy, macular abnormalities, and elevated hematologic ornithine. The 54-year-old heterozygous mother (OAT: c.1186C>T) presented with bilateral pathologic myopia, asymmetric posterior staphyloma, retina and choroidal capillary layer atrophy, retinal pigment epithelium abnormalities, and mildly elevated hematologic ornithine. Compared to normal individuals, the daughter and mother had 29% and 46% relative OAT mRNA expression, respectively (p < 0.001). We believe that this is the first report of a carrier of one OAT variant allele exhibiting a mild phenotype, suggesting that family members should be aware of the possibility of clinical involvement in carriers with some autosomal recessive conditions. Additional data suggest that nonsense-mediated, decay-initiated mRNA degradation may cause GACR.
Keywords: OAT gene; allele; autosomal recessive; carrier; gyrate atrophy of the choroid and retina (GACR).
Conflict of interest statement
The authors declare no conflicts of interest.
Figures


Similar articles
-
Diagnostic value of a combination of next-generation sequencing, chorioretinal imaging and metabolic analysis: lessons from a consanguineous Chinese family with gyrate atrophy of the choroid and retina stemming from a novel OAT variant.Br J Ophthalmol. 2019 Mar;103(3):428-435. doi: 10.1136/bjophthalmol-2018-312347. Epub 2018 Oct 26. Br J Ophthalmol. 2019. PMID: 30366948
-
Variable phenotypes of gyrate atrophy in siblings with a nonsense mutation in OAT gene.Ophthalmic Genet. 2021 Jun;42(3):300-303. doi: 10.1080/13816810.2020.1870149. Epub 2021 Jan 19. Ophthalmic Genet. 2021. PMID: 33463379
-
Inheritance of ornithine aminotransferase gene, mRNA, and enzyme defect in a family with gyrate atrophy of the choroid and retina.Am J Hum Genet. 1989 Mar;44(3):353-7. Am J Hum Genet. 1989. PMID: 2916581 Free PMC article.
-
Ocular Tissue-Specific Amino Acid Metabolism in Gyrate Atrophy.Adv Exp Med Biol. 2025;1468:279-284. doi: 10.1007/978-3-031-76550-6_46. Adv Exp Med Biol. 2025. PMID: 39930209 Free PMC article. Review.
-
Deficit of human ornithine aminotransferase in gyrate atrophy: Molecular, cellular, and clinical aspects.Biochim Biophys Acta Proteins Proteom. 2021 Jan;1869(1):140555. doi: 10.1016/j.bbapap.2020.140555. Epub 2020 Oct 14. Biochim Biophys Acta Proteins Proteom. 2021. PMID: 33068755 Review.
References
-
- Montioli R., Bellezza I., Desbats M.A., Borri Voltattorni C., Salviati L., Cellini B. Deficit of human ornithine aminotransferase in gyrate atrophy: Molecular, cellular, and clinical aspects. Biochim. Biophys. Acta. Proteins Proteom. 2021;1869:140555. doi: 10.1016/j.bbapap.2020.140555. - DOI - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

