Fertility preserving techniques in neuro-oncology patients: A systematic review
- PMID: 39220246
- PMCID: PMC11364935
- DOI: 10.1093/noajnl/vdae124
Fertility preserving techniques in neuro-oncology patients: A systematic review
Abstract
Background: Advancements in cancer treatments have enhanced survival rates and quality of life for patients with central nervous system (CNS) tumors. There is growing recognition of the significance of fertility preservation methods. Currently, techniques, including oocyte cryopreservation and sperm cryopreservation are established. Nevertheless, oncologists may exhibit reluctance when referring patients to reproductive specialists. This review aimed to assess the best evidence for fertility preservation techniques used in patients with CNS cancers and evaluate outcomes relating to their success and complications.
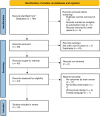
Methods: Two reviewers performed a search of Pubmed, Embase, Medline, Cochrane, and Google Scholar. Papers were included if they reported at least 1 fertility preservation technique in a neuro-oncology patient. Non-English studies, editorials, animal studies, and guidelines were excluded. Meta-analysis was performed using the random effects model.
Results: Sixteen studies containing data from 237 participants (78.8% female) were included in the systematic review and meta-analysis, of whom 110 (46.4%) underwent fertility preservation techniques. All patients (100%) successfully underwent fertility preservation with 1 participant (2.9%) returning to rewarm their oocytes, embryos or sperm. On average, 17.8 oocytes were retrieved with 78%, ultimately being cryopreserved. Five (6.0%) patients successfully conceived 9 healthy-term children after utilizing their cryopreserved sperm, embryos, or oocytes. Moreover, 6 patients successfully conceived naturally or using intrauterine insemination, resulting in 7 healthy-term children.
Conclusions: Fertility preservation techniques could offer a safe and effective way for neuro-oncology patients to deliver healthy-term babies following treatment. However, further studies concerning risks, long-term pregnancy outcomes, and cost-effectiveness are needed.
Keywords: embryo cryopreservation; fertility preservation; neuro-oncology; oocyte cryopreservation; ovarian tissue transposition.
© The Author(s) 2024. Published by Oxford University Press, the Society for Neuro-Oncology and the European Association of Neuro-Oncology.
Conflict of interest statement
The authors have no relevant financial or nonfinancial interests to disclose.
Figures




Similar articles
-
Fertility Preservation Techniques in Neuro-Oncology Patients: Protocol for a Systematic Review.JMIR Res Protoc. 2023 May 8;12:e44825. doi: 10.2196/44825. JMIR Res Protoc. 2023. PMID: 37155238 Free PMC article.
-
Live birth rate after female fertility preservation for cancer or haematopoietic stem cell transplantation: a systematic review and meta-analysis of the three main techniques; embryo, oocyte and ovarian tissue cryopreservation.Hum Reprod. 2023 Mar 1;38(3):489-502. doi: 10.1093/humrep/deac249. Hum Reprod. 2023. PMID: 36421038 Free PMC article.
-
Fertility preservation in adult male patients with cancer: a systematic review and meta-analysis.Hum Reprod Open. 2024 Jan 30;2024(1):hoae006. doi: 10.1093/hropen/hoae006. eCollection 2024. Hum Reprod Open. 2024. PMID: 38389980 Free PMC article. Review.
-
A comparison of fertility preservation outcomes in patients who froze oocytes, embryos, or ovarian tissue for medically indicated circumstances: a systematic review and meta-analysis.Fertil Steril. 2022 Jun;117(6):1266-1276. doi: 10.1016/j.fertnstert.2022.03.004. Epub 2022 Apr 19. Fertil Steril. 2022. PMID: 35459522
-
Ovarian stimulation for fertility preservation in women with cancer: A systematic review and meta-analysis comparing random and conventional starts.J Gynecol Obstet Hum Reprod. 2021 Oct;50(8):102080. doi: 10.1016/j.jogoh.2021.102080. Epub 2021 Feb 2. J Gynecol Obstet Hum Reprod. 2021. PMID: 33545413
Cited by
-
Comprehensive Fertility Management After Pituitary Adenoma Surgery: Lessons from a Rural Japanese Case and Practical Review.Reports (MDPI). 2025 Aug 15;8(3):144. doi: 10.3390/reports8030144. Reports (MDPI). 2025. PMID: 40843886 Free PMC article.
References
-
- Siegel RL, Miller KD, Jemal A.. Cancer statistics, 2018. CA Cancer J Clin. 2018;68(1):7–30. - PubMed
-
- Anderson RA, Wallace WHB.. Antimüllerian hormone, the assessment of the ovarian reserve, and the reproductive outcome of the young patient with cancer. Fertil Steril. 2013;99(6):1469–1475. - PubMed
-
- Meirow D, Biederman H, Anderson RA, Wallace WHB.. Toxicity of chemotherapy and radiation on female reproduction. Clin Obstet Gynecol. 2010;53(4):727–739. - PubMed
LinkOut - more resources
Full Text Sources
