Engineering of Bioresorbable Polymers for Tissue Engineering and Drug Delivery Applications
- PMID: 39233521
- PMCID: PMC11616265
- DOI: 10.1002/adhm.202401674
Engineering of Bioresorbable Polymers for Tissue Engineering and Drug Delivery Applications
Abstract
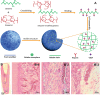
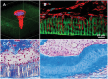
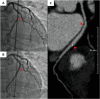
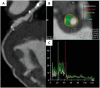
Herein, the recent advances in the development of resorbable polymeric-based biomaterials, their geometrical forms, resorption mechanisms, and their capabilities in various biomedical applications are critically reviewed. A comprehensive discussion of the engineering approaches for the fabrication of polymeric resorbable scaffolds for tissue engineering, drug delivery, surgical, cardiological, aesthetical, dental and cardiovascular applications, are also explained. Furthermore, to understand the internal structures of resorbable scaffolds, representative studies of their evaluation by medical imaging techniques, e.g., cardiac computer tomography, are succinctly highlighted. This approach provides crucial clinical insights which help to improve the materials' suitable and viable characteristics for them to meet the highly restrictive medical requirements. Finally, the aspects of the legal regulations and the associated challenges in translating research into desirable clinical and marketable materials of polymeric-based formulations, are presented.
Keywords: clinical challenges; drug delivery; implants; medical imaging; polymer matrices; resorbable biomaterials; tissue engineering.
© 2024 The Author(s). Advanced Healthcare Materials published by Wiley‐VCH GmbH.
Conflict of interest statement
The authors declare no conflict of interest.
Figures







Similar articles
-
Conductive Polymeric-Based Electroactive Scaffolds for Tissue Engineering Applications: Current Progress and Challenges from Biomaterials and Manufacturing Perspectives.Int J Mol Sci. 2021 Oct 26;22(21):11543. doi: 10.3390/ijms222111543. Int J Mol Sci. 2021. PMID: 34768972 Free PMC article. Review.
-
Glycosaminoglycan-based resorbable polymer composites in tissue refurbishment.Regen Med. 2017 Apr;12(4):431-457. doi: 10.2217/rme-2017-0012. Epub 2017 Jun 16. Regen Med. 2017. PMID: 28621207 Review.
-
Conducting Polymers for Tissue Engineering.Biomacromolecules. 2018 Jun 11;19(6):1764-1782. doi: 10.1021/acs.biomac.8b00276. Epub 2018 Apr 30. Biomacromolecules. 2018. PMID: 29684268 Free PMC article. Review.
-
Current state of fabrication technologies and materials for bone tissue engineering.Acta Biomater. 2018 Oct 15;80:1-30. doi: 10.1016/j.actbio.2018.09.031. Epub 2018 Sep 22. Acta Biomater. 2018. PMID: 30248515 Review.
-
Biomimetic approaches for tissue engineering.J Biomater Sci Polym Ed. 2018 Oct;29(14):1667-1685. doi: 10.1080/09205063.2018.1500084. Epub 2018 Sep 26. J Biomater Sci Polym Ed. 2018. PMID: 29998794 Review.
Cited by
-
Application of biodegradable implants in pediatric orthopedics: shifting from absorbable polymers to biodegradable metals.Bioact Mater. 2025 Apr 10;50:189-214. doi: 10.1016/j.bioactmat.2025.04.001. eCollection 2025 Aug. Bioact Mater. 2025. PMID: 40256329 Free PMC article.
-
Nanofibrous Scaffolds' Ability to Induce Mesenchymal Stem Cell Differentiation for Soft Tissue Regenerative Applications.Pharmaceuticals (Basel). 2025 Feb 11;18(2):239. doi: 10.3390/ph18020239. Pharmaceuticals (Basel). 2025. PMID: 40006052 Free PMC article. Review.
-
Biodegradable Polymers: Properties, Applications, and Environmental Impact.Polymers (Basel). 2025 Jul 18;17(14):1981. doi: 10.3390/polym17141981. Polymers (Basel). 2025. PMID: 40732859 Free PMC article. Review.
-
Ultraminiaturized neural implanted constructs display minimal immunologic response.Mater Today Bio. 2025 Apr 29;32:101819. doi: 10.1016/j.mtbio.2025.101819. eCollection 2025 Jun. Mater Today Bio. 2025. PMID: 40391020 Free PMC article.
-
Fullerene-Functionalized Cellulosic Hydrogel Biosensor with Bacterial Turn-on Fluorescence Response Derived from Carboxymethyl Cellulose for Intelligent Food Packaging with DFT Calculations and Molecular Docking.Gels. 2025 Apr 28;11(5):329. doi: 10.3390/gels11050329. Gels. 2025. PMID: 40422349 Free PMC article.
References
-
- Vert M., Doi Y., Hellwich K. H., Hess M., Hodge P., Kubisa P., Rinaudo M., Schué F., Pure Appl. Chem. 2012, 84, 377.
-
- Kasi P. B., Azar M. G., Dodda J. M., Belsky P., Kovárík T., Slouf M., Dobrá J. K., Babuska V., Int. J. Biol. Macromol. 2023, 243, 125334. - PubMed
-
- Sowbhagya R., Muktha H., Ramakrishnaiah T. N., Surendra A. S., Sushma S. M., Tejaswini C., Roopini K., Rajashekara S., Tissue Cell 2024, 90, 102497. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

