State of the art: peripheral diagnostic bronchoscopy
- PMID: 39268128
- PMCID: PMC11388231
- DOI: 10.21037/jtd-24-346
State of the art: peripheral diagnostic bronchoscopy
Abstract
Lung cancer is the leading cause of cancer related death worldwide and in the United States according to the World Health Organization and National Cancer Institute. Improvements in the diagnosis and treatment of lung cancer are of the utmost importance. A prompt diagnosis is a crucial factor to improve outcomes in the treatment of lung cancer. Although the implementation of lung cancer screening guidelines and the overall steady growth in the use of computed tomography have improved the likelihood of detecting lung cancer at an earlier stage, the diagnosis of peripheral pulmonary lesions (PPLs) has remained a challenge. The bronchoscopic techniques for PPL sampling have historically offered modest diagnostic yields at best in comparison to computed tomography guided transthoracic needle aspiration (TTNA). Fortunately, recent advances in technology have ushered in a new era of diagnostic peripheral bronchoscopy. In this review, we discuss the introduction of advanced intraprocedural imaging included digital tomosynthesis (DT), augmented fluoroscopy (AF), and cone beam computed tomography. We discuss robotic assisted bronchoscopy with a review of the currently available platforms, and we discuss the implementation of novel biopsy tools. These technologic advances in the bronchoscopic approach to PPLs offer greater diagnostic certainty and pave the way toward peripheral therapeutics in bronchoscopy.
Keywords: Peripheral pulmonary lesion (PPL); cone beam computed tomography (CBCT); diagnostic bronchoscopy; robotic-assisted bronchoscopy (RAB).
2024 Journal of Thoracic Disease. All rights reserved.
Conflict of interest statement
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://jtd.amegroups.com/article/view/10.21037/jtd-24-346/coif). B.D.S. has worked as a consultant for both Ethicon (a subsidiary of Johnson & Johnson) and Noah Medical. H.B. has received support from Phillips in studying the efficacy of their LungSuite software, which is related to a portion of the topic of this review. H.B. has received support from Siemens, Philips, and GE as sponsors of the annual CBCT educational course held at Stanford. The other authors have no conflicts of interest to declare.
Figures
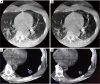

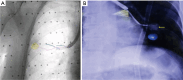
References
Publication types
LinkOut - more resources
Full Text Sources
