Metabolic health in people living with type 1 diabetes in Belgium: a repeated cross-sectional study
- PMID: 39271516
- PMCID: PMC11604828
- DOI: 10.1007/s00125-024-06273-7
Metabolic health in people living with type 1 diabetes in Belgium: a repeated cross-sectional study
Abstract
Aims/hypothesis: Metabolic abnormalities such as central obesity, insulin resistance, dyslipidaemia and hypertension, often referred to as 'the metabolic syndrome' (or 'combined metabolic abnormalities'), are increasingly being identified in people living with type 1 diabetes, accelerating the risk for CVD. As a result, in recent years, treatment in people living with type 1 diabetes has shifted to improving overall metabolic health rather than glucose control alone. In Belgium, diabetes care for people living with type 1 diabetes is centrally organised. The Initiative for Quality Improvement and Epidemiology in Diabetes, imposed by the Belgian health insurance system, has systematically collected data from patients on intensive insulin therapy treated in all 101 diabetes clinics in Belgium since 2001. The aim of this real-world study is to describe the evolution of treatment and metabolic health, including the prevalence of obesity and combined metabolic abnormalities, in people living with type 1 diabetes over the past 20 years, and to compare the treatment and prevalence of complications between those with and without combined metabolic abnormalities.
Methods: We analysed data on adults (≥16 years old) living with type 1 diabetes, who were diagnosed at age ≤45 years and who had a diabetes duration ≥1 year, collected between 2001 and 2022. The evolution of HbA1c, BMI, LDL-cholesterol, systolic BP, lipid-lowering therapy and antihypertensive therapy over time was analysed. The prevalence of individual and multiple metabolic abnormalities according to various definitions of the metabolic syndrome/combined metabolic abnormalities was analysed, and the association between combined metabolic abnormalities and metabolic health indicators, complications and treatment was investigated in the 2022 data.
Results: The final dataset consisted of 26,791 registrations of adults living with type 1 diabetes collected between 2001 and 2022. Although glycaemic and lipid control generally improved over time, the prevalence of obesity strongly increased (12.1% in 2001 vs 21.7% in 2022, p<0.0001), as did the presence of combined metabolic abnormalities (WHO criteria: 26.9% in 2001 vs 42.9% in 2022 in women, p<0.0001; 30.4% in 2001 vs 52.1% in 2022 in men, p<0.0001; WHO criteria without albuminuria: 22.3% in 2001 vs 40.6% in 2022 in women, p<0.0001; 25.1% in 2001 vs 49.2% in 2022 in men, p<0.0001; NCEP-ATPIII criteria: 39.9% in 2005 vs 57.2% in 2022 in women, p<0.0001; 40.8% in 2005 vs 60.9% in 2022 in men, p<0.0001; IDF criteria: 43.9% in 2005 vs 59.3% in 2022 in women, p<0.001; 33.7% in 2005 vs 50.0% in 2022 in men, p<0.0001). People with combined metabolic abnormalities had higher glucose levels compared to those without combined metabolic abnormalities (HbA1c >58 mmol in men: 48.9% vs 36.9%; HbA1c >58 mmol in women: 53.3% vs 41.1%, p<0.0001). People with combined metabolic abnormalities were more often treated with adjunct therapies such as metformin, sodium-glucose transport protein 2 inhibitors and glucagon-like peptide-1 receptor agonists. In both men and women, the presence of combined metabolic abnormalities was strongly related to the presence of eye complications, peripheral neuropathy, chronic kidney disease and CVD, corrected for age, diabetes duration and HbA1c.
Conclusions/interpretation: Overweight, obesity and combined metabolic abnormalities are increasingly being identified in people living with type 1 diabetes, further accelerating the risk of microvascular and macrovascular complications. Early identification of the presence of combined metabolic abnormalities should enable therapeutic interventions to be modified towards multifactorial approaches, with attention to education on avoidance of overweight (e.g. dietary counselling) in addition to strict glycaemic control and intensification of use of antihypertensive agents and statins. Use of adjunct therapies in this population as a tool should be explored more thoroughly to reduce risk of complications.
Keywords: Combined metabolic abnormalities; Diabetes complications; Diabetes treatment; Metabolic health; Metabolic syndrome; Obesity; Real-world data; Type 1 diabetes.
© 2024. The Author(s).
Conflict of interest statement
Acknowledgements: This article is written on behalf of the IQED Group of Experts. The members of the IQED Group of Experts are L. Crenier, C. De Block, A.-S. Vanherwegen, A. Lavens, C. Mathieu, F. Nobels, J.-C. Philips, P. Oriot, M. Vandenbroucke and V. Vanelshocht. We would like to thank the staff of all Belgian specialised diabetes centres for the data collection. Some of the data were presented as an abstract at the EASD meeting in 2023. Data availability: Data cannot be shared publicly because of the use of pseudonymised person-level data. Readers who wish to access some or all of the data require approval from the Belgian Information Security Committee on Social Security and Health. More information about the access procedure may be obtained by contacting iqed@sciensano.be. Metadata (e.g. overview of variables, legal framework) are available on https://fair.healthdata.be/ . Funding: The IQED programme is funded by the Belgian National Institute for Health and Disability Insurance. Authors’ relationships and activities: The authors declare that there are no relationships or activities that might bias, or be perceived to bias, their work. Contribution statement: AL, CM, PO and CDB developed the concept and design of this study. Data analysis was performed by AL. All authors made substantial contributions to the interpretation of results. AL, CDB, PO and CM drafted the manuscript, and all authors contributed to critical revision of the manuscript for important intellectual content. All authors approved the final manuscript for publication. AL had full access to the data and accepts the responsibility for the integrity of the data and accuracy of the data analysis.
Figures
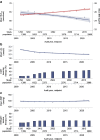

References
-
- DCCT Research Group, Nathan DM, Genuth S et al (1993) The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med 329(14):977–986. 10.1056/NEJM199309303291401 - PubMed
-
- Diabetes Control and Complications Trial (DCCT)/Epidemiology of Diabetes Interventions and Complications (EDIC) Study Research Group (2016) Intensive diabetes treatment and cardiovascular outcomes in type 1 diabetes: the DCCT/EDIC study 30-year follow-up. Diabetes Care 39(5):686–693. 10.2337/dc15-1990 - PMC - PubMed
-
- Van der Schueren B, Ellis D, Faradji RN, Al-Ozairi E, Rosen J, Mathieu C (2021) Obesity in people living with type 1 diabetes. Lancet Diabetes Endocrinol 9(11):776–785. 10.1016/S2213-8587(21)00246-1 - PubMed
-
- Edqvist J, Rawshani A, Adiels M et al (2019) BMI, mortality, and cardiovascular outcomes in type 1 diabetes: findings against an obesity paradox. Diabetes Care 42(7):1297–1304. 10.2337/dc18-1446 - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

