Intraoral Scanning Enables Virtual-Splint-Based Non-Invasive Registration Protocol for Maxillofacial Surgical Navigation
- PMID: 39274408
- PMCID: PMC11396243
- DOI: 10.3390/jcm13175196
Intraoral Scanning Enables Virtual-Splint-Based Non-Invasive Registration Protocol for Maxillofacial Surgical Navigation
Abstract
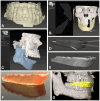
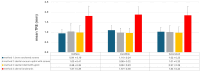
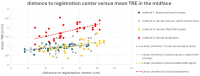
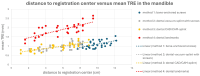
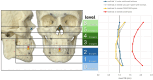
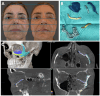
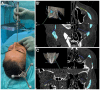
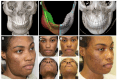
Background/Objectives: Surgical navigation has advanced maxillofacial surgery since the 1990s, bringing benefits for various indications. Traditional registration methods use fiducial markers that are either invasively bone-anchored or attached to a dental vacuum splint and offer high accuracy but necessitate additional imaging with increased radiation exposure. We propose a novel, non-invasive registration protocol using a CAD/CAM dental splint based on high-resolution intraoral scans. Methods: The effectiveness of this method was experimentally evaluated with an ex vivo 3D-printed skull measuring the target registration error (TRE). Surgical application is demonstrated in two clinical cases. Results: In the ex vivo model, the new CAD/CAM-splint-based method achieved a mean TRE across the whole facial skull of 0.97 ± 0.29 mm, which was comparable to traditional techniques like using bone-anchored screws (1.02 ± 0.23 mm) and dental vacuum splints (1.01 ± 0.33 mm), while dental anatomical landmarks showed a lower accuracy with a mean TRE of 1.84 ± 0.44 mm. Multifactorial ANOVA confirmed significant differences in TRE based on the registration method and the navigated level of the facial skull (p < 0.001). In clinical applications, the presented method demonstrated high accuracy for both midfacial and mandibular surgeries. Conclusions: Our results suggest that this non-invasive CAD/CAM-splint-based method is a viable alternative to traditional fiducial marker techniques, with the potential for broad application in maxillofacial surgery. This approach retains high accuracy while eliminating the need for supplementary imaging and reduces patient radiation exposure. Further clinical trials are necessary to confirm these findings and optimize splint design for enhanced navigational accuracy.
Keywords: computer-assisted planning; intraoral scanning; maxillofacial surgery; navigational registration; surgical navigation.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures

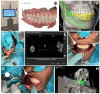
Similar articles
-
Novel CAD/CAM-splint-based navigation protocol enhances intraoperative maxillary position control in orthognathic surgery: a case control study.Head Face Med. 2025 Jan 10;21(1):1. doi: 10.1186/s13005-024-00477-3. Head Face Med. 2025. PMID: 39794777 Free PMC article.
-
Utilization of a 3D printed dental splint for registration during electromagnetically navigated mandibular surgery.Int J Comput Assist Radiol Surg. 2020 Dec;15(12):1997-2003. doi: 10.1007/s11548-020-02271-3. Epub 2020 Oct 16. Int J Comput Assist Radiol Surg. 2020. PMID: 33067757
-
Evaluation of two dental registration-splint techniques for surgical navigation in cranio-maxillofacial surgery.J Craniomaxillofac Surg. 2014 Jul;42(5):448-53. doi: 10.1016/j.jcms.2013.05.040. Epub 2013 Jul 5. J Craniomaxillofac Surg. 2014. PMID: 23835568
-
Comparison of 4 registration strategies for computer-aided maxillofacial surgery.Otolaryngol Head Neck Surg. 2007 Jul;137(1):93-9. doi: 10.1016/j.otohns.2007.02.015. Otolaryngol Head Neck Surg. 2007. PMID: 17599573
-
Point-to-point registration with mandibulo-maxillary splint in open and closed jaw position. Evaluation of registration accuracy for computer-aided surgery of the mandible.J Craniomaxillofac Surg. 2012 Oct;40(7):592-8. doi: 10.1016/j.jcms.2011.10.016. Epub 2011 Nov 10. J Craniomaxillofac Surg. 2012. PMID: 22079336
Cited by
-
Novel CAD/CAM-splint-based navigation protocol enhances intraoperative maxillary position control in orthognathic surgery: a case control study.Head Face Med. 2025 Jan 10;21(1):1. doi: 10.1186/s13005-024-00477-3. Head Face Med. 2025. PMID: 39794777 Free PMC article.
References
LinkOut - more resources
Full Text Sources
Miscellaneous

