Clinical utility of an artificial intelligence radiomics-based tool for risk stratification of pulmonary nodules
- PMID: 39292567
- PMCID: PMC11521375
- DOI: 10.1093/jncics/pkae086
Clinical utility of an artificial intelligence radiomics-based tool for risk stratification of pulmonary nodules
Abstract
Background: Clinical utility data on pulmonary nodule (PN) risk stratification biomarkers are lacking. We aimed to determine the incremental predictive value and clinical utility of using an artificial intelligence (AI) radiomics-based computer-aided diagnosis (CAD) tool in addition to routine clinical information to risk stratify PNs among real-world patients.
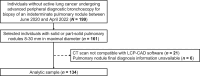
Methods: We performed a retrospective cohort study of patients with PNs who underwent lung biopsy. We collected clinical data and used a commercially available AI radiomics-based CAD tool to calculate a Lung Cancer Prediction (LCP) score. We developed logistic regression models to evaluate a well-validated clinical risk prediction model (the Mayo Clinic model) with and without the LCP score (Mayo vs Mayo + LCP) using area under the curve (AUC), risk stratification table, and standardized net benefit analyses.
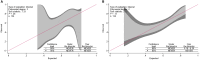
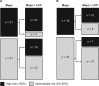
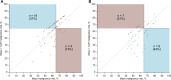
Results: Among the 134 patients undergoing PN biopsy, cancer prevalence was 61%. Addition of the radiomics-based LCP score to the Mayo model was associated with increased predictive accuracy (likelihood ratio test, P = .012). The AUCs for the Mayo and Mayo + LCP models were 0.58 (95% CI = 0.48 to 0.69) and 0.65 (95% CI = 0.56 to 0.75), respectively. At the 65% risk threshold, the Mayo + LCP model was associated with increased sensitivity (56% vs 38%; P = .019), similar false positive rate (33% vs 35%; P = .8), and increased standardized net benefit (18% vs -3.3%) compared with the Mayo model.
Conclusions: Use of a commercially available AI radiomics-based CAD tool as a supplement to clinical information improved PN cancer risk prediction and may result in clinically meaningful changes in risk stratification.
© The Author(s) 2024. Published by Oxford University Press.
Conflict of interest statement
L.C.P. is an employee of and owns stock in Optellum, Ltd. The remaining authors do not report conflicts of interest relevant to this submitted work.
Figures
References
-
- Gould MK, Donington J, Lynch WR, et al. Evaluation of individuals with pulmonary nodules: when is it lung cancer? Diagnosis and management of lung cancer, 3rd ed: American College of Chest Physicians evidence-based clinical practice guidelines. Chest. 2013;143(suppl 5):e93S-e120S. doi: 10.1378/chest.12-2351 - DOI - PMC - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous
