Identifying Racial Disparities in Utilization and Clinical Outcomes of Ambulatory Hip Arthroscopy: Analysis of Temporal Trends and Causal Inference via Machine Learning
- PMID: 39314831
- PMCID: PMC11418677
- DOI: 10.1177/23259671241257507
Identifying Racial Disparities in Utilization and Clinical Outcomes of Ambulatory Hip Arthroscopy: Analysis of Temporal Trends and Causal Inference via Machine Learning
Abstract
Background: Arthroscopic diagnosis and treatment of femoroacetabular pathology has experienced significant growth in the last 30 years; nevertheless, reduced utilization of orthopaedic procedures has been observed among the underrepresented population.
Purpose/hypothesis: The purpose of this study was to examine racial differences in case incidence rates, outcomes, and complications in patients undergoing hip arthroscopy. It was hypothesized that racial and ethnic minority patients would undergo hip arthroscopy at a decreased rate compared with their White counterparts but that there would be no differences in clinical outcomes.
Study design: Cross-sectional study.
Methods: The State Ambulatory Surgery and Services Database and the State Emergency Department Database of New York were queried for patients undergoing hip arthroscopy between 2011 and 2017. Patients were stratified into White and racial and ethnic minority races, and intergroup comparisons were performed for utilization over time, total charges billed per encounter, 90-day emergency department (ED) visits, and revision hip arthroscopy. Temporal trends in the utilization of hip arthroscopy were identified, and racial differences in secondary outcomes were analyzed with a semiparametric method known as targeted maximum likelihood estimation (TMLE) backed by a library of machine learning algorithms.
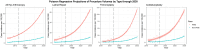
Results: A total of 9745 patients underwent hip arthroscopy during the study period, with 1081 patients of minority race (11.1%). White patients underwent hip arthroscopy at 5.68 (95% CI, 4.98-6.48) times the incidence rate of racial and ethnic minority patients; these incidence rates grew annually at a ratio of 1.11 in White patients compared with 1.03 in racial and ethnic minority patients (P < .001). Based on the TMLE, racial and ethnic minority patients were significantly more likely to incur higher costs (P < .001) and visit the ED within 90 days (P = .049) but had negligible differences in reoperation rates at a 2-year follow-up (P = .53). Subgroup analysis identified that higher likelihood for 90-day ED admissions among racial and ethnic minority patients compared with White patients was associated with Medicare insurance (P = .002), median income in the lowest quartile (P = .012), and residence in low-income neighborhoods (P = .006).
Conclusion: Irrespective of insurance status, racial and ethnic minority patients undergo hip arthroscopy at a lower incidence and incur higher costs per surgical encounter.
Keywords: diversity; femoroacetabular impingement; hip; hip arthroscopy; hip/pelvis/thigh; machine learning.
© 2024 The Author(s).
Conflict of interest statement
One or more of the authors has declared the following conflict of interest or source of funding: E.M.M. has received education payments from Exactech and hospitality payments from Stryker. M.D. has received hospitality payments from Stryker. M.H. has received education payments from Arthrex, Foundation Medical, Medwest Associates, and Smith+Nephew; honoraria from Encore Medical; hospitality payments from Orthalign and Medical Device Business Services; and consulting fees from Vericel. B.A.L. has received consulting fees from Arthrex and Smith+Nephew; nonconsulting fees from Arthrex, Smith+Nephew, and Linvatec; and royalties or license payments from Arthrex. A.J.K. has received nonconsulting fees from Arthrex; royalties or license payments from Arthrex; consulting fees from Arthrex, JRF Ortho, and Responsive Arthroscopy; a grant from DJO; and honoraria from JRF Ortho and MTF Biologics. K.R.O. has received education payments from Foundation Medical, Gemini Medical, Arthrex, Endo Pharmaceuticals, Pinnacle, Medwest Associates, and Smith+Nephew; nonconsulting fees from Smith+Nephew, Arthrex, and Medical Device Business Services; hospitality payments from Stryker, Arthrex, Wright Medical Technology, Medical Device Business Services, and Zimmer Biomet Holdings; consulting fees from Endo Pharmaceuticals and Smith+Nephew; and a grant from Arthrex. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
Figures



Similar articles
-
National Patterns in Utilization of Knee and Hip Arthroscopy: An Analysis of Racial, Ethnic, and Geographic Disparities in the United States.Orthop J Sports Med. 2023 Aug 16;11(8):23259671231187447. doi: 10.1177/23259671231187447. eCollection 2023 Aug. Orthop J Sports Med. 2023. PMID: 37655237 Free PMC article.
-
Patient Sociodemographics and Comorbidities and Birth Hospital Characteristics Associated With Postpartum Emergency Department Care.JAMA Netw Open. 2023 Mar 1;6(3):e233927. doi: 10.1001/jamanetworkopen.2023.3927. JAMA Netw Open. 2023. PMID: 36943266 Free PMC article.
-
The role of race and ethnicity in the State Children's Health Insurance Program (SCHIP) in four states: are there baseline disparities, and what do they mean for SCHIP?Pediatrics. 2003 Dec;112(6 Pt 2):e521. Pediatrics. 2003. PMID: 14654674
-
Is Our Science Representative? A Systematic Review of Racial and Ethnic Diversity in Orthopaedic Clinical Trials from 2000 to 2020.Clin Orthop Relat Res. 2022 May 1;480(5):848-858. doi: 10.1097/CORR.0000000000002050. Epub 2021 Dec 2. Clin Orthop Relat Res. 2022. PMID: 34855650 Free PMC article.
-
Systematic Review and Meta-analysis of Outcomes After Hip Arthroscopy in Femoroacetabular Impingement.Am J Sports Med. 2019 Feb;47(2):488-500. doi: 10.1177/0363546517749475. Epub 2018 Jan 26. Am J Sports Med. 2019. PMID: 29373805
References
-
- Allen MM, Pareek A, Krych AJ, et al.. Are female soccer players at an increased risk of second anterior cruciate ligament injury compared with their athletic peers? Am J Sports Med. 2016;44(10):2492-2498. - PubMed
-
- Amen TB, Varady NH, Rajaee S, Chen AF. Persistent racial disparities in utilization rates and perioperative metrics in total joint arthroplasty in the U.S.: a comprehensive analysis of trends from 2006 to 2015. J Bone Joint Surg Am. 2020;102(9):811-820. - PubMed
-
- Amen TB, Varady NH, Wright-Chisem J, et al.. Emerging racial disparities in outpatient utilization of total joint arthroplasty. J Arthroplasty. 2022;37(11):2116-2121. - PubMed
-
- Braaten AD, Hanebuth C, McPherson H, et al.. Social determinants of health are associated with physical therapy use: a systematic review. Br J Sports Med. 2021;55(22):1293-1300. - PubMed
LinkOut - more resources
Full Text Sources

