Noninvasive intracranial pressure profile in 31 patients submitted to fullendoscopic spine surgery
- PMID: 39319901
- PMCID: PMC11414522
- DOI: 10.1590/acb396424
Noninvasive intracranial pressure profile in 31 patients submitted to fullendoscopic spine surgery
Abstract
Purpose: Full-endoscopic spine surgery (FESS) is associated with specific complications, possibly linked to increased intracranial pressure (ICP) resulting from continuous saline infusion into the epidural space. This study aimed to assess the impact of saline irrigation and its correlation with noninvasively obtained ICP waveform changes.
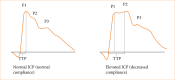
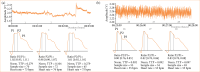
Methods: Patients undergoing FESS between January 2019 and November 2020 were included. Noninvasive ICP (n-ICP) monitoring utilized an extracranial strain sensor generating ICP waveforms, from which parameters P2/P1 ratio and time to peak (TTP) values were derived and correlated to irrigation and vital parameters. Documentation occurred at specific surgical intervals (M0-preoperatively; M1 to M4-intraoperatively; M5-postoperatively). Mixed-model analysis of variance and multiple comparisons tests were applied, with M0 as the baseline.
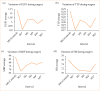
Results: Among 31 enrolled patients, three experienced headaches unrelated to increased ICP at M5. The P2/P1 ratio and TTP decreased during surgery (p < 0.001 and p < 0.004, respectively). Compared to baseline, P2/P1 ratio and vital parameters remained significantly lower at M5. No significant differences were observed for fluid parameters throughout surgery.
Conclusions: This study demonstrated a decline in the n-ICP parameters after anesthetic induction despite the anticipated increase in ICP due to constant epidural irrigation. The n-ICP parameters behaved independently of fluid parameters, suggesting a potential protective effect of anesthesia.
Conflict of interest statement
Figures


Similar articles
-
Intracranial Pressure Evaluation in Swine During Full-Endoscopic Lumbar Spine Surgery.World Neurosurg. 2023 Nov;179:e557-e567. doi: 10.1016/j.wneu.2023.09.001. Epub 2023 Sep 9. World Neurosurg. 2023. PMID: 37690580
-
Waveform Morphology as a Surrogate for ICP Monitoring: A Comparison Between an Invasive and a Noninvasive Method.Neurocrit Care. 2022 Aug;37(1):219-227. doi: 10.1007/s12028-022-01477-4. Epub 2022 Mar 24. Neurocrit Care. 2022. PMID: 35332426 Free PMC article.
-
Can a new noninvasive method for assessment of intracranial pressure predict intracranial hypertension and prognosis?Acta Neurochir (Wien). 2023 Jun;165(6):1495-1503. doi: 10.1007/s00701-023-05580-z. Epub 2023 Apr 15. Acta Neurochir (Wien). 2023. PMID: 37061612 Free PMC article.
-
[Value of serial CT scanning and intracranial pressure monitoring for detecting new intracranial mass effect in severe head injury patients showing lesions type I-II in the initial CT scan].Neurocirugia (Astur). 2005 Jun;16(3):217-34. Neurocirugia (Astur). 2005. PMID: 16007322 Review. Spanish.
-
Ultrasonographic optic nerve sheath diameter for predicting elevated intracranial pressure during laparoscopic surgery: a systematic review and meta-analysis.Surg Endosc. 2018 Jan;32(1):175-182. doi: 10.1007/s00464-017-5653-3. Epub 2017 Jun 21. Surg Endosc. 2018. PMID: 28639043
References
-
- Wu C, Lee CY, Chen SC, Hsu SK, Wu MH. Functional outcomes of full-endoscopic spine surgery for high-grade migrated lumbar disc herniation: a prospective registry-based cohort study with more than 5 years of follow-up. BMC Musculoskelet Disord. 2021;22(1):58–58. doi: 10.1186/s12891-020-03891-1. - DOI - PMC - PubMed
-
- Phan K, Xu J, Schultz K, Alvi MA, Lu VM, Kerezoudis P, Maloney PR, Murphy ME, Mobbs RJ, Bydon M. Full-endoscopic versus micro-endoscopic and open discectomy: A systematic review and meta-analysis of outcomes and complications. Clin Neurol Neurosurg. 2017;154:1–12. doi: 10.1016/j.clineuro.2017.01.003. - DOI - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

