Global parental acceptance, attitudes, and knowledge regarding human papillomavirus vaccinations for their children: a systematic literature review and meta-analysis
- PMID: 39334328
- PMCID: PMC11428909
- DOI: 10.1186/s12905-024-03377-5
Global parental acceptance, attitudes, and knowledge regarding human papillomavirus vaccinations for their children: a systematic literature review and meta-analysis
Abstract
Background: This systematic literature review aims to summarize global research on parental acceptance, attitudes, and knowledge regarding human papillomavirus vaccinations.
Methods: The literature search was conducted in PubMed, Web of Science and Scopus, and included publications from 2006 to 2023. Study quality was assessed using the Newcastle-Ottawa Scale. The Grading of Recommendations Assessment, Development, and Evaluation guidelines were used to assess the strength of evidence for the primary outcome. Meta-analyses were performed using random-effects models to estimate pooled parental acceptance of HPV vaccinations. Studies were stratified by study years, and a subgroup analysis was conducted to estimate vaccine acceptance rates by world regions. Additionally, sensitivity analyses examined the role of parents in accepting HPV vaccinations for children of different sexes.
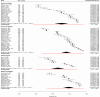
Results: Based on 86 studies, we found that parents generally supported HPV vaccinations for their children, yet HPV vaccine acceptance rates showed high variation (12.0 to 97.5%). The subgroup analysis revealed geographical variations in pooled parental HPV vaccine acceptance rates, with the highest rate observed in Africa (79.6%; 95% CI: 73.5-85.2; I² = 98.3%; p < 0.01) and the lowest in North America (56.7%; 95% CI: 49.3-64.0; I² = 99.4%; p < 0.01). Sensitivity analyses showed that acceptance was higher for daughters than for sons, with mothers more willing to get their daughters vaccinated. The proportion of parents reporting barriers or benefits regarding HPV vaccinations varied widely (0.3-95.8%) between study regions. Across all world regions, fear of adverse effects and concerns about vaccine safety were the main barriers, whereas the desire to protect their children from cancer was a significant predictor of vaccine acceptance. Knowledge levels varied widely (6.5 to 100%) between world regions and according to the questions asked. In most studies, knowledge e.g., that HPV is sexually transmitted, and that HPV vaccination provides protection against cervical cancer, ranged from moderate to high.
Conclusions: The results indicated moderate parental acceptance of HPV vaccines. Public knowledge of HPV infection should be promoted, and special efforts should be made to minimize the existing barriers and increase vaccination accessibility and uptake.
Keywords: Acceptance; Human papillomavirus; Meta-analysis; Systematic review; Vaccination.
© 2024. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures



Similar articles
-
Barriers associated with the parental acceptance of human papillomavirus (HPV) vaccination of minors in Asir, Saudi Arabia: A cross-sectional study.Hum Vaccin Immunother. 2025 Dec;21(1):2513708. doi: 10.1080/21645515.2025.2513708. Epub 2025 Jun 3. Hum Vaccin Immunother. 2025. PMID: 40462525 Free PMC article.
-
A systematic review and meta-analysis on parental uptake and willingness to vaccinate children against human papillomavirus in the Eastern Mediterranean Region.Vaccine. 2025 Mar 7;49:126832. doi: 10.1016/j.vaccine.2025.126832. Epub 2025 Feb 6. Vaccine. 2025. PMID: 39920024
-
Parental Perspectives on Human Papillomavirus (HPV) Vaccination in Gulf Cooperation Council Countries: A systematic review.Medicine (Baltimore). 2024 Oct 18;103(42):e40124. doi: 10.1097/MD.0000000000040124. Medicine (Baltimore). 2024. PMID: 39432651 Free PMC article.
-
Knowledge and willingness of parents towards child girl HPV vaccination in Debre Tabor Town, Ethiopia: a community-based cross-sectional study.Reprod Health. 2022 Jun 10;19(1):136. doi: 10.1186/s12978-022-01444-4. Reprod Health. 2022. PMID: 35689288 Free PMC article.
-
Human papillomavirus vaccination hesitancy among young girls in Ethiopia: factors and barriers to uptake.Front Public Health. 2025 Jan 23;13:1507832. doi: 10.3389/fpubh.2025.1507832. eCollection 2025. Front Public Health. 2025. PMID: 39916703 Free PMC article.
Cited by
-
Therapeutic Impact of Gardasil® in Recurrent Respiratory Papillomatosis: A Retrospective Study on RRP Patients.Viruses. 2025 Feb 26;17(3):321. doi: 10.3390/v17030321. Viruses. 2025. PMID: 40143250 Free PMC article.
-
Knowledge of Human Papillomavirus, Risk Factors and Screening for Cervical Cancer Among Women in Ghana.Cancer Control. 2025 Jan-Dec;32:10732748251323765. doi: 10.1177/10732748251323765. Cancer Control. 2025. PMID: 40009887 Free PMC article.
-
Barriers associated with the parental acceptance of human papillomavirus (HPV) vaccination of minors in Asir, Saudi Arabia: A cross-sectional study.Hum Vaccin Immunother. 2025 Dec;21(1):2513708. doi: 10.1080/21645515.2025.2513708. Epub 2025 Jun 3. Hum Vaccin Immunother. 2025. PMID: 40462525 Free PMC article.
-
HPV vaccination willingness among 3,081 secondary school parents in China's capital.Hum Vaccin Immunother. 2025 Dec;21(1):2477383. doi: 10.1080/21645515.2025.2477383. Epub 2025 Mar 12. Hum Vaccin Immunother. 2025. PMID: 40072923 Free PMC article.
-
Factors affecting caregivers' HPV vaccination decisions for adolescent girls: A secondary analysis of a Chinese RCT.PLoS One. 2025 Jun 17;20(6):e0324260. doi: 10.1371/journal.pone.0324260. eCollection 2025. PLoS One. 2025. PMID: 40526724 Free PMC article. Clinical Trial.
References
-
- Herzog TJ. New approaches for the management of cervical cancer. Gynecol Oncol. 2003;90:S22–7. 10.1016/s0090-8258(03)00466-9. - PubMed
-
- Chaturvedi AK. Beyond cervical cancer: burden of other HPV-related cancers among men and women. J Adolesc Health. 2010;46:S20–6. 10.1016/j.jadohealth.2010.01.016. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

