Allograft Screws as Fixation of the Scarf Osteotomy
- PMID: 39337115
- PMCID: PMC11433284
- DOI: 10.3390/jcm13185628
Allograft Screws as Fixation of the Scarf Osteotomy
Abstract
Background: In comparison to titanium screws, novel cortical bone allograft screws may come with advantages in osseointegration and with avoidance of potential material removal surgery after scarf osteotomy. Methods: A scarf osteotomy with allograft bone screws as fixation was performed in 21 patients (30 feet). Clinical and radiological parameters were prospectively collected until one year after surgery. A retrospective control group, consisting of 75 patients (82 feet) after scarf osteotomy using headless compression screws, was used to compare clinical outcomes. Results: After fixation with allograft bone screws, the mean preoperative AOFAS score increased from 51.5 points preoperatively to 93.5 points one year after surgery. In radiological assessments, a continuous osseointegration with the remodeling of the bone screw was observed in all patients that finished follow-up. However, four metatarsal fractures occurred early postoperatively after fixation using allograft bone screws. There were only three material removal surgeries in patients treated with headless compression screws. Conclusions: Allograft bone screws display a safe fixation and are a biological alternative for scarf osteotomy. Enough distance between the screw and the proximal osteotomy should be ensured to avoid fractures.
Keywords: allograft bone screw; headless compression screw; scarf osteotomy.
Conflict of interest statement
One of the authors (RW) receives consulting fees from Johnson&Johnson Medical Limited (New Brunswick, NJ, USA) and consulting fees from Stryker European Operations Limited (Amsterdam, NL, EU). K.D., S.A., M.H. and S.P. confirm that there are no conflicts of interest associated with this publication, and there has been no financial support for this work that could have influenced its outcome.
Figures



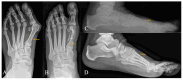
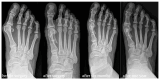
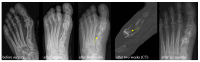
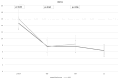
References
-
- Partio N., Ponkilainen V.T., Rinkinen V., Honkanen P., Haapasalo H., Laine H.J., Mäenpää H.M. Interpositional Arthroplasty of the First Metatarsophalangeal Joint with Bioresorbable Pldla Implant in the Treatment of Hallux Rigidus and Arthritic Hallux Valgus: A 9-Year Case Series Follow-Up. Scand. J. Surg. 2021;110:93–98. doi: 10.1177/1457496919893597. - DOI - PubMed
-
- Jentzsch T., Renner N., Niehaus R., Farei-Campagna J., Deggeller M., Scheurer F., Palmer K., Wirth S.H. The influence of the number of screws and additional surgical procedures on outcome in hallux valgus treatment. J. Orthop. Surg. Res. 2018;13:99. doi: 10.1186/s13018-018-0796-z. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources

