Pneumolysin contributes to dysfunction of nasal epithelial barrier for promotion of pneumococcal dissemination into brain tissue
- PMID: 39345124
- PMCID: PMC11520308
- DOI: 10.1128/msphere.00655-24
Pneumolysin contributes to dysfunction of nasal epithelial barrier for promotion of pneumococcal dissemination into brain tissue
Abstract
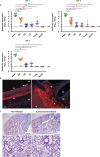
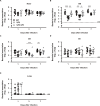
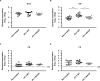
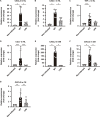
Streptococcus pneumoniae is one of the major pathogens responsible for bacterial meningitis and neurological sequelae. The present study was conducted to identify a non-hematogenous route used by S. pneumoniae to gain access to brain tissue without causing bacteremia or pneumonia, as well as bacterial and host factors involved in this process. To investigate the molecular mechanisms and dissemination pathways of pneumococcal infection in brain tissue, mice were intranasally inoculated with S. pneumoniae strain EF3030, a clinical isolate from a patient with otitis media. Pneumococci were isolated from the frontal olfactory bulb, caudal cerebrum, and cerebellum, with neither bacteremia nor pneumonia observed in the present model. Immunostaining imaging revealed the presence of S. pneumoniae organisms in olfactory nerve fibers. Knockout of the ply gene encoding pneumolysin (PLY) markedly compromised the ability of the bacterial organisms to disseminate into brain tissue, whereas the dissemination efficiency of the complemented strain was restored to nearly the same level as the wild type. Notably, distinct upregulation of Gli1 and Snail1, which are involved in the transcriptional repression of junctional proteins, along with downregulation of E-cadherin, was detected in nasal lavage samples from mice infected with the wild-type or complemented strain, but not in those from mice infected with the ply mutant. Taken together, the present findings indicate that PLY induces Gli1-Snail1-dependent dysfunction of the nasal epithelial barrier, thus allowing pneumococcal dissemination to brain tissue that occurs in a non-hematogenous manner.IMPORTANCEBacterial meningitis, considered to be caused by bacteremia, can lead to blood-brain barrier disruption and bacterial dissemination into the central nervous system. Despite the availability of intravenously administered antibiotics with cerebrospinal fluid transferability, bacterial meningitis remains associated with high rates of morbidity and mortality. Here, we utilized Streptococcus pneumoniae strain EF3030, clinically isolated from otitis media, for the construction of a murine infection model to investigate the molecular mechanisms by which nasally colonized pneumococci disseminate into brain tissue. The obtained findings indicate that pneumolysin (PLY) induces Gli1-Snail1-dependent dysfunction of the nasal epithelial barrier, which facilitates pneumococcal dissemination to brain tissue in a non-hematogenous manner. Our results support the existence of an alternative route by which S. pneumoniae can reach the central nervous system and indicate the need for the development of novel therapeutic strategies, which would be an important contribution to the clinical management of bacterial meningitis.
Keywords: Streptococcus pneumoniae; bacterial meningitis; non-hematogenous route; pneumolysin.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

References
-
- WHO . 2014. The world health report 2014. Geneva
MeSH terms
Substances
Grants and funding
- JP22wm0325019,JP23wm0325062/Japan Agency for Medical Research and Development (AMED)
- JP22fk0108130/Japan Agency for Medical Research and Development (AMED)
- JP18K19643,JP22H03262,JP22K19618/MEXT | Japan Society for the Promotion of Science (JSPS)
- JP22H03301/MEXT | Japan Society for the Promotion of Science (JSPS)
- JP22H03263/MEXT | Japan Society for the Promotion of Science (JSPS)
LinkOut - more resources
Full Text Sources
Medical
Research Materials
