The Etiology and Pathogenesis of Benign Prostatic Hyperplasia: The Roles of Sex Hormones and Anatomy
- PMID: 39345801
- PMCID: PMC11430843
- DOI: 10.2147/RRU.S477396
The Etiology and Pathogenesis of Benign Prostatic Hyperplasia: The Roles of Sex Hormones and Anatomy
Abstract
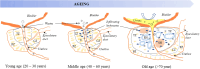
Benign prostatic hyperplasia (BPH) mainly causes lower urinary tract symptoms in ageing men, but its exact etiology and pathogenesis have not been established. The objective of this review was to design an update on the advances of human BPH research. We undertook a literature search for identifying studies of the roles of sex hormones (androgens and estrogens) in the onset and development of human BPH using the Pubmed database. In literature, many studies have indicated that ageing and obesity are the factors for preceding the onset of BPH. No evidence for the role of testosterone (T) or dihydrotestosterone (DHT) is found in BPH initiation. Since BPH exclusively occurs in the transitional zone (TZ) surrounding the urethra, it is postulated that years of exposure to uncharacterized urinary toxins could disrupt the homeostasis of the stroma and/or epithelium of this prostatic zone that are typically occurring in ageing men. After cellular damage and subsequent inflammation generated, the intraprostatic DHT produced mainly from T by 5α-reductase promotes BPH development. Further, estrogens could take part in the nodular proliferation of stromal cells in some BPH patients. The confounding of BPH may attenuate the development of prostate tumor in the TZ. In conclusion, evidence in literature suggests that androgens are not etiological factors for BPH, and intraprostatic DHT along with chronic inflammation are mainly responsible for nodular proliferation of stromal and/or epithelial cells in prostatic TZ. The urinary factors for the etiology of BPH and BPH as a prediction of PCa progression still need further investigation.
Keywords: androgens; benign prostatic hyperplasia; epithelium; etiology; nodular proliferation; steroid sex hormones; stroma; tissue homeostasis.
© 2024 Xu et al.
Conflict of interest statement
All authors have no competing interest to declare.
Figures
Similar articles
-
Androgens and estrogens: their interaction with stroma and epithelium of human benign prostatic hyperplasia and normal prostate.J Steroid Biochem. 1983 Jul;19(1A):155-61. J Steroid Biochem. 1983. PMID: 6193338
-
Combined treatment with dihydrotestosterone and lipopolysaccharide modulates prostate homeostasis by upregulating TNF-α from M1 macrophages and promotes proliferation of prostate stromal cells.Asian J Androl. 2022 Sep-Oct;24(5):513-520. doi: 10.4103/aja2021114. Asian J Androl. 2022. PMID: 34975070 Free PMC article.
-
Dihydrotestosterone and the concept of 5alpha-reductase inhibition in human benign prostatic hyperplasia.World J Urol. 2002 Apr;19(6):413-25. doi: 10.1007/s00345-002-0248-5. World J Urol. 2002. PMID: 12022710 Review.
-
The prostaglandin pathway is activated in patients who fail medical therapy for benign prostatic hyperplasia with lower urinary tract symptoms.Prostate. 2021 Sep;81(13):944-955. doi: 10.1002/pros.24190. Epub 2021 Jul 20. Prostate. 2021. PMID: 34288015 Free PMC article.
-
Intraprostatic testosterone and dihydrotestosterone. Part I: concentrations and methods of determination in men with benign prostatic hyperplasia and prostate cancer.BJU Int. 2012 Jan;109(2):176-82. doi: 10.1111/j.1464-410X.2011.10651.x. Epub 2011 Oct 12. BJU Int. 2012. PMID: 21992222 Review.
Cited by
-
Impact of fatty liver index and metabolic dysfunction-associated steatotic liver disease on the risk of benign prostatic hyperplasia in older male adults.BMC Geriatr. 2025 Aug 14;25(1):625. doi: 10.1186/s12877-025-06314-9. BMC Geriatr. 2025. PMID: 40813969 Free PMC article.
-
Genetically predicted benign prostate hyperplasia causally affects prostate cancer: a two-sample Mendelian randomization.Transl Androl Urol. 2025 Mar 30;14(3):661-668. doi: 10.21037/tau-2024-673. Epub 2025 Mar 26. Transl Androl Urol. 2025. PMID: 40226058 Free PMC article.
-
Association between the non-high-density lipoprotein cholesterol to high-density lipoprotein cholesterol ratio (NHHR) and early-onset benign prostatic hyperplasia: a cross-sectional analysis based on NHANES.J Health Popul Nutr. 2025 Aug 23;44(1):307. doi: 10.1186/s41043-025-01048-1. J Health Popul Nutr. 2025. PMID: 40849494 Free PMC article.
-
Chemopreventive Potential of Paddy Waste: A Promising Approach Against Benign Prostate Hyperplasia in Spontaneously Hypertensive Rats.Anal Cell Pathol (Amst). 2025 Mar 13;2025:4029625. doi: 10.1155/ancp/4029625. eCollection 2025. Anal Cell Pathol (Amst). 2025. PMID: 40115867 Free PMC article.
-
Association between TyG-BMI and BPH in a national prospective cohort study.Sci Rep. 2025 Mar 13;15(1):8743. doi: 10.1038/s41598-024-81629-y. Sci Rep. 2025. PMID: 40082448 Free PMC article.
References
-
- Awedew AF. The global, regional, and national burden of benign prostatic hyperplasia in 204 countries and territories from 2000 to 2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet Health Longev. 2022;3(11):e754–e776. doi:10.1016/S2666-7568(22)00213-6 - DOI - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources

