Association of autosomal mosaic chromosomal alterations with risk of bladder cancer in Chinese adults: a prospective cohort study
- PMID: 39349436
- PMCID: PMC11443067
- DOI: 10.1038/s41419-024-07087-6
Association of autosomal mosaic chromosomal alterations with risk of bladder cancer in Chinese adults: a prospective cohort study
Abstract
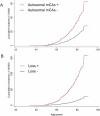
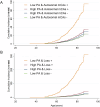
Little is known about the prospective association between autosomal mosaic chromosomal alterations (mCAs), a group of large-scale somatic mutations on autosomes, and bladder cancer. Here we utilized data from 99,877 participants who were free of physician-diagnosed cancer at baseline (2004-2008) of the China Kadoorie Biobank to estimate the associations between autosomal mCAs and bladder cancer (ICD-10: C67). A total of 2874 autosomal mCAs events among 2612 carriers (2.6%) were detected. After a median follow-up of 12.4 years, we discovered that participants with all autosomal mCAs exhibited higher risks of bladder cancer, with a multivariable-adjusted hazard ratio (HR) (95% confidence interval [CI]) of 2.60 (1.44, 4.70). The estimate of such association was even stronger for mosaic loss events (HR [95% CI]: 6.68 [2.92, 15.30]), while it was not significant for CN-LOH events. Both expanded (cell fraction ≥10%) and non-expanded autosomal mCAs, as well as mosaic loss, were associated with increased risks of bladder cancer. Of interest, physical activity (PA) significantly modified the associations of autosomal mCAs and mosaic loss (Pinteraction = 0.038 and 0.012, respectively) with bladder cancer. The increased risks of bladder cancer were only observed with mCAs and mosaic loss among participants with a lower level of PA (HR [95% CI]: 5.11 [2.36, 11.09] and 16.30 [6.06, 43.81]), but not among participants with a higher level of PA. Our findings suggest that peripheral leukocyte autosomal mCAs may represent a novel risk factor for bladder cancer, and PA may serve as a potential intervention target for mCAs carriers.
© 2024. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures

References
-
- Ferlay J, Ervik M, Lam F, Laversanne M, Colombet M, Mery L, et al. Global Cancer Observatory: Cancer Today. Lyon, France: International Agency for Research on Cancer; 2022. Available from: https://gco.iarc.fr/today
MeSH terms
Grants and funding
- WT_/Wellcome Trust/United Kingdom
- 82192901,82192904, 82192900,81390540, 91846303, 81941018/National Natural Science Foundation of China (National Science Foundation of China)
- 2011BAI09B01/Chinese Ministry of Science and Technology | Department of S and T for Social Development (Department of S&T for Social Development)
- 212946/Z/18/Z, 202922/Z/16/Z, 104085/Z/14/Z, 088158/Z/09/Z/Wellcome Trust (Wellcome)
LinkOut - more resources
Full Text Sources
Medical

