The impact of periampullary diverticula on cannulation and adverse events in endoscopic retrograde cholangiopancreatography
- PMID: 39398975
- PMCID: PMC11470493
- DOI: 10.1177/17562848241279105
The impact of periampullary diverticula on cannulation and adverse events in endoscopic retrograde cholangiopancreatography
Abstract
Background: Periampullary diverticulum (PAD) is commonly encountered in endoscopic retrograde cholangiopancreatography (ERCP) procedures.
Objectives: We sought to determine whether PADs are associated with a lower success rate of cannulation and an increased risk of adverse events.
Design: A retrospective cohort study was conducted using prospectively gathered nationwide registry data.
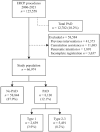
Methods: Using the Swedish registry for gallstone surgery and ERCP, we analyzed a cohort of 66,974 prospectively registered ERCP procedures performed in 2006-2021. The presence of PAD was divided into two groups based on the PAD type: Boix type 1 (the papilla located inside the PAD) and Boix types 2-3 (the papilla located either at the edge of the PAD or immediately adjacent to the PAD). The primary outcomes were the success rate of cannulation and overall adverse events within 30 days.
Results: PADs were registered in 8130 (12.1%) of ERCPs included in the study population. In total, 2114 (3.9%) patients had Boix type 1 PAD, while 5035 (8.2%) patients had Boix type 2 or 3 PAD. The chance of successful cannulation was lower in patients with type 1 PAD compared to no PAD (80.1% vs 88.7%; odds ratio: 0.42, 95% confidence interval: 0.38-0.46). No differences were seen in overall adverse events or post-ERCP pancreatitis. Adverse events occurred in 14.6% of patients with PAD type 1 and 16.0% of patients with PAD type 2 or 3, compared to 16.5% of patients without a PAD.
Conclusion: Cannulation appears less successful during ERCP when the papilla is located in the PAD (i.e., type 1). Adverse events seem not to increase with the presence of a PAD, but they could theoretically be influenced by the inability to cannulate.
Keywords: ERCP; adverse events; cannulation; duodenal diverticula; endoscopic retrograde cholangiopancreatography; periampullary diverticulum.
Plain language summary
How a pouch in the duodenum affects the difficulty and complications of an endoscopic procedure investigating the bile ducts A duodenal diverticulum (pouch in the duodenum) is a common finding during endoscopic examinations. A diverticulum can make it harder to do an ERCP, which is an endoscopic procedure that examines the bile ducts. The diverticulum might make it harder to do an ERCP because it affects the opening where the bile is released into the intestine. If the bile duct opening is inside the diverticulum, it is classified as type 1. If it is on the edge or outside, it is classified as type 2-3. This study used Swedish registry data to see if these types of diverticula make ERCP harder and cause more problems after the procedure. 47,486 procedures were investigated, and 12.1% had a diverticulum. A type 1 diverticulum makes ERCP harder. There was no difference in complications between the types of diverticula and no diverticulum. This means a diverticulum does not raise the risk of complications during ERCP. However, for a type 1 diverticulum, not being able to perform ERCP may prevent complications.
© The Author(s), 2024.
Conflict of interest statement
The authors declare that there is no conflict of interest.
Figures

Similar articles
-
Efficacy and safety of endoscopic retrograde cholangiopancreatography (ERCP) performed in patients with Periampullary duodenal diverticula (PAD).Clin Ter. 2014;165(4):e291-4. doi: 10.7417/CT.2014.1745. Clin Ter. 2014. PMID: 25203345
-
Effect of periampullary diverticulum morphology on ERCP cannulation and clinical results.Scand J Gastroenterol. 2025 Apr;60(4):292-299. doi: 10.1080/00365521.2025.2469121. Epub 2025 Feb 23. Scand J Gastroenterol. 2025. PMID: 39987936
-
Impact of periampullary diverticulum on biliary cannulation and ERCP outcomes: a single-center experience.Surg Endosc. 2021 Nov;35(11):5953-5961. doi: 10.1007/s00464-020-08080-8. Epub 2020 Oct 7. Surg Endosc. 2021. PMID: 33029732
-
Impact of periampullary diverticula on the rates of successful cannulation and ERCP complications: An up-to-date systematic review and meta-analysis.J Dig Dis. 2024 Sep-Oct;25(9-10):573-586. doi: 10.1111/1751-2980.13315. Epub 2024 Nov 18. J Dig Dis. 2024. PMID: 39557071
-
Endoscopic retrograde cholangiopancreatography in periampullary diverticulum: The challenge of cannulation.World J Gastrointest Endosc. 2016 Mar 25;8(6):282-7. doi: 10.4253/wjge.v8.i6.282. World J Gastrointest Endosc. 2016. PMID: 27014423 Free PMC article. Review.
Cited by
-
Combined Cholecystoenteric Fistula and Choledocholithiasis: A Report of a Rare Case.Cureus. 2024 Dec 30;16(12):e76608. doi: 10.7759/cureus.76608. eCollection 2024 Dec. Cureus. 2024. PMID: 39881910 Free PMC article.
-
Association of periampullary diverticulum types with post-ERCP hyperamylasemia: a retrospective observational study.BMC Gastroenterol. 2025 Apr 23;25(1):284. doi: 10.1186/s12876-025-03896-x. BMC Gastroenterol. 2025. PMID: 40269757 Free PMC article.
References
-
- Jayaraj M, Mohan BP, Dhindsa BS, et al.. Periampullary diverticula and ERCP outcomes: a systematic review and meta-analysis. Dig Dis Sci 2019; 64: 1364–1376. - PubMed
-
- Shemesh E, Klein E, Czerniak A, et al.. Endoscopic sphincterotomy in patients with gallbladder in situ: the influence of periampullary duodenal diverticula. Surgery 1990; 107: 163–166. - PubMed
-
- Chen L, Xia L, Lu Y, et al.. Influence of periampullary diverticulum on the occurrence of pancreaticobiliary diseases and outcomes of endoscopic retrograde cholangiopancreatography. Eur J Gastroenterol Hepatol 2017; 29: 105–111. - PubMed
-
- Ho JL, Seneviratna A, Yip CHB. Impact of periampullary diverticulum on biliary cannulation: a retrospective cohort study. Adv Dig Med 2023; 10: 232–239.
LinkOut - more resources
Full Text Sources

